From exposure therapy’s limitations to the somatic revolution, from EMDR’s established efficacy to Brainspotting’s emerging promise, and why the future of trauma treatment lies in matching the therapy to the brain.
The field of trauma treatment is undergoing a transformation that challenges three decades of clinical assumptions. For years, the consensus was clear: trauma is a disorder of fear, and the cure is exposure. Confront the memory, extinguish the fear response, move on. This framework produced Prolonged Exposure and Cognitive Processing Therapy, the “gold standard” protocols recommended by every major guideline body from the American Psychological Association to the VA/DoD.
These approaches work. The evidence is robust. But they don’t work for everyone, and the reasons why are reshaping how we understand trauma itself.
The research emerging in 2024 and 2025 tells a more complex story. It reveals that 30 to 50 percent of patients don’t achieve remission even after completing gold-standard protocols. It shows dropout rates in real-world settings reaching 50 percent for exposure therapy. It documents how the brain’s fear circuitry can shut down the very cognitive capacities these treatments require. And it validates what somatic therapists have long argued: that trauma lives in the body, not just the mind, and that effective treatment must address the autonomic nervous system directly.
This is not a story of one approach replacing another. It is a story of the field growing up, recognizing that trauma is biologically heterogeneous and that matching treatment to patient is more important than declaring any single therapy the universal answer.
The Established Canon: What Works and What Doesn’t
Prolonged Exposure (PE) remains the most extensively studied trauma treatment. It operates on Emotional Processing Theory: trauma creates a pathological fear structure in memory, and the cure is to activate that structure while acquiring corrective information that contradicts the expectation of harm. Through imaginal exposure (recounting the trauma in present tense) and in vivo exposure (confronting avoided situations), patients habituate to their fear and the memory loses its power.
The efficacy data is solid. Meta-analyses of exposure-based therapies confirm large effect sizes relative to waitlist and treatment-as-usual controls. For patients who can tolerate the protocol, PE effectively extinguishes the physiological startle response and intrusive symptoms associated with the amygdala’s fear circuitry. Furthermore, recent adaptations such as twice-weekly massed protocols have shown potential for reducing dropout rates by condensing the treatment duration, thereby minimizing the period of anticipatory anxiety that often leads to attrition.
Cognitive Processing Therapy (CPT) takes a different angle. Rather than prioritizing habituation to the memory itself, CPT focuses on “stuck points,” the maladaptive beliefs about safety, trust, power, control, esteem, and intimacy that develop following trauma. Through Socratic questioning and structured worksheets, patients learn to challenge overgeneralized beliefs like “The world is entirely dangerous” or “It was all my fault.” Head-to-head comparisons generally show CPT and PE are equivalent in efficacy for PTSD symptom reduction. CPT is often favored for presentations involving intense guilt, shame, or moral injury, as the cognitive restructuring component directly addresses the interpretive framework of the trauma rather than just physiological arousal.
Both treatments are recommended by the APA and the International Society for Traumatic Stress Studies as first-line interventions.
So what’s the problem?
The Efficacy-Effectiveness Gap
The central issue is the distinction between efficacy (performance in controlled trials) and effectiveness (performance in routine clinical care). The gap between them is substantial.
Attrition is high. While meta-analyses of clinical trials suggest dropout rates for PE hover around 20 to 30 percent, effectiveness studies in community and VA settings often report attrition as high as 50 percent. The requirement to revisit and relive traumatic events is inherently distressing. For subsets of patients, particularly those with high anxiety sensitivity or dissociative subtypes, the exposure process can precipitate flooding or emotional dysregulation that exceeds their coping capacity. This has led to vigorous debate regarding the “safety” of exposure for complex presentations, with some clinicians arguing that without prior stabilization, exposure can be retraumatizing.
Non-response is common. Even among treatment completers, a substantial minority don’t achieve remission. Estimates suggest 30 to 50 percent of patients retain a PTSD diagnosis or significant residual symptoms following a full course of PE or CPT. This non-response is particularly prevalent in cases of chronic, developmental, or complex trauma, where the pathology extends beyond a specific fear memory to encompass broader dysregulation of self-concept and affect. The APA’s guidelines acknowledge this limitation, noting that while TF-CBT is the best tool available, it is not a panacea, and “shared decision-making” is essential to align treatment selection with patient values and tolerance.
