The Body is the Mind: Demystifying the Body-Brain Connection in Trauma Therapy

For centuries, Western medicine and psychology operated under a delusion inherited from the philosopher René Descartes: the idea that the mind and the body are separate entities. “I think, therefore I am,” he famously declared, locating the seat of human existence entirely within the cognitive intellect. This Cartesian Dualism treated the body as a mere machine—a taxi cab for the brain—while the mind was viewed as the driver, fully in control and independent of the vehicle.
However, the last thirty years of neuroscience have shattered this assumption. We now know that the body and brain are not separate; they are a continuous, bi-directional feedback loop. In fact, for survivors of trauma, the “driver” (the thinking brain) is often held hostage by the “vehicle” (the nervous system). As Dr. Bessel van der Kolk famously posited, “The Body Keeps the Score.” To heal mental health conditions like PTSD, anxiety, and depression, we cannot simply talk to the mind; we must learn to speak the language of the body.
The Anatomy of the Split: “Top-Down” vs. “Bottom-Up” Processing
To understand why we feel the way we do, we must understand the architecture of the human brain. It is not a single organ but a hierarchy of three evolutionary structures, often referred to as the Triune Brain.
[Image of triune brain model diagram]
1. The Neocortex (The Thinking Brain)
This is the newest part of the brain, responsible for logic, language, time, and narrative. It is where “talk therapy” operates. It processes information Top-Down: “I see a spider. I know spiders in this area aren’t poisonous. Therefore, I am safe.”
2. The Limbic System (The Emotional Brain)
Located beneath the cortex, this area houses the Amygdala (the smoke detector) and the Hippocampus (the memory filer). It judges the world based on emotional valence: good/bad, safe/dangerous. It does not understand time; a trigger from 20 years ago feels like it is happening now.
3. The Brainstem (The Reptilian Brain)
The oldest and deepest structure, responsible for survival functions like heart rate, breathing, and the Freeze/Fight/Flight response. It processes information Bottom-Up: “Sensation of fast movement -> Adrenaline dump -> Run.” This happens milliseconds before the thinking brain even knows what is happening.
The Trauma Trap: When trauma occurs, the connection between the Neocortex and the Limbic system is severed. The “thinking brain” goes offline (a phenomenon called hypofrontality), and the body is left reacting to a past threat as if it were a present reality. You cannot reason with a brainstem. This is why you can know you are safe (cognitive) but still feel terrified (somatic).
The Polyvagal Ladder: How the Nervous System Scans for Safety
The bridge between the brain and the body is the Vagus Nerve. According to Stephen Porges’ Polyvagal Theory, our nervous system is constantly scanning the environment for danger signals—a process called Neuroception.
We move through three distinct physiological states, like climbing a ladder:
- Ventral Vagal (Safe & Social): We are calm, connected, and capable of empathy. Digestion works, and the immune system heals. This is the state necessary for therapy to work.
- Sympathetic (Mobilization): The “Fight or Flight” response. Heart rate increases, muscles tense, and the body prepares for action. Anxiety is essentially a stuck Sympathetic state.
- Dorsal Vagal (Immobilization): The “Freeze or Collapse” response. If fighting or fleeing is impossible, the body shuts down to feign death. This manifests as dissociation, depression, and numbness.
Traditional talk therapy requires the client to be in a Ventral Vagal state to process language. However, many trauma survivors are stuck in chronic Sympathetic or Dorsal states. Asking them to “talk about it” can be re-traumatizing because their physiology is screaming that they are currently under attack.
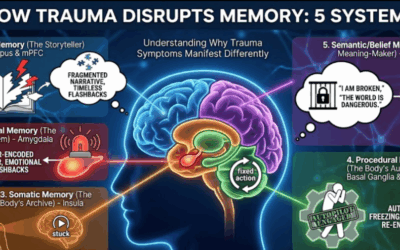
Implicit vs. Explicit Memory: Why the Body Remembers What the Mind Forgets
Why do we get triggered by a smell, a sound, or a tone of voice without knowing why? This is the difference between Explicit Memory and Implicit Memory.
- Explicit Memory (Declarative): This is the movie of your life. “I remember when I graduated high school.” It has a beginning, middle, and end. It is stored in the Hippocampus and accessible to the Neocortex.
- Implicit Memory (Non-Declarative): This is the memory of sensation and procedure. It is the feeling of the steering wheel in your hands, or the knot in your stomach when your father yelled.
