Executive Summary: The Neurobiology of Insight
The Mechanism: Vipassana acts as a neural “interrupter,” breaking the feedback loop between the Amygdala (fear center) and the Default Mode Network (rumination). It forces the brain to process “bottom-up” somatic data rather than “top-down” narratives.
The Clinical Verdict: While highly effective for rewiring the traumatized brain’s response to stress, it carries a risk of flooding. Without a sufficient “Window of Tolerance,” the silence can amplify dissociation rather than cure it.
Key Studies Cited: Lazar et al. (Harvard) on cortical thickness; Brewer et al. (Yale) on the Default Mode Network; Van der Kolk on the breakdown of the Thalamus.
Is Vipassana What I Need to Heal Trauma? A Neurobiological and Depth Psychological Analysis
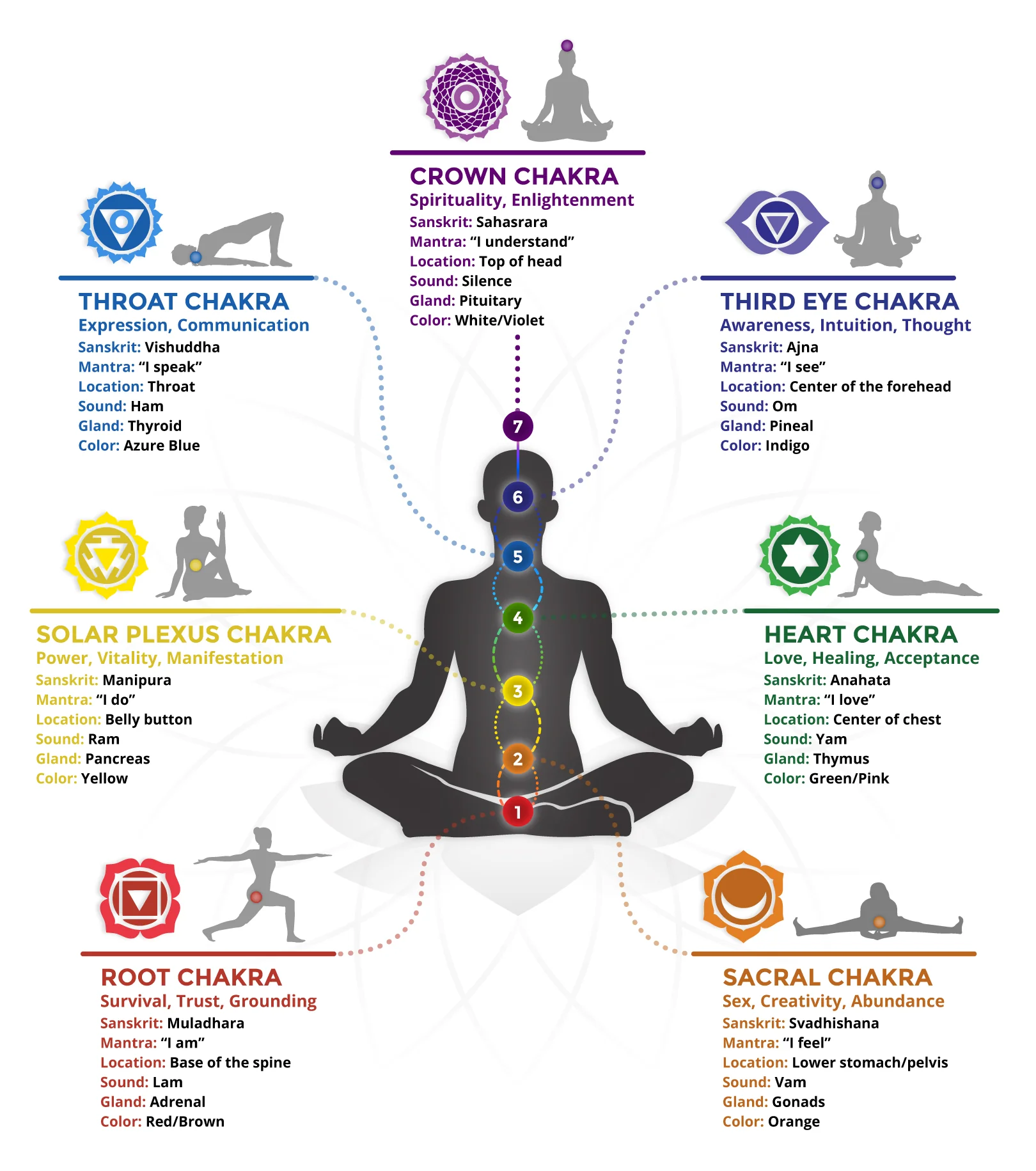
In the clinical treatment of Complex PTSD (C-PTSD) and developmental trauma, talk therapy often hits a wall. This is because trauma is not stored in the broca’s area (the language center); it is encoded in the Limbic System and the fascia of the body. Vipassana meditation, an ancient technique of “body scanning,” has gained attention as a somatic intervention that bypasses the verbal brain entirely.