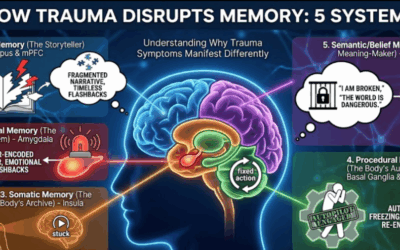
The brain goes offline. Neuroimaging research indicates that during traumatic recall, the medial prefrontal cortex is often hypoactive, and Broca’s area (responsible for speech) may shut down. Bessel van der Kolk termed this “speechless terror.” Under these conditions, the cognitive capacity required for CPT or PE is arguably unavailable. You cannot restructure cognitions when the cognitive apparatus has gone dark.
This is where the somatic revolution enters.
Written Exposure Therapy: A Bridge Protocol
In response to the barriers of time commitment and dropout associated with PE and CPT, Written Exposure Therapy (WET) has emerged as a critical innovation. Developed by Denise Sloan and Brian Marx, WET is a brief five-session protocol that removes the extensive homework and cognitive restructuring components of standard TF-CBT. Patients engage in written narrative exposure during the session, with the therapist providing brief feedback and checking for habituation.
The clinical utility of WET lies in its efficiency and tolerability. Multiple non-inferiority trials have demonstrated that WET produces symptom reductions comparable to PE but with significantly lower dropout rates, often less than 15 percent. By reducing the “dose” of exposure to a manageable level and removing the burden of homework, WET lowers the barrier to entry for hesitant patients. The VA/DoD Clinical Practice Guidelines now recommend WET as a viable alternative, particularly in resource-constrained health systems where the 12 to 16 session commitment of PE or CPT creates bottlenecks in access to care.
However, questions remain regarding its efficacy for severe Complex PTSD, as the brief nature of the intervention may be insufficient to address deep-seated disturbances in self-organization.
The Shift from Top-Down to Bottom-Up
The most significant evolution in the trauma field is the recognition that cognitive-linguistic interventions may be insufficient for a nervous system fundamentally dysregulated at the brainstem level. This has precipitated what researchers call the shift from “top-down” to “bottom-up” processing.
Top-down therapies (CBT, CPT) assume that changes in cognition will drive changes in emotion and physiology. They rely on the functional integrity of the prefrontal cortex to inhibit the amygdala. But if the prefrontal cortex is offline during traumatic activation, this top-down inhibition fails.
Bottom-up approaches posit that trauma is stored in the subcortical brain and the body (sensorimotor memory) and that effective treatment must begin with the regulation of the autonomic nervous system. These therapies, including Somatic Experiencing, Sensorimotor Psychotherapy, and Brainspotting, aim to alter the physiological state directly through interoceptive awareness and motor execution, theoretically calming the limbic system to a point where cognitive integration becomes possible.
This model aligns with the “Triune Brain” concept, targeting the brainstem and limbic system before engaging the neocortex. It connects to what we understand about the roots of trauma in the deep brain and how experiential and somatic therapy differs from cognitive approaches.
Somatic Experiencing: The Body Completes What the Mind Cannot
Somatic Experiencing (SE), developed by Dr. Peter Levine, is perhaps the most prominent bottom-up modality. It is grounded in the ethological observation that wild animals, despite frequent life-threatening threats, rarely exhibit trauma symptoms. Levine hypothesized that animals discharge the survival energy mobilized for fight or flight through physical mechanisms (shaking, trembling, running) once the threat has passed. Humans, constrained by the neocortex and social conditioning, often inhibit this discharge, leading to “trapped” survival energy in the nervous system.
SE defines trauma not by the event itself but by the nervous system’s inability to restore equilibrium. The therapy utilizes the SIBAM framework, tracking Sensation, Image, Behavior, Affect, and Meaning to guide the client toward “completion” of defensive responses. Three key mechanisms distinguish SE from exposure therapy:
Titration: The therapist introduces small, manageable amounts of activation to prevent the flooding common in exposure therapy. Rather than “running toward the fire,” clients “dip a toe in.”
Pendulation: Clients shift attention between areas of activation (distress) and areas of resource and safety (feeling the feet on the ground, noticing where the body feels okay). This oscillation builds the nervous system’s capacity to tolerate intensity.
Discharge: The goal is the release of tension, often manifested as heat, tingling, or spontaneous movement, which SE posits is the biological resolution of the trauma.
