If you’ve been searching “maternal mental health laws Alabama” or “postpartum screening mandatory” and feeling your heart race, you’re not alone. Rumors are spreading about forced screenings, new medications, and DHR interventions. As a Birmingham-based therapy clinic, we’ve done the deep research—digging through actual legislation, Medicaid policy documents, and DHR protocols—to separate internet fears from legal facts. Here’s the truth about your rights as a mother in Alabama.
The Headlines vs. The Reality: What You Need to Know Right Now
Before we dive deep, here’s the core message you need to hear:
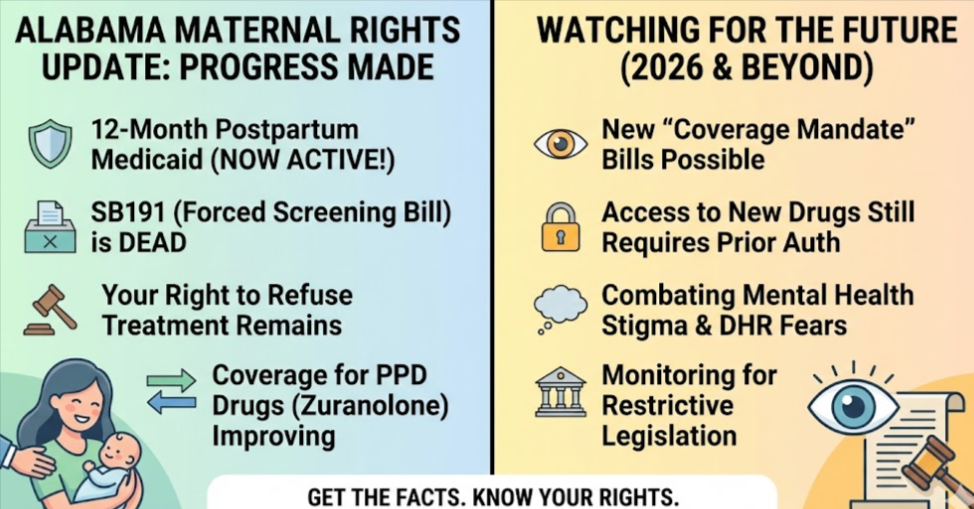
You are seeing scary headlines, but the reality in Alabama is currently one of expanded support, not stripped rights. New laws have been trying to get insurance to pay for your care, not force you into it. You still have the absolute right to say no.
Now let’s break down exactly what’s happening, what it means for you, and what your rights are.
Part One: The “Boogeyman” Bill—What Actually Happened with SB191
The Fear
Social media posts and worried conversations have spread claims that Alabama passed a law forcing mothers to be screened for postpartum depression, that a “bad” screening result could lead to immediate Child Protective Services involvement, and that mothers would be medicated against their will.
The Reality
Senate Bill 191 is dead. It was introduced during the 2025 Legislative Session but was “Indefinitely Postponed” on May 6, 2025, and did not become law. In Alabama legislative procedure, indefinite postponement effectively kills a bill for the remainder of the session.
More importantly, even if SB191 had passed, it was never designed to force anything on mothers. The bill was a coverage mandate for insurance, not a treatment mandate for mothers. Here’s what the bill actually proposed:
- Required Alabama Medicaid to pay for PPD screenings—meaning doctors would get reimbursed for offering screenings, making them more available
- Prohibited insurance companies from denying coverage for PPD medications like Zuranolone
- Banned “step therapy” requirements—which currently force mothers to fail on cheaper antidepressants before accessing newer, more effective treatments
The bill explicitly stated that healthcare professionals “shall exercise professional judgment” in recommending treatment. It contained no provision requiring mothers to accept screening or medication.
Why This Matters
The failure of SB191 actually means that supportive infrastructure for maternal mental health did not advance. There is still no statutory mandate requiring PPD screening in Alabama—providers retain full discretion over whether to screen, which tools to use, and how to follow up. The restrictive Medicaid policies that make accessing new treatments difficult remain in place.
Part Two: Understanding Zuranolone—The New PPD Medication
What Is Zuranolone (Zurzuvae)?
Zuranolone represents a genuine breakthrough in postpartum depression treatment. Unlike traditional antidepressants that can take six to eight weeks to show effectiveness, Zuranolone is a neuroactive steroid specifically designed for PPD that works within a 14-day course. It’s the first oral medication specifically approved for postpartum depression.
