The Biology of Safety: A Somatic Guide to Polyvagal Theory
For most of the history of psychology, we treated the nervous system like a simple toggle switch. We believed we were either stressed or calm, in “fight or flight” or “rest and digest.” But any therapist who has sat with a client frozen in grief, or a trauma survivor who cannot speak, knows this binary model fails to capture the complexity of human suffering. It was not until 1994, when Dr. Stephen Porges introduced the Polyvagal Theory, that we finally had a map for the gray areas of our biology. Porges revealed that our nervous system is not a switch, but a hierarchy—a complex evolutionary ladder that dictates how we connect, how we defend ourselves, and ultimately, how we heal.
At its core, Polyvagal Theory shifts the conversation from “what is wrong with you?” to “how is your body trying to save you?” It explains that our behaviors—whether it is the rage of a panic attack or the numbness of dissociation—are not character flaws. They are physiological states. As a clinician practicing Somatic Experiencing regarding trauma, I have found that understanding this biological hierarchy is often the first step in reducing the shame clients feel about their own reactions. When we understand the Vagus Nerve, we stop fighting our biology and start learning to regulate it.
The Three States of the Autonomic Ladder
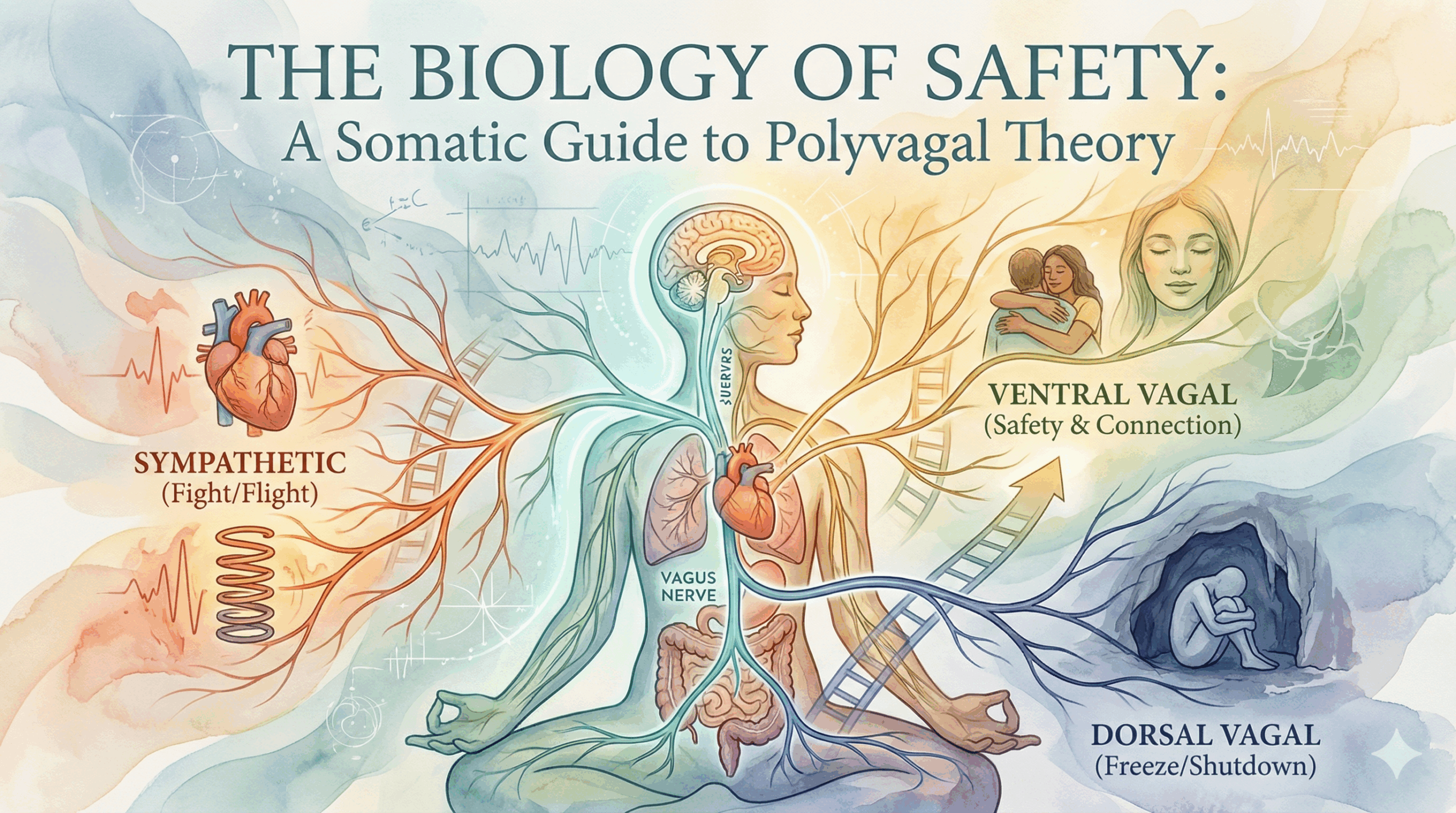
Porges identified that the Vagus Nerve, the tenth cranial nerve which wanders from the brainstem to the gut, has two distinct branches. These branches, along with the sympathetic nervous system, create three distinct physiological states. We move through these states in a predictable order, often without conscious awareness, a process Porges termed “Neuroception.”
