When someone receives a diagnosis like bipolar disorder, schizophrenia, severe OCD, or even autism, they’re usually told it’s a lifelong condition. They’re given medications to manage symptoms and counseled to accept that this is simply how their brain works. Parents are told their children will always struggle. Adults are told to adjust their expectations for life.
But what if that’s not the whole story?
A growing body of medical research is revealing something that could change everything for millions of people: many psychiatric conditions have underlying biological causes that can be identified through testing and, in many cases, successfully treated. These aren’t exotic theories. They’re published in peer-reviewed medical journals and supported by clinical evidence showing patients who were told they’d never recover achieving complete remission once the real problem was found and addressed.
The troubling reality is that most patients are never tested for these causes. They receive a diagnosis based on their symptoms, start medication, and that’s where the investigation ends. The deeper question, “What’s actually causing this?” often goes unasked.
This article explores what the research shows about the hidden biological triggers behind many brain disorders, and why finding them could be the difference between a lifetime of managing symptoms and actually getting better.
Hidden Infections That Affect the Brain
One of the most surprising findings in recent psychiatric research is how often chronic infections play a role in mental health conditions. We’re not talking about being sick with the flu. We’re talking about infections that take up residence in the body, often without obvious symptoms, and quietly interfere with brain function for years.
Common Viruses With Uncommon Effects
Most adults have been exposed to herpes simplex virus (the kind that causes cold sores) and Epstein-Barr virus (the one behind mono). These viruses never fully leave the body. They go dormant, but they can reactivate periodically, and when they do, they trigger inflammation that affects the brain.
Research published in Frontiers in Psychiatry found that over 90% of people with schizophrenia tested positive for Epstein-Barr virus, compared to about 79% of healthy people. That might not sound like a huge difference, but statistically it’s highly significant. More importantly, the viral presence was linked to higher levels of inflammation in the body, and that inflammation correlated with worse symptoms.
Similar patterns show up in bipolar disorder, where herpes simplex virus is found at elevated rates. The virus appears to interfere with brain receptors involved in mood regulation.
Even more striking: when a mother is infected with herpes during pregnancy, her child has roughly double the risk of developing depression and a significantly higher risk of psychotic disorders later in life. The timing of infection matters enormously for brain development.
Tick-Borne Infections: The Overlooked Epidemic
Perhaps the most dramatic findings involve tick-borne infections: Lyme disease (Borrelia), Babesia, and Bartonella. These bacteria and parasites are increasingly being found in patients with psychiatric diagnoses, often at remarkably high rates.
North Carolina State University researchers found Bartonella bacteria in the blood of 43% of adults with psychosis, compared to just 14% of healthy people. These patients often had no idea they’d ever been bitten by a tick or flea (which also transmits Bartonella).
In children, the numbers are even more striking. A study of 37 kids diagnosed with pediatric bipolar disorder found that 92% showed evidence of tick-borne infection. Over half had Babesia, nearly half had Bartonella, and about a quarter had Lyme disease. Many had multiple infections at once.
Here’s what makes this so important: case reports document patients with severe, treatment-resistant psychiatric symptoms who recovered completely after receiving appropriate antibiotic and antiparasitic treatment. Some were able to stop all their psychiatric medications. These weren’t minor improvements. These were people getting their lives back.
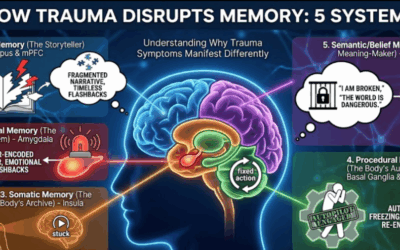
When the Immune System Attacks the Brain
Sometimes infections trigger an autoimmune response where the body’s immune system mistakenly attacks brain tissue. This is the mechanism behind PANDAS, where strep throat triggers sudden-onset OCD or tics in children. But it’s not just strep. Other infections including Toxoplasma (the parasite from cat litter) can cause similar problems by forming cysts in the parts of the brain that control impulses and repetitive behaviors.
In children with autism, researchers have found significantly higher rates of herpes antibodies along with antibodies that attack brain tissue itself. Nearly all the autistic children with herpes antibodies also had antibodies targeting their own amygdala and hippocampus, brain regions crucial for emotion and memory. This suggests the virus may be triggering an autoimmune attack on the brain, a potentially treatable condition that’s rarely even looked for.