Historically, SE lacked the rigorous RCT evidence of CBT. That has changed. The landmark Brom et al. study provided robust evidence for SE’s efficacy, finding significant reductions in PTSD symptoms (Cohen’s d = 0.94 to 1.26) compared to waitlist control. Crucially, these improvements occurred without the detailed narrative exposure required by PE, suggesting that somatic regulation alone can drive symptom remission.
Recent research in safety-net settings has highlighted the high acceptability of somatic therapies among diverse, low-income populations who had previously disengaged from exposure-based treatments. The focus on bodily sensation rather than verbal narrative was cited as a key factor in reducing stigma and retraumatization.
One of the most compelling arguments for SE is its low attrition rate. Unlike PE, which asks patients to “run toward the fire,” SE asks them to “dip a toe in.” This gentle approach makes it particularly suitable for patients with complex trauma who have a low window of tolerance. The focus on resourcing, establishing safety before processing, aligns with the phased treatment model recommended for Complex PTSD.
EMDR: The Hybrid That Became First-Line
EMDR occupies a unique “hybrid” space in the trauma landscape. While it incorporates cognitive elements (identifying negative and positive cognitions), its defining feature is bilateral stimulation, typically eye movements but also taps or auditory tones.
The mechanism of bilateral stimulation remains the subject of intense scientific debate:
Working Memory Hypothesis: The most empirically supported theory suggests that performing a dual task (tracking eye movements) while holding a traumatic memory taxes the limited capacity of working memory. This competition degrades the vividness and emotional intensity of the memory, facilitating reconsolidation with less distress.
REM Sleep Hypothesis: Proponents argue that bilateral stimulation mimics the saccadic eye movements of REM sleep, activating innate physiological processing systems that consolidate episodic memories into semantic networks.
Parasympathetic Activation: Another view is that bilateral stimulation triggers a “relaxation response” via the parasympathetic nervous system, allowing the patient to remain in a window of tolerance while processing.
What matters clinically is that EMDR is firmly established as a Tier 1 treatment. It is recommended by the APA, ISTSS, and VA/DoD with the same level of endorsement as PE and CPT.
Meta-analyses consistently show that EMDR is equivalent to trauma-focused CBT in reducing PTSD symptoms. But EMDR possesses distinct advantages in implementation:
Efficiency: Some studies indicate EMDR may achieve remission in fewer sessions than TF-CBT.
Tolerability: Comparisons often find lower dropout rates in EMDR compared to PE. This is likely because EMDR does not require the patient to verbally describe the trauma in explicit detail or listen to recordings of the narrative, reducing the “dread” factor.
No homework: The absence of daily homework makes EMDR highly attractive for patients with chaotic lives or low executive function.
The clinical consensus in 2025 is that EMDR is a robust, effective alternative to pure exposure, particularly for single-incident trauma. For patients who have tried and failed PE, or who cannot tolerate the exposure requirements, EMDR offers an evidence-based path forward.
Brainspotting: Innovation at the Edge of Evidence
Brainspotting emerged from EMDR in 2003, discovered by David Grand. While both use eye position, their application is diametrically opposed. EMDR uses moving eyes to distract and process; Brainspotting uses a fixed gaze to focus and access.
The core tenet is: “Where you look affects how you feel.” The therapist guides the client to scan their visual field while focusing on the somatic activation of a traumatic issue. When a specific point correlates with a spike in distress or a reflexive response (blink, twitch, swallow), this is identified as a “Brainspot.” The client then holds their gaze on this spot, often with the aid of a pointer, to facilitate deep processing.
Grand argues that the fixed gaze accesses the midbrain, specifically the superior colliculus, and subcortical regions directly, bypassing the neocortex. The neuroscience of Brainspotting suggests the retina, composed of brain tissue, has a direct pathway to the superior colliculus, which orchestrates orienting responses. By anchoring the eye, Brainspotting theoretically inhibits the cortical “flight” response and forces the subcortical brain to process encapsulated memory.
However, this mechanistic explanation is currently speculative. While consistent with principles of neuroanatomy, there is limited fMRI or PET scan data directly confirming that Brainspotting selectively activates the midbrain in the way proponents claim. Skeptics argue these neuro-sounding explanations are metaphorical rather than literal.