The Fear
Some mothers worry this new drug will be forced on them or that doctors will push it as a first-line treatment.
The Reality
Zuranolone is actually extremely difficult to access in Alabama, not easy. Alabama Medicaid has implemented one of the most restrictive coverage policies in the nation—a “fail-first” or “step therapy” protocol that requires patients to try and fail two different generic antidepressants before Medicaid will authorize coverage for Zuranolone.
This means:
- A standard antidepressant trial lasts four to six weeks to determine efficacy
- Requiring two trials imposes a minimum delay of eight to twelve weeks
- By the time Zuranolone is approved, much of the critical postpartum window has passed
- Even after meeting these requirements, doctors must complete extensive Prior Authorization paperwork (Form 369) documenting the failed medications
No one is handing out Zuranolone casually. If anything, mothers who want access to this medication face significant bureaucratic barriers.
Part Three: The Good News—Medicaid Expansion You Should Know About
Here’s something that often gets lost in the fearful conversations: Alabama has made a significant positive change for maternal healthcare.
Alabama has permanently adopted the 12-month postpartum Medicaid extension.
Under the old law, Medicaid coverage ended 60 days after birth—right when many mothers are just beginning to recognize symptoms of postpartum depression or anxiety. Under the current law, full Medicaid benefits continue for 12 months after delivery.
This is a massive win for maternal rights in Alabama. It means:
- Access to therapy and mental health care for a full year postpartum
- Continued coverage for psychiatric medications if needed
- Time to establish care relationships with providers
- Coverage that recognizes the “fourth trimester” and beyond as a vulnerable period
Part Four: DHR, Mandatory Reporting, and Your Rights—The Hard Truths
This is where we need to have a frank conversation. The intersection of mental health and child welfare in Alabama is complex, and understanding your rights requires understanding the system.
What Mandatory Reporting Actually Means
Alabama’s mandatory reporting laws require healthcare providers, therapists, social workers, teachers, and many other professionals to report “known or suspected” child abuse or neglect. Here’s the critical distinction every mother needs to understand:
Therapists and doctors are mandatory reporters for abuse, not for illness.
Admitting you’re struggling with intrusive thoughts, depression, anxiety, or emotional overwhelm is not abuse. Having scary thoughts about your baby is not the same as harming your baby. Thoughts do not equal actions. Abuse requires that a child is actually harmed or in imminent danger.
Seeking help for mental health struggles is actually evidence of what professionals call “protective capacity”—it demonstrates you’re taking steps to keep yourself and your baby safe.
When DHR Involvement May Occur
DHR involvement typically happens in specific circumstances:
- Substance use affecting the infant: If an infant tests positive for controlled substances or shows withdrawal symptoms, a “Plan of Safe Care” assessment is triggered
- Documented neglect: Defined as “failure to provide adequate food, medical treatment, clothing, or shelter”—actual observable failures in care, not symptoms of depression
- Present danger: A parent who is “violent, out of control, or seemingly unable to control their behavior”—this refers to acute crises, not chronic mental health conditions
The Important Distinction
Having postpartum depression does not make you an unfit parent. Being diagnosed with a mental illness is not grounds for removing a child. The legal standard for involuntary commitment in Alabama requires “clear and convincing evidence” of a “real and present threat of substantial harm”—this is a very high legal bar.
Part Five: Your Rights—A Patient Bill of Rights for Alabama Mothers
Print this. Save this. Know this. These are your rights under current Alabama law.
1. The Right to Refuse Screening
You have the absolute right to decline any mental health screening, including the Edinburgh Postnatal Depression Scale (EPDS) questionnaire. You can say: “I am not comfortable completing this form today” or “I would prefer to discuss this verbally with my provider.”
There is no law in Alabama mandating that you complete postpartum depression screening. Providers may offer it, recommend it, and document your refusal—but they cannot require it.
2. The Right to Refuse Medication
You have the absolute right to decline any medication offered for postpartum depression or anxiety. You can ask about non-medication options such as therapy, support groups, lifestyle interventions, or watchful waiting.
A doctor’s recommendation is exactly that—a recommendation. Informed consent means you make the final decision about what goes into your body.
