The clinical landscape of Post-Traumatic Stress Disorder treatment is undergoing its most significant transformation since the introduction of prolonged exposure therapies. For decades our dominant therapeutic paradigm operated on a top-down model which assumed that cortical insight and verbal processing were the primary vehicles for extinguishing traumatic fear. We operated under the belief that by altering the narrative or the cognitive appraisal of a traumatic event the downstream physiological dysregulation would resolve. However data emerging in 2024 and 2025 suggests a fundamental inversion of this hierarchy. The field is rapidly pivoting toward bottom-up interventions that bypass the prefrontal cortex to directly target the subcortical autonomic and visceral substrates of threat. This article analyzes this new frontier for the practicing clinician and examines treatments that address PTSD not merely as a psychological disorder of memory but as a physiological disorder of the autonomic nervous system and midbrain survival circuitry.
The Sympathetic Reset: Stellate Ganglion Block
Among the emerging modalities the Stellate Ganglion Block (SGB) represents the most advanced integration of anesthesiology and psychiatry. While originally utilized for complex regional pain syndrome SGB involves the precise injection of a local anesthetic into the stellate ganglion which is a cluster of sympathetic nerves located at the level of the C6 and C7 vertebrae. In the context of trauma this procedure is conceptualized not as a numbing agent for pain but as a biological reboot for a sympathetic nervous system locked in a chronic fight-or-flight state. The durability of the effects of SGB has challenged simple pharmacological explanations because the relief often lasts months despite the anesthetic metabolizing within hours. Current research points to the Nerve Growth Factor (NGF) Hypothesis to explain this phenomenon. Chronic stress and PTSD are associated with elevated levels of NGF which promotes the sprouting of sympathetic nerve fibers and increases the concentration of norepinephrine. This process effectively sensitizes the system to threat. The injection of anesthetic into the ganglion is hypothesized to trigger a downregulation of NGF and a reduction in norepinephrine levels which breaks the positive feedback loop between the peripheral sympathetic nervous system and the central threat circuitry involving the amygdala and hippocampus.
Targeting the Midbrain: Deep Brain Reorienting
While SGB targets the peripheral autonomic system a new class of psychotherapies is targeting the central nervous system threat detection circuitry found in the midbrain and brainstem. Deep Brain Reorienting (DBR) represents a significant theoretical advancement by moving beyond the limbic system to target phylogenetically older structures like the Superior Colliculus and the Periaqueductal Gray. DBR is predicated on the hypothesis that the physiological response to threat occurs in a specific and rapid sequence. This sequence begins with Orienting which is mediated by the Superior Colliculus directing the eyes and head toward a new stimulus. This is followed by Tension mediated by the Locus Coeruleus which generates the preparatory tension for action. The next phase is Shock which is mediated by the Periaqueductal Gray and represents the moment the system registers a threat that cannot be immediately mitigated. Finally the sequence concludes with Affect which is the generation of emotional states in the limbic system. Standard trauma therapies typically intervene at the level of Affect or Cognition. DBR posits that if the trauma is locked at the level of Orienting or Shock then processing the emotion is insufficient. The therapy aims to access the physical sensation in the neck and shoulders associated with that split-second turning toward danger to release the residual shock.
A landmark Randomized Controlled Trial conducted in 2023 and 2024 provided robust evidence for the efficacy of DBR. The study demonstrated that eight sessions resulted in a 36.6% reduction in CAPS-5 scores post-treatment which deepened to a 48.6% reduction at the 3-month follow-up. Most notably 52% of participants in the DBR group no longer met the diagnostic criteria for PTSD at follow-up compared to the waitlist group where no significant change occurred. The study also highlighted a remarkably low dropout rate which suggests that DBR is well-tolerated even by patients with complex PTSD who often destabilize during exposure-based treatments.
The Oculomotor Debate: Brainspotting and the Flash Technique
Brainspotting operates on the theory that the visual field maps to the neural substrate of the brain. A brainspot is defined as a specific eye position that correlates with the activation of a traumatic or somatic pocket of distress. Proponents hypothesize that the fixed gaze engages the Superior Colliculus in a way that bypasses cortical inhibition and allows for the processing of implicit and non-verbal memory. While some neuroscientists argue that the claim that specific eye positions correspond to discrete memory capsules lacks direct fMRI validation clinical trials have begun to substantiate its utility. A 2024 RCT comparing Brainspotting to treatment-as-usual found significant improvements in PTSD and depression. Another comparative study showed that while EMDR produced slightly larger effect sizes Brainspotting also demonstrated robust efficacy and is often highlighted as a flexible alternative for patients who find rigid protocols overstimulating.