[Image of autonomic nervous system diagram]
The first and most evolved state is the Ventral Vagal state. This is the state of social engagement and safety. Biologically, the myelinated ventral vagus nerve acts as a “brake” on the heart, allowing us to remain calm and connected. In this state, we can read facial expressions, listen to the prosody (tone) of a voice, and feel a sense of agency. This is the physiological requirement for intimacy and play. When we define what trauma really is, we are essentially describing the chronic loss of this state.
When our neuroception detects danger, we slide down the ladder into the Sympathetic state. This is the familiar “fight or flight” mobilization. The “vagal brake” releases, the heart rate accelerates, and blood shunts to our muscles. In therapy, we see this as anxiety, rage, or frantic energy. It is an adaptive mobilization response designed to get us away from a threat.
But if fighting or fleeing is impossible—if the threat is too great or we are trapped—we drop to the bottom of the ladder: the Dorsal Vagal state. This is the most primitive defense, shared with reptiles. It is total immobilization. We freeze, collapse, or dissociate. In this state, the body conserves energy to survive, slowing the heart and metabolism. This is the state of “shame,” depression, and the “checkout” often seen in complex PTSD. Crucially, you cannot think your way out of a Dorsal state; you must sense your way out.
The Brain-Body Connection and Neuroception
One of the most radical contributions of Polyvagal Theory is the concept of “Neuroception.” Unlike perception, which is a conscious cognitive process (e.g., “I see a snake”), neuroception is the subconscious detection of safety or threat by the neural circuits. It happens before we have a thought. This explains why trauma survivors often feel unsafe even when they are cognitively aware that they are in a safe room. Their body has detected a cue—a sound, a smell, a tone of voice—that signals “predator,” and the autonomic state shifts instantly.
This biological reality is why top-down therapies (like CBT) often fail with deep trauma. You cannot talk a brainstem out of a survival state. This is where we must bridge the gap between talk therapy and body-based approaches. In my practice, I often refer to the brain-body connection in Somatic Experiencing as the primary mechanism for change. By working with the felt sense—the physical sensations of the body—we can communicate directly with the nervous system, bypassing the logic centers that go offline during stress.
Clinical Practice: Co-Regulation and the Therapeutic Container
The implications of Polyvagal Theory for clinical practice are profound. It suggests that safety is not the absence of threat, but the presence of connection. This fundamentally changes how we approach therapy. In a traditional talk therapy model, we might ask a client to cognitively process a traumatic event. But if that client is in a Dorsal Vagal freeze, their “social engagement system” is offline. They physically cannot process relational safety. Asking them to talk in this state is like trying to download a file to a computer that has no wifi connection.
Instead, Polyvagal-informed therapy prioritizes “Co-Regulation.” This is the biological imperative that mammals need another nervous system to help them regulate their own. As therapists, our own ventral vagal state becomes the anchor. We use tone of voice, prosody, and grounded presence to signal safety to the client’s neuroception. We are not just listening to their words; we are speaking to their brainstem. This is why approaches like Brainspotting and EMDR are so effective; they provide a container where the client’s nervous system can safely discharge survival energy while tethered to the therapist’s regulated presence.
For example, when a client begins to dissociate (Dorsal Vagal) during a session, we pause the narrative. We might use orienting exercises—asking them to look around the room and name three blue objects. This simple act engages the neck and eye muscles, which are innervated by the Ventral Vagal complex, effectively stimulating the system to come back online. We are physically recruiting the nerves of safety.
The Role of Attachment and Early Development
Our autonomic settings are shaped early in life. If an infant cries and is met with a soothing parent (Co-regulation), their nervous system learns that distress is temporary and that they can return to safety. This builds “Vagal Tone”—resilience. However, if a child is met with neglect or abuse, their nervous system learns that the world is dangerous. They may become chronically stuck in Sympathetic arousal (anxious attachment) or Dorsal collapse (avoidant/disorganized attachment).
This early programming often follows us into adulthood. We see this clearly in how the Jungian Anima and Animus show up in relationships. The “Anima” often carries the emotional load of our unmet needs for connection, while the “Animus” may represent our capacity for boundaries and protection. When these archetypes are wounded, our nervous system reacts to intimacy as a threat. Polyvagal Theory gives us a biological language for these archetypal patterns, explaining why we might sabotage a safe relationship because our body misinterprets “calm” as “boring” or “unsafe.”