3. The Right to “Least Restrictive” Treatment
Alabama law (Code § 22-52-10.1) explicitly favors outpatient treatment over hospitalization. Unless you present an immediate danger to yourself or your baby—not theoretical risk, but actual immediate danger—a provider cannot force you into inpatient care.
The law recognizes a hierarchy: outpatient therapy, intensive outpatient programs, partial hospitalization, and only then inpatient treatment when absolutely necessary.
4. The Right to Your Medical Records
Under HIPAA and Alabama law, you have the right to request and receive copies of your medical records, including what your doctor has written about your mental health. You can review what’s being documented about you and request corrections to inaccurate information.
5. The Right to a Second Opinion
If an OB-GYN suggests medication you’re uncomfortable with, or if you receive a diagnosis you question, you have the right to seek consultation with a psychiatrist, psychologist, or Licensed Clinical Social Worker (LICSW) before making any decisions.
No treatment decision needs to be made in a single appointment. You can take time to research, consult, and decide.
6. The Right to Informed Consent
Before any treatment begins, you have the right to understand:
- What the treatment is and how it works
- What the potential benefits are
- What the potential risks and side effects are
- What alternatives exist
- What happens if you choose not to pursue treatment
7. The Right to Confidentiality
Your mental health information is protected by both HIPAA and Alabama law. With limited exceptions (mandatory reporting of actual abuse, court orders, immediate safety threats), your therapist or doctor cannot share your information without your written consent.
Your employer, your family, and your social network do not have automatic access to your mental health records.
8. The Right to Continuity of Care
With the 12-month Medicaid extension, you have the right to maintain your healthcare coverage throughout the postpartum period. You cannot be dropped from Medicaid at 60 days postpartum as under the old law.
9. The Right to Legal Representation
If you ever face DHR investigation or involuntary commitment proceedings, you have the right to legal representation. The Alabama Disabilities Advocacy Program (ADAP) provides federally mandated protection and advocacy for individuals with mental illness and can intervene if you’re being discriminated against based on a diagnosis rather than actual parenting behavior.
10. The Right to Be Treated with Dignity
Mental illness is a medical condition, not a moral failing. You have the right to be treated with respect by healthcare providers, to have your concerns taken seriously, and to participate as a full partner in decisions about your care.
Part Six: Looking Forward—Best Case, Worst Case, and Most Likely Scenarios
Based on legislative trends, comparison with other states, and the current political climate, here’s what the next five years might look like for maternal mental health rights in Alabama.
What Is Unlikely to Change
The legal standard for involuntary commitment. Alabama’s requirement of “clear and convincing evidence” of a “real and present threat of substantial harm” is constitutionally grounded and deeply embedded in state law. You cannot be committed simply for having depression or anxiety. This high legal bar is unlikely to be lowered.
Basic informed consent rights. The fundamental right to accept or refuse medical treatment is protected by constitutional principles that transcend state politics.
Mandatory reporter distinctions. The legal difference between mental illness and child abuse/neglect is established in statute and case law.
Best Case Scenario (5 Years)
- PPD screening becomes routine (like blood pressure checks) but remains voluntary
- Step therapy restrictions on Zuranolone and other PPD medications are lifted, either through state legislation or federal Safe Step Act passage
- “Integrated Care” models emerge where OB-GYN offices have therapists in-house, reducing stigma and improving access
- Midwifery expansion (HB257) passes, expanding provider networks in rural areas
- DHR protocols are updated to explicitly distinguish mental illness from neglect
- Peer support programs like Project SAFE expand statewide
Worst Case Scenario (5 Years)
- “Fetal personhood” interpretations expand to scrutinize pregnant and postpartum conduct more strictly
- Chemical endangerment laws, already aggressively applied in Alabama, create further chilling effects on help-seeking
- Refusing mental health care could theoretically be framed as “neglect” in contentious custody battles (though unlikely to be criminalized)
- Economic pressures on Medicaid lead to further restrictions on mental health coverage
Most Likely Scenario
The most probable outcome is incremental change in both directions. Supportive measures like midwifery expansion may pass while punitive reproductive legislation consumes legislative bandwidth. The fundamental framework of rights will likely remain stable, but access to care will continue to depend heavily on geography, insurance status, and individual provider practices.
