In the wellness world, mindfulness is marketed as a universal cure-all. We are told that if we just sit still, close our eyes, and watch our breath, our anxiety will dissolve. For many people, this is true. But for trauma survivors, this advice can be dangerous. It is not uncommon for a person with complex PTSD to try meditation and find themselves suddenly flooded with terror, dissociated (“floating away”), or physically shaking.
This is not because they are “doing it wrong.” It is because standard mindfulness practices were originally designed for monks living in monasteries—people who had already established a high degree of safety and regulation. They were not designed for a nervous system stuck in a chronic freeze response. If you have tried to meditate and felt worse, you need to know: It is not your fault, and there is a safer way.
The “Window of Tolerance” and the Trap of Silence
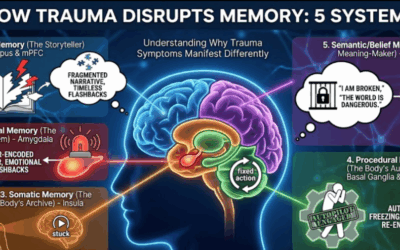
Trauma is, by definition, an experience of being overwhelmed. To survive it, the brain often walls off the sensations of the body (dissociation). When you sit in silence and turn your attention inward without “guardrails,” you risk tearing down that wall too quickly. You may be plunged into the abyss of the trauma before you have the tools to handle it.
This phenomenon is well-documented in the work of researchers like Dr. Willoughby Britton (who studies adverse effects of meditation) and trauma experts like David Treleaven. For a hyper-aroused nervous system, silence isn’t peaceful; it’s threatening. The lack of external sensory input forces the brain to amplify internal signals—the racing heart, the tight chest—which can trigger a panic loop.
Trauma-Sensitive Mindfulness: How to adapt the Practice
The goal isn’t to stop being mindful; it is to modify the practice so it remains within your “Window of Tolerance.” Robin Taylor, LICSW-S specializes in teaching trauma-informed mindfulness. Here are the key adjustments we use in therapy:
1. Keep Your Eyes Open (Orienting)
Closing your eyes cuts off your primary safety system: vision. If closing your eyes makes you feel floaty or anxious, keep them open. Soften your gaze and look at a spot on the floor, or actively look around the room. This is called “Orienting.” By seeing that you are in a safe room, you signal to your amygdala that you are here, now, not back there, then.
2. Focus on External Anchors
Standard meditation focuses on the breath. But for many trauma survivors, the breath is a trigger (it is where we hold anxiety). Instead of watching your breath, focus on an external anchor. The sound of a fan. The feeling of your feet on the floor. The texture of a blanket. This keeps you grounded in the present reality without forcing you to interocept (look inside) too deeply, too soon.
3. Titration (The “Toe-Dip” Method)
Do not try to meditate for 20 minutes. Start with 30 seconds. Touch the stillness, then immediately return to activity. We call this Pendulation. You swing between a state of rest and a state of engagement. Over time, your nervous system learns that it can enter stillness and come back out safely. This builds capacity without flooding.
4. Moving Mindfulness
Stillness can feel like “Freeze” to a traumatized body. Movement can break that association. Try walking meditation, swaying while you sit, or doing gentle stretching. Thich Nhat Hanh famously taught that mindfulness can be found in washing dishes or walking slowly. If your body needs to move to feel safe, let it move.
From Dissociation to Embodiment
The ultimate goal of mindfulness in trauma therapy is not transcendence (leaving the body); it is embodiment (safely inhabiting the body). This is a slow process. It involves reclaiming the body inch by inch, respecting the defenses that are there for a reason.
If you have felt alienated by the “just breathe” culture of modern wellness, we invite you to try a different approach. At our clinic, we don’t just hand you a meditation app. We work with you to build a customized, somatic toolkit that respects your history and your nervous system’s unique needs.
Ready to find safety in stillness? Schedule a session with Robin Taylor, LICSW-S, to learn trauma-informed mindfulness tools that actually work for you.





















0 Comments