Traumatic memories are often encoded primarily as Implicit Memories. Because the hippocampus (the timestamping mechanism) goes offline during extreme stress, the memory is not filed away as “past.” Instead, it remains trapped in the body-brain as a free-floating sensation. A somatic therapist helps the client locate these physical footprints—the tightness in the throat, the heaviness in the chest—and helps the brain finally file them away.
Going Beyond Cognitive Understanding: The Rise of Brain-Based Therapies
Since we cannot think our way out of a body-based problem, we need therapies that target the subcortical brain directly. These are often called “Bottom-Up” therapies.
1. Brainspotting: Where You Look Affects How You Feel
Discovered by David Grand, Brainspotting posits that our visual field is mapped to our subcortical brain. By locating a specific eye position (a “Brainspot”) that correlates with a somatic sensation, the therapist can hold the “door open” to the deep brain. This allows the brain to process the frozen traumatic packet without the need for extensive talking.
2. EMDR (Eye Movement Desensitization and Reprocessing)
EMDR utilizes bilateral stimulation (moving eyes back and forth, tapping, or audio tones) to mimic the REM sleep cycle. This stimulation keeps the dual awareness of “I am here now” while visiting the “there and then,” allowing the brain to digest the traumatic memory and move it from the Amygdala to the long-term memory banks.
3. Somatic Experiencing
Developed by Peter Levine, this modality observes that wild animals rarely get PTSD because they physically shake off the energy of a threat after it passes. Humans, constrained by social norms, often “freeze” this energy. Somatic Experiencing involves pendulation—moving between a resource (a safe feeling) and the activation (the trauma)—to slowly discharge the stuck energy.
My Experience with Brainspotting: A Case Study in Somatic Release
During my personal journey with Brainspotting, I discovered a profound emotional experience that had always been present but remained unrecognized by my cognitive mind. In talk therapy, I could articulate why I was anxious perfectly. I knew the childhood roots; I knew the logic. Yet, the panic attacks persisted.
In the Brainspotting session, we didn’t analyze the narrative. We simply located the tightness in my solar plexus and found the eye position that intensified it. As I held my gaze there, a flood of implicit memory—images, sensations, and emotions—surged forward. It was not an intellectual “aha” moment; it was a physiological release. My body shook, I felt temperature changes, and then, a sudden calm. The “alarm” in my brainstem had finally been turned off. I gained the ability to acknowledge the emotion’s presence and consciously choose my subsequent actions, rather than being hijacked by a reflex.
The Body-Brain Connection: Emotional and Physical Footprints
The body brain stores information not as visual images or intellectual comprehension but as emotional and physical footprints. When we encounter triggers, our body remembers, often manifesting as:
- Muscular Armoring: Chronic tension in the jaw, shoulders, or hips (the psoas muscle is known as the “muscle of the soul” for how it holds trauma).
- Visceral Distress: IBS, nausea, or that “cold pit” in the stomach.
- Respiratory Changes: Shallow, chest-based breathing that signals constant anxiety to the vagus nerve.
These physical reactions are accompanied by an energetic defensive posture, as our sensory-motor system mobilizes to protect us. By acknowledging and sitting with these experiences—a practice known as Interoception—we can begin to understand the profound impact of the body brain on our daily lives.
The body-brain connection highlights the vital role our bodies play in shaping our experiences and responses. Brain-based therapies provide a pathway to access and process deeply rooted traumas that cognitive approaches often overlook. As we navigate the complexities of our emotional lives, it is essential to recognize the power of the body brain and its influence on our overall well-being. By engaging with this concept and exploring brain-based therapies, we can find healing, resilience, and a newfound sense of control over our emotions.
Bibliography
- Levine, P. A. (2010). In an Unspoken Voice: How the Body Releases Trauma and Restores Goodness. North Atlantic Books.
- Porges, S. W. (2011). The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-regulation. W. W. Norton & Company.
- van der Kolk, B. A. (2015). The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma. Penguin Books.
- Damasio, A. (2000). The Feeling of What Happens: Body and Emotion in the Making of Consciousness. Mariner Books.
- Grand, D. (2013). Brainspotting: The Revolutionary New Therapy for Rapid and Effective Change. Sounds True.


















0 Comments