The 2026 legislative session appears focused on contentious reproductive ethics debates (HB46’s extreme provisions regarding rape/incest cases) rather than consensus maternal mental health measures. This suggests that practical improvements in PPD care will more likely come through administrative policy changes, federal action, or grassroots clinical practice shifts than state legislation.
Part Seven: Resources for Alabama Mothers
Birmingham Metro Area
UAB Women & Infants Center
Tertiary care with Perinatal Nurse Navigators who connect patients to mental health services. Offers the “Mothers & Babies Support and Education Group”—a four-week cognitive-behavioral program.
Ascension St. Vincent’s Birmingham
Maternity Support Center with virtual and in-person Postpartum Support Groups. Baby Café locations (breastfeeding support that functions as peer support) meet Tuesdays and Wednesdays, 1-3 PM.
Brookwood Baptist Health
“Rattled” group for emotional regulation and anxiety meets Tuesdays 12:30-2:00 PM. “Beautiful Bundles” general new mom support meets Thursdays 12:30-2:30 PM.
Chocolate Milk Mommies
Specific support for Black breastfeeding mothers, meeting the second Saturday of each month at East Lake United Methodist Church.
Huntsville/North Alabama
Alabama Birth Center
Hosts “The Fourth Trimester Support Circle” for new mothers.
Shoals Area (Florence/Muscle Shoals)
Project Luna
Provides 16 free therapy sessions to eligible women—addresses the coverage gap for those who don’t qualify for Medicaid but can’t afford private care.
Statewide Resources
Postpartum Support International (PSI) Alabama
Warmline: 1-800-944-4773 (1-800-944-4PPD)
Provider directory and online support groups available at postpartum.net
Alabama Disabilities Advocacy Program (ADAP)
Legal advocacy for parents facing discrimination due to mental illness.
adap.ua.edu
Project SAFE (Alabama Perinatal Quality Collaborative)
Provides postpartum medical alert bracelets that identify you as recently postpartum to emergency responders.
Part Eight: What To Do If You’re Struggling
If you’re reading this article because you’re worried about your own mental health, here’s what we want you to know:
Seeking help is a sign of strength, not weakness. It’s evidence that you’re doing everything you can to be the best mother you can be.
You are not your thoughts. Intrusive thoughts—even scary ones about your baby—are extremely common in postpartum mental health conditions. Having these thoughts does not make you dangerous or unfit.
Treatment works. Postpartum depression and anxiety are highly treatable conditions. With proper support, the vast majority of mothers recover fully.
You have options. Medication is one tool, but it’s not the only tool. Therapy, support groups, lifestyle changes, and time all play roles in recovery. You get to choose what feels right for you.
You have rights. You cannot be forced into treatment against your will simply for having depression or anxiety. You are in control of your care.
A Checklist for Expecting Mothers: 7 Things You Can Do Right Now to Protect Yourself
1. Know Your Magic Words for Refusing a Screening
If you don’t want to complete the Edinburgh Postnatal Depression Scale (EPDS) questionnaire at your OB appointment, say this:
“I’m not comfortable completing this form today. I’d prefer to discuss how I’m feeling verbally if you have concerns.”
This works because there is no Alabama law requiring you to complete written PPD screening. SB191, the bill that would have mandated Medicaid coverage for screenings, died in committee on May 6, 2025. Screening remains entirely voluntary.
2. Request “Outpatient Only” in Writing
If you’re seeking mental health treatment and worried about hospitalization, tell your provider at your first appointment:
“I want to document that I’m seeking outpatient care only. Please note in my chart that I’m here voluntarily and prefer the least restrictive treatment options.”
Alabama Code § 22-52-10.1 legally requires providers to favor outpatient treatment over hospitalization. Having this preference documented creates a paper trail that protects you.
3. Bring a Support Person to Appointments
You have the right to have someone present during medical appointments. A partner, mother, friend, or doula can:
- Take notes on what’s recommended
- Ask clarifying questions you might forget
- Witness what was actually said (versus what gets documented)
- Help you feel less pressured to agree to something you’re unsure about
Simply say: “I’ve brought [name] for support. They’ll be staying for this appointment.”
4. Ask This Question Before Signing Anything
Before signing intake forms at any new provider, ask:
“Can you explain exactly what triggers a mandatory report in your practice? I want to understand the limits of confidentiality before we begin.”