Environmental Toxins and Brain Health
We hear a lot about “chemical imbalances” in the brain causing mental illness. But there’s growing evidence that actual chemicals, toxins from our environment, play a much larger role than most doctors acknowledge.
Parkinson’s Disease: A Case Study in Toxic Exposure
Parkinson’s disease is now the fastest-growing brain disorder in the world. Only about 15% of cases run in families. The rest appear to be caused primarily by environmental factors.
The numbers are alarming. Exposure to the weed killer paraquat increases Parkinson’s risk by 150%. It’s banned in over 30 countries but still widely used in the United States. Even worse is a common industrial solvent called TCE (trichloroethylene), used in dry cleaning and degreasing. TCE exposure increases Parkinson’s risk by 500%. This chemical contaminates up to 30% of U.S. groundwater and can seep into homes and schools from underground.
Research from the American Parkinson Disease Association shows that pesticide exposure causes lasting changes to brain genes, creating a kind of “molecular memory” that makes brain cells more vulnerable to degeneration years or even decades later. This means Parkinson’s isn’t really a disease of aging. It’s a disease of accumulated toxic exposure, which means it’s potentially preventable.
Aluminum and Brain Degeneration
Aluminum has no useful function in the human body, but it’s everywhere: in cookware, food additives, antacids, and some vaccines. For most people, the body handles it fine. But for those with genetic vulnerabilities in their detoxification systems, aluminum can accumulate in the brain over time.
A 36-year research program has consistently found elevated aluminum levels in the brains of people with Alzheimer’s disease. The metal promotes the formation of the plaques and tangles characteristic of the disease and damages the brain’s protective barriers.
The key point: some people have genetic variants that make them poor detoxifiers. For these individuals, everyday aluminum exposure that wouldn’t bother most people can push them past a threshold into brain damage. This is testable, and for those at risk, it’s potentially actionable through avoidance and detoxification support.
Genetic Factors That Make Everything Harder
Not everyone responds to infections and toxins the same way. Your genes determine how well your body handles these challenges, and certain common genetic variants can make you much more vulnerable.
The MTHFR Gene: Why Some People Can’t Use Their Vitamins
You may have heard of MTHFR. It’s a gene that controls how your body processes B vitamins, particularly folate. This process is essential for making neurotransmitters like serotonin, dopamine, and norepinephrine, the very chemicals most psychiatric medications target.
About 10-15% of the population has a variant that reduces this gene’s function to just 25% of normal. A review of 81 studies confirmed that this MTHFR variant is significantly associated with schizophrenia and major depression.
Here’s the practical problem: people with this variant often show normal or even high B12 levels on standard blood tests, but their bodies can’t actually use the vitamin in its standard form. They have a functional deficiency despite “normal” lab results. This is easily addressed with the right form of supplementation once you know to look for it.
Glutathione: Your Body’s Master Detoxifier
Glutathione is your body’s most important antioxidant and detoxification molecule. It neutralizes toxins, fights oxidative stress, and protects brain cells. The MTHFR variants mentioned above can slash glutathione production by up to 90%.
In autism, low glutathione levels appear to be a key factor in why symptoms develop. When glutathione is depleted, the brain becomes hypersensitive to toxins and infections it would normally handle. Supplementing with NAC (N-acetyl cysteine), which the body uses to make glutathione, has been shown to reduce irritability in autistic children by 80%.
Other genetic variants affecting glutathione have been linked to conditions like Tourette syndrome. Again, these are testable factors that can guide treatment.
Iron Overload in the Brain
Iron is essential for brain function, but too much is toxic. Some people carry genetic variants that cause iron to accumulate in the brain, especially in men. This excess iron promotes the formation of the abnormal proteins seen in Alzheimer’s and Parkinson’s disease and increases oxidative stress.
Testing for iron status and these genetic variants should be standard practice for anyone with cognitive decline or movement symptoms, but it rarely is.
The Good News: These Conditions Can Often Improve
If all of this sounds overwhelming, here’s the hopeful part: when these underlying causes are found and addressed, conditions that were considered permanent sometimes turn out not to be.
Reversing Cognitive Decline
Dr. Dale Bredesen has developed an approach called the ReCODE protocol that addresses over 36 different factors contributing to Alzheimer’s disease, including infections, toxins, nutrient deficiencies, and metabolic problems.