The Flash Technique has emerged as another distinct and minimally intrusive intervention. Originally developed as a titration tool for EMDR it is now a standalone therapy utilizing a mechanism of subliminal processing. The patient engages in a positive engaging focus such as discussing a hobby while momentarily checking or flashing on the traumatic memory. The hypothesis is that by keeping the amygdala calm via the positive focus the fleeting contact with the trauma allows the memory to be reconsolidated and stripped of its emotional valence without triggering the defense cascade. Recent Bayesian analyses have found no significant difference in the reduction of memory vividness between Flash and EMDR but noted that Flash was rated as significantly more pleasant by participants.
Rewiring the Vagus Nerve: Technology Meets Biology
The Vagus Nerve has become a primary target for technological interventions aimed at increasing vagal tone to counteract sympathetic dominance. At the forefront of this neurotechnology is Targeted Plasticity Therapy which involves the surgical implantation of a Vagus Nerve Stimulation (VNS) device. Unlike continuous stimulation used for epilepsy this protocol triggers short bursts of stimulation precisely when the patient engages with a traumatic memory during prolonged exposure therapy. This timing triggers the release of neuromodulators like acetylcholine and norepinephrine which enhances synaptic plasticity and accelerates fear extinction. The results of a Phase 1 trial published in 2025 were unprecedented as 100% of the participants lost their PTSD diagnosis following the treatment course. For broader scalability research is also focused on non-invasive wearable technologies like Apollo Neuro and Sensate. Apollo Neuro is worn on the wrist or ankle and delivers silent vibrations designed to mimic the frequency and rhythm of human touch. Clinical trials have reported that participants described the experience as life-changing with improved sleep and a greater ability to return from dissociative states. Sensate utilizes infrasonic resonance via bone conduction on the sternum to stimulate the vagus nerve. Pilot studies indicate a significant decrease in stress levels and improvements in sleep quality. While these non-invasive tools may not yet offer the durable cures seen in implanted VNS trials they provide accessible means for daily autonomic regulation.
The Internal Environment: Psychobiotics and Inflammation
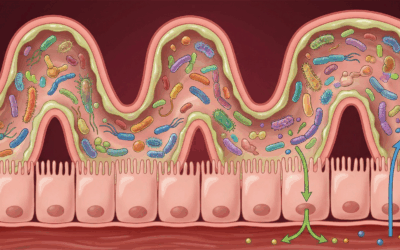
PTSD is increasingly understood as a systemic inflammatory disorder often accompanied by dysbiosis in the gut microbiome. Patients frequently exhibit elevated levels of pro-inflammatory cytokines which disrupts the blood-brain barrier and perpetuates neuroinflammation. The Psychobiotic Revolution addresses this by using specific probiotic strains to signal safety to the brain via the vagus nerve. The strain Lactobacillus rhamnosus GG (LGG) has emerged as a lead candidate. A longitudinal double-blind randomized placebo-controlled trial involving veterans is currently assessing the impact of LGG supplementation on biological signatures of inflammation and clinical symptoms. Preliminary studies suggest that probiotic treatment can reverse stress-induced decreases in cortical Brain-Derived Neurotrophic Factor and reduce anxiety behaviors. This suggests that nutritional psychiatry will become a standard adjunctive pillar in comprehensive trauma care.
Future Frontiers: Methylone and 3MDR
The pharmacological landscape is also shifting. Following regulatory delays with MDMA Methylone (TSND-201) received FDA Breakthrough Therapy Designation in 2025. Methylone acts as a rapid-acting neuroplastogen that lacks the hallucinogenic profile of classic psychedelics. This makes it potentially safer and more scalable within existing medical infrastructures. Finally Modular Motion-assisted Memory Desensitization and Reconsolidation (3MDR) offers a multimodal therapy for treatment-resistant PTSD. This intervention combines Virtual Reality exposure with physical movement on a treadmill. The element of forward motion is hypothesized to physiologically counteract the freeze response and encourage approach behavior toward the trauma.
The convergence of anesthesiology neurotechnology gastroenterology and psychotherapy is creating a robust toolkit that respects the complexity of survival. We are moving away from a one-size-fits-all approach limited to cognitive processing and SSRIs. We can now envision a stratified treatment model where we utilize SGB for sympathetic hyperarousal DBR for brainstem shock psychobiotics for systemic inflammation and targeted neuroplasticity for hardened fear networks. By addressing the biological reality of trauma including the frozen gaze and the inflamed gut clinicians are finally gaining the means to treat the disorder at its source.



















0 Comments