A good provider will explain clearly: mandatory reporting is for child abuse or neglect—actual harm or imminent danger. Depression, anxiety, and intrusive thoughts are not reportable conditions. If a provider can’t clearly explain this distinction, consider finding another provider.
5. Get Your Medicaid Extended—Here’s How
Alabama now offers 12-month postpartum Medicaid coverage (up from 60 days). If your coverage is about to end or already ended, take these steps:
- Call Alabama Medicaid: 1-800-362-1504
- Say: “I gave birth within the last 12 months and need to confirm my postpartum coverage extension”
- Have ready: Your Medicaid ID, date of delivery, and baby’s birth certificate
- If denied: Request a written denial and file an appeal—the 12-month extension is state policy as of October 2022
6. Document Everything in a “Mama File”
Create a folder (physical or digital) containing:
- Copies of all your medical records (request these under HIPAA—providers must comply within 30 days)
- Names, dates, and summaries of every appointment
- Any medications recommended and your response
- Copies of anything you sign
- Contact information for a family law attorney (even if you never need one)
This isn’t paranoia—it’s preparation. Documentation protects you if anything is ever misrepresented.
7. Save These Emergency Numbers Now
Put these in your phone today:
- Postpartum Support International Warmline: 1-800-944-4773 (call or text)
- Alabama Medicaid: 1-800-362-1504
- ADAP (Alabama Disabilities Advocacy Program): 1-800-826-1675—free legal help if DHR contacts you
- National Maternal Mental Health Hotline: 1-833-943-5746 (24/7, free, confidential)
What Your OB Isn’t Telling You About PPD Medication in Alabama
Here’s what we see in clinical practice that most mothers don’t know:
Zuranolone (Zurzuvae) Is Nearly Impossible to Get on Medicaid
You may have heard about the new “miracle” 14-day PPD medication. Here’s the reality in Alabama:
- Alabama Medicaid requires you to fail TWO different antidepressants before they’ll cover Zuranolone
- Each antidepressant trial takes 4-6 weeks to “fail”
- That’s 8-12 weeks of waiting and suffering before accessing the faster-acting medication
- Your doctor must complete Form 369 (Prior Authorization) documenting both failures
- Even then, approval isn’t guaranteed
If a provider suggests Zuranolone, ask directly: “What’s the prior authorization process, and how long will it realistically take to get approved?”
You Can Ask for Therapy First
Medication is not the only option. If your provider jumps straight to prescribing, you can say:
“I’d like to try therapy first before considering medication. Can you refer me to a perinatal mental health specialist?”
Your Medicaid coverage (extended to 12 months postpartum) includes therapy. You’re entitled to try non-medication approaches.
Generic SSRIs Have Different Side Effect Profiles
If you do choose medication, know that not all antidepressants affect breastfeeding, libido, sleep, or weight the same way. Ask your prescriber:
- “Which option is most compatible with breastfeeding?”
- “Which has the lowest risk of weight gain?”
- “Which is least likely to affect my sleep?”
You have the right to participate in choosing which medication, not just whether to take one.
DHR and Postpartum Depression: Separating Fact from Fear
This is the question that brings most mothers to articles like this one. Let’s be direct.
Can DHR Take Your Baby Because You Have Postpartum Depression?
No. Having a mental health diagnosis is not grounds for child removal in Alabama. Here’s what the law actually says:
DHR can only intervene when there is evidence of:
- Abuse: Physical harm, sexual abuse, or emotional cruelty to the child
- Neglect: Failure to provide adequate food, shelter, clothing, or medical care
- Present danger: The child is in immediate risk of harm
Depression is not neglect. Anxiety is not abuse. Intrusive thoughts are not harm.
What Actually Triggers DHR Involvement
Based on DHR protocols, here’s what can trigger an investigation:
- Infant testing positive for controlled substances at birth
- Observable signs the child is not being fed, clothed, or supervised
- Reports of physical injury to the child
- Parent appearing actively impaired (intoxicated, psychotic, violent) while caring for child
Notice what’s not on that list: being sad, being anxious, having scary thoughts, taking psychiatric medication, going to therapy, or being diagnosed with PPD.
What To Do If DHR Contacts You
If a DHR caseworker shows up or calls:
- Stay calm. An investigation doesn’t mean removal.
- Ask for their card and case number. Write everything down.
- You can say: “I’d like to consult with an attorney before answering questions. When can we reschedule?”