His published research shows cognitive decline reversing in the majority of patients who follow the protocol. One patient’s hippocampus (the memory center of the brain) went from the 17th percentile to the 75th percentile after ten months. The brain wasn’t just stopping its decline. It was rebuilding.
Bredesen’s theory is that what we call “Alzheimer’s” is often the brain’s protective response to various biological threats. Remove the threats, and the brain can begin to recover.
Metabolic Approaches to Mental Illness
A movement called Metabolic Psychiatry is showing that many mental health conditions may be fundamentally problems of brain energy. When brain cells can’t get enough fuel, they malfunction in ways that look like bipolar disorder, schizophrenia, or depression.
The ketogenic diet, which shifts the brain’s fuel source from glucose to ketones, has produced remarkable results in treatment-resistant cases. Some patients with severe mental illness have achieved complete remission through dietary changes alone. This represents a fundamental shift in how we understand these conditions.
Recovery From Infection-Driven Psychosis
Perhaps most dramatic are the cases where psychosis, considered one of the most serious psychiatric conditions, resolves completely with antibiotic treatment.
One published case report describes a 14-year-old boy with sudden-onset psychotic behavior that didn’t respond to any psychiatric medication. Testing revealed Bartonella infection. After appropriate antimicrobial treatment, he recovered completely and stopped all psychiatric medications.
Another case involved a patient with severe OCD who recovered fully after treatment for Lyme disease. A series of ten patients with late-stage tick-borne neurological disease achieved complete remission with long-term antibiotic and antiparasitic treatment.
These cases suggest something important: what looks like “treatment-resistant” mental illness may simply be “incompletely diagnosed” mental illness.
Why Isn’t Everyone Being Tested?
If these underlying causes are so common and so treatable, why aren’t they part of standard psychiatric evaluation?
Part of the answer is historical. Psychiatry developed as a field separate from the rest of medicine, with its own diagnostic categories based on symptoms rather than causes. A patient who hears voices gets diagnosed with schizophrenia. A patient with mood swings gets diagnosed with bipolar disorder. The diagnosis describes what’s happening but not why.
Part of the answer is practical. The tests for these underlying factors aren’t always straightforward or covered by insurance. They require thinking about mental health in a different way than most clinicians were trained.
But the ethical implications are serious. Telling someone their condition is permanent without first ruling out treatable causes denies them information they need to make informed decisions about their care. The basic principles of medical ethics require that we do no harm and that we act in patients’ best interests. As the evidence for these biological triggers grows, the failure to look for them becomes harder to justify.
What This Means For You
If you or someone you love has been diagnosed with a chronic psychiatric or neurological condition, especially one that isn’t responding well to standard treatment, it may be worth asking some questions:
Has anyone tested for chronic infections? This includes not just standard blood tests but specialized testing for tick-borne diseases, which often don’t show up on routine screening.
Has anyone assessed environmental exposures? This might include testing for heavy metals, reviewing occupational history, and checking whether you’ve lived in areas with known groundwater contamination.
Has anyone looked at relevant genetic factors? MTHFR testing is increasingly available and can reveal whether you might benefit from specific forms of B vitamins. Other genetic tests can identify vulnerabilities in detoxification and iron metabolism.
Has anyone considered metabolic factors? Blood sugar regulation, insulin resistance, and mitochondrial function all affect brain health and can be assessed and addressed.
Finding a practitioner who thinks this way can be challenging. Functional medicine doctors, integrative psychiatrists, and some naturopathic physicians are more likely to investigate these factors. The key is working with someone willing to ask “why” rather than just “what.”
A Different Kind of Hope
None of this means that every psychiatric condition has a hidden treatable cause waiting to be discovered. Biology is complicated, and sometimes the answers aren’t simple. But the research increasingly suggests that many people currently living with “permanent” diagnoses might have options they’ve never been told about.
The question isn’t whether to abandon psychiatric treatment. It’s whether to expand the investigation before concluding that symptoms are all that can be addressed. For some patients, the difference between finding the underlying cause and missing it is the difference between a lifetime of disability and genuine recovery.
That possibility, even if it doesn’t apply to everyone, seems worth pursuing.
Joel is a Licensed Independent Clinical Social Worker (LICSW-S) and Clinical Director of Taproot Therapy Collective in Birmingham, Alabama. His practice integrates depth psychology, neuroscience, and holistic approaches in the treatment of complex presentations, with a commitment to exploring root causes alongside symptom management.


















0 Comments