Self-Help: Moving Up the Ladder
For clients outside the therapy room, the goal is not to stay in Ventral Vagal 100% of the time—that is impossible. The goal is flexibility: the ability to move up and down the ladder without getting stuck. Porges calls this “Vagal Tone.” Just as we exercise muscles, we can exercise our nervous system.
One powerful tool for self-regulation is the use of sound. The Vagus Nerve passes through the vocal cords and the inner ear. Humming, chanting, or singing can physically stimulate the nerve and engage the “vagal brake.” This is why “Om” chanting has been used for millennia to induce calm. It is a biological hack for the nervous system, remarkably similar to Jungian Somatic Meditation techniques that use breath and sound to integrate the shadow.
Another accessible tool is the “Physiological Sigh”—two quick inhales through the nose followed by a long, slow exhale through the mouth. This specific breathing pattern offloads carbon dioxide and mechanically triggers the heart to slow down. It is a manual override for the Sympathetic “fight or flight” response. Recognizing where you are on the ladder is the first step. If you are angry (Sympathetic), you need movement to discharge that energy. If you are numb (Dorsal), you need gentle sensory stimulation to wake up.
Trauma and the Deep Brain
We often ask “why” we behave the way we do, looking for a logical reason. But trauma lives in the deep brain, far below the reach of logic. Finding the roots of trauma in the deep brain requires us to respect the intelligence of our survival mechanisms. The part of you that freezes when your boss raises their voice is not “weak”; it is a highly skilled survivalist that once kept you safe from a dangerous parent. Polyvagal Theory invites us to thank these defenses rather than pathologize them.
This perspective is crucial when working with complex conditions like Dissociative Identity Disorder (DID). In many ways, DID is the ultimate creative adaptation of the Polyvagal system, compartmentalizing overwhelming trauma into separate states of consciousness to survive. Tools like DID alter mapping allow us to see how different “alters” often correspond to different autonomic states—a “fight” part holding the Sympathetic rage, and a “little” part holding the Dorsal freeze.
Legacy and Influence
The introduction of Polyvagal Theory was a paradigm shift that bridged the gap between neurobiology and psychology. Before Porges, “trauma” was often viewed purely as a psychological wound. Polyvagal Theory provided the physiological evidence that trauma is an injury to the nervous system. This validated the experiences of millions of survivors who felt “crazy” for their physical symptoms.
This theory has become the bedrock for modern somatic therapies. It provides the mechanism of action for EMDR (Eye Movement Desensitization and Reprocessing), helping explain how bilateral stimulation keeps clients in a window of tolerance. It is the foundation of Deb Dana’s clinical work, which translated Porges’ dense academic theory into practical exercises for therapists. It has also influenced the treatment of autism, highlighting how auditory hypersensitivity is often a result of a nervous system stuck in a defensive state, unable to filter out background noise.
Timeline of Polyvagal Theory
- 1994: Dr. Stephen Porges introduces the Polyvagal Theory in his presidential address to the Society for Psychophysiological Research, challenging the paired antagonism model of the Autonomic Nervous System. View the original concept context.
- 2011: Publication of “The Polyvagal Theory: Neurophysiological Foundations,” compiling decades of research into a comprehensive volume for the scientific community. View Publisher Page.
- 2018: Deb Dana publishes “The Polyvagal Theory in Therapy,” officially bridging the gap between academic research and clinical application for social workers and counselors. See Deb Dana’s Resources.
- 2020s: Research expands into the “Science of Safety,” exploring how Polyvagal principles apply to education, social justice, and long-COVID treatment. Read the “Science of Safety” NIH Paper.
Bibliography
- Porges, S. W. (2011). The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-regulation. W. W. Norton & Company. Link to Publisher
- Dana, D. (2018). The Polyvagal Theory in Therapy: Engaging the Rhythm of Regulation. W. W. Norton & Company. Link to Book Resource
- Porges, S. W. (2022). Polyvagal Theory: A Science of Safety. Frontiers in Integrative Neuroscience. Link to Full Text at NIH
- Levine, P. A. (2010). In an Unspoken Voice: How the Body Releases Trauma and Restores Goodness. North Atlantic Books. Link to Book Resource
- Van der Kolk, B. A. (2014). The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma. Viking. Link to Author Page
Legacy and Influence
The legacy of Stephen Porges and the Polyvagal Theory is the re-humanization of clinical practice. By proving that our need for safety is biological, not just psychological, he has influenced an entire generation of “bottom-up” therapies. His work laid the groundwork for the current explosion of interest in somatic psychology, vagus nerve stimulation technology, and trauma-informed care in schools. Models like Internal Family Systems (IFS) now regularly integrate Polyvagal language, helping clients map their “parts” to their autonomic states. Ultimately, Porges gave us the science to prove what the heart always knew: we are wired for connection, and we heal in relationship.





















0 Comments