- Call ADAP immediately: 1-800-826-1675. They provide free legal advocacy for parents with disabilities/mental illness.
- Document the contact: Date, time, what was said, who was present.
If you’re already in therapy, your therapist can provide documentation that you’re actively seeking help—this is evidence of “protective capacity” that works in your favor.
Your Complete Rights Checklist
Print this or screenshot it. These are your rights under current Alabama law:
☐ Refuse any screening (EPDS, PHQ-9, etc.) without penalty
☐ Refuse any medication and request non-medication alternatives
☐ Access your complete medical records within 30 days of request
☐ Receive 12 months of postpartum Medicaid coverage
☐ Bring a support person to any appointment
☐ Request outpatient treatment only
☐ Seek a second opinion before any major treatment decision
☐ Know the limits of confidentiality before treatment begins
☐ Receive the least restrictive treatment appropriate for your condition
☐ Access legal advocacy through ADAP if your rights are violated
Red Flags: When to Seek Different Care
Based on our clinical experience, here are warning signs that a provider may not be the right fit:
- They insist you must take medication without discussing alternatives
- They can’t clearly explain mandatory reporting limits
- They seem rushed or dismiss your concerns as “just hormones”
- They threaten hospitalization or DHR involvement to pressure compliance
- They won’t let you bring a support person
- They don’t ask about your birth experience or trauma history
You deserve a provider who treats you as a partner in your care, not a patient to be managed.
What’s Actually Changing in Alabama Law (2025-2026)
Here’s the legislative reality, stripped of social media panic:
Bills That Died (Not Becoming Law)
SB191 – Would have mandated Medicaid coverage for PPD screening and banned step therapy for PPD medications. Indefinitely postponed May 2025. The supportive infrastructure this bill offered did not pass.
Bills Still Active
HB257 (Midwifery Expansion) – Supported by ACLU of Alabama, this would expand midwife scope of practice and could improve rural maternal mental health access. Still moving through legislature.
What’s Not Changing
- Involuntary commitment standards (still requires “clear and convincing evidence” of imminent danger)
- Informed consent rights
- Mandatory reporter distinctions between illness and abuse
- Your right to refuse treatment
Local Birmingham Resources—Vetted and Current
These are resources we actually refer clients to:
Free/Low-Cost Support Groups
Brookwood Baptist “Rattled” Group
Tuesdays, 12:30-2:00 PM | Focus: Anxiety and emotional regulation
Location: Women’s Center, Birmingham
St. Vincent’s Baby Café
Tuesdays & Wednesdays, 1:00-3:00 PM | Breastfeeding support + peer connection
Location: Women’s & Children’s Center
UAB Mothers & Babies Program
4-week series | Evidence-based PPD prevention
Contact: UAB Women & Infants Center
Chocolate Milk Mommies
2nd Saturday monthly, 11:00 AM | Black maternal support
Location: East Lake United Methodist Church
Crisis Resources
PSI Warmline: 1-800-944-4773 (call or text “HELP”)
National Maternal Mental Health Hotline: 1-833-943-5746 (24/7)
Crisis Text Line: Text HOME to 741741
If You Need Legal Help
ADAP: 1-800-826-1675 (free advocacy for parents with mental illness)
Legal Aid Society of Birmingham: 205-328-3540
Getting Expert Support in Birmingham
Navigating maternal mental health challenges requires specialized support from providers who understand both the clinical complexities and the unique pressures facing Alabama mothers.
Dr. Haley Beech at Taproot Therapy Collective is a perinatal mental health and motherhood specialist who can help you navigate postpartum depression, anxiety, birth trauma, identity transitions into motherhood, and the complex emotions that accompany this profound life change. Her approach honors both the challenges and the transformative potential of the motherhood journey.
Whether you’re struggling with symptoms, worried about your rights, or simply need someone who understands what you’re going through, specialized perinatal support can make all the difference.
Schedule a consultation with Dr. Haley Beech at Taproot Therapy Collective →
This article was researched and written by Taproot Therapy Collective to provide accurate, comprehensive information about maternal mental health rights in Alabama. It is intended for educational purposes and does not constitute legal or medical advice. For specific concerns about your situation, please consult with a qualified attorney or healthcare provider.
Last updated: January 2026























0 Comments