However, from a neurobiological perspective, Vipassana is not “relaxation.” It is a rigorous form of exposure therapy that targets the neural correlates of reactivity. Before undertaking a 10-day silent retreat, one must understand the mechanics of how this practice interacts with a traumatized nervous system.
The Neuroscience of “Sankharas”: Implicit Memory and the Body
In Vipassana theory, trauma is described as Sankharas—conditioned reactions of craving or aversion stored in the body. Modern neuroscience validates this via the concept of Implicit Memory.
1. The Thalamic Breakdown
Trauma expert Bessel van der Kolk has demonstrated that during trauma, the Thalamus (the brain’s cook) stops functioning correctly. It fails to integrate sensory input into a coherent autobiographical memory. Instead, the memory is fragmented into isolated somatic sensations: a tight chest, a flash of heat, a pit in the stomach.
Vipassana directs the practitioner to scan the body for these fragmented sensations. By observing them without reacting (Equanimity), the brain is forced to re-integrate these isolated sensory fragments back into the conscious timeline, effectively “metabolizing” the stuck trauma.
2. Shrinking the Amygdala (The Alarm Bell)
A landmark study by Sara Lazar at Harvard Medical School (2011) utilized fMRI scans to show that 8 weeks of mindfulness practice actually shrank the gray matter volume of the Amygdala. The Amygdala is the brain’s “smoke detector,” responsible for the fight-or-flight response. In trauma survivors, the Amygdala is chronically enlarged and hyperactive.
Simultaneously, the study found increased cortical thickness in the Prefrontal Cortex (PFC)—the area responsible for executive function and emotional regulation. This suggests that Vipassana physically rewires the brain to turn down the volume on fear while turning up the volume on rationality.
The Default Mode Network: Breaking the Cycle of Rumination
Trauma survivors often suffer from an overactive Default Mode Network (DMN). This is the network of brain regions active when we are not focused on the outside world—it is the “storyteller” that constantly rehearses the past and fears the future.
Research by Judson Brewer (Yale) indicates that experienced meditators show significantly reduced activity in the DMN. By anchoring attention in the body (bottom-up processing), Vipassana inhibits the DMN (top-down processing). This creates a “gap” in the stream of depressive rumination, allowing the True Self (or Witness Consciousness) to emerge.
The Danger Zone: The Window of Tolerance
While the neurology is promising, the clinical reality is complex. Dr. David Treleaven, author of Trauma-Sensitive Mindfulness, warns that meditation can backfire if the survivor’s Window of Tolerance is exceeded.
Interoceptive Exposure
Vipassana relies on Interoception—the ability to feel the internal state of the body. The Insula is the part of the brain that monitors these internal signals.
* Hypo-arousal: Many trauma survivors are dissociated (numb). They have low Insula activity.
* Hyper-arousal: Others are flooded with panic. They have high Insula activity.
If a survivor with a history of severe dissociation attempts intense Vipassana, the silence may strip away their coping mechanisms, leading to Flooding or Re-traumatization. This is why we often recommend Somatic Experiencing first, to build the capacity to feel safe in the body before attempting deep immersion.
A Jungian Perspective: The Alchemical Work
From a depth psychological perspective, Vipassana is a confrontation with the Shadow. The “impurities” that rise to the surface during a retreat are the repressed contents of the unconscious.
- The Nigredo: The early days of a retreat often mirror the alchemical stage of Nigredo (The Blackening), where the Ego is broken down, and dark emotions (rage, grief, terror) surface.
- The Witness: The goal is to cultivate the “Observer Self.” This aligns with Jung’s concept of the Self—the center of the psyche that can hold the tension of opposites without breaking.
Conclusion: Is It Right for You?
Vipassana is a potent neurobiological intervention. It does not just “soothe” stress; it structurally alters the brain’s fear circuitry. However, it is surgery, not a massage. It requires a baseline of ego-strength to endure.
If you are currently in acute crisis or actively dissociated, we recommend starting with Neurofeedback or Trauma-Informed Therapy to stabilize the nervous system. Once the Window of Tolerance has widened, Vipassana can be the vehicle that takes you from managing symptoms to truly dissolving them.
Scientific References & Further Reading
- Hölzel, B. K., Carmody, J., Vangel, M., Congleton, C., Yerramsetti, S. M., Gard, T., & Lazar, S. W. (2011). Mindfulness practice leads to increases in regional brain gray matter density. Psychiatry Research: Neuroimaging.
- Brewer, J. A., Worhunsky, P. D., Gray, J. R., Tang, Y. Y., Paquette, J., & Craik, F. I. (2011). Meditation experience is associated with differences in default mode network activity and connectivity. PNAS.
- Van der Kolk, B. A. (2014). The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma. Viking.
- Treleaven, D. A. (2018). Trauma-Sensitive Mindfulness: Practices for Safe and Transformative Healing. W. W. Norton & Company.



















0 Comments