Despite the lack of mechanistic proof, clinical adoption of Brainspotting is surging. Therapists report it is “gentler” and “deeper” than EMDR, allowing access to pre-verbal or developmental trauma that EMDR sometimes misses.
The evidence base for Brainspotting is in the “emerging” phase. A key 2017 study by Hildebrand et al. compared Brainspotting to EMDR in 76 patients. The results showed no significant difference in efficacy: both treatments significantly reduced PTSD symptoms. This non-inferiority finding is critical, as it suggests Brainspotting may be a valid alternative to the established EMDR protocol.
Additional research has found Brainspotting effective in reducing distress comparable to EMDR.
Critics point to small sample sizes and the lack of independent replication outside the Brainspotting community. Until large-scale RCTs are conducted, Brainspotting remains classified as “experimental” by insurance and guideline bodies. But clinical adoption is surging, particularly among therapists working with complex trauma. We’ve written extensively about how Brainspotting has changed our clinical practice.
DBT-PTSD: The Answer for Complex Trauma
Standard PTSD treatments often exclude patients with active suicidality, severe self-injury, or Borderline Personality Disorder, comorbidities that affect a significant proportion of complex trauma survivors. Dialectical Behavior Therapy adaptations have risen to fill this critical gap. The theoretical premise is that emotional regulation must be established before trauma processing can be safe or effective.
Two primary protocols have emerged:
DBT-PE (Harned Protocol): This is an “add-on” to standard DBT following a strict hierarchy. First, standard DBT achieves behavioral control (elimination of self-harm, reduction of interfering behaviors). Once stability is achieved (typically after two months of no self-harm), the DBT PE protocol implements Prolonged Exposure techniques integrated with DBT skills coaching to manage distress.
DBT-PTSD (Bohus Protocol): This more integrated approach, often residential, was developed specifically for Complex PTSD. It blends DBT skills with PE, compassion-focused therapy, and specific modules for trauma-associated disgust and shame, emotions often resistant to standard fear-based exposure. It uses a “skills-assisted exposure” model where skills are applied during the exposure to maintain the window of tolerance.
The efficacy data is compelling. A landmark trial by Bohus et al. compared DBT-PTSD to CPT for women with childhood abuse-related Complex PTSD. The results were striking:
Remission: 58% of the DBT-PTSD group achieved symptomatic remission compared to 41% in the CPT group.
Dropout: The dropout rate was significantly lower in DBT-PTSD (25%) than CPT (39%).
This provides strong evidence that for complex presentations involving childhood abuse and affect dysregulation, an integrated, phase-based approach is superior to standalone trauma-focused therapy. It validates what clinicians working with severe dissociation and complex presentations have long intuited: stabilization before processing is not a detour but the direct route.
A 2024 meta-analysis confirmed that both DBT-PE and DBT-PTSD result in large effects on self-injury and BPD symptoms, alongside moderate effects on PTSD. Specifically, DBT-PE showed a larger effect size for reducing self-injury, highlighting the protective nature of the Harned protocol.
The Polyvagal Question: Clinically Useful, Scientifically Contested
Central to the somatic movement is Stephen Porges’ Polyvagal Theory. It proposes a hierarchical framework for understanding autonomic responses to threat:
Ventral Vagal Complex: The newest system (mammalian), controlling social engagement, safety, and connection via the myelinated vagus.
Sympathetic Nervous System: The mobilization system (fight/flight).
Dorsal Vagal Complex: The oldest system (reptilian), controlling immobilization, shutdown, and dissociation via the unmyelinated vagus.
Clinically, Polyvagal Theory has been transformative. It offers non-pathologizing language for patients to understand their reactions. The concept of “neuroception,” the subconscious detection of safety or threat, helps explain why survivors may feel unsafe even in benign environments. Therapies informed by Polyvagal Theory focus on stimulating the ventral vagus to restore social engagement and down-regulate defensive states.
However, Polyvagal Theory faces significant criticism from evolutionary biologists and neuroanatomists. Critics argue that the anatomical tenets are flawed. Specifically, the claim that the dorsal motor nucleus is exclusively “reptilian” and responsible for massive bradycardia in mammals is disputed. Furthermore, critics contend that Respiratory Sinus Arrhythmia is an imprecise proxy for “ventral vagal tone” and that Porges’ rigid evolutionary hierarchy doesn’t hold up to comparative neuroanatomy.
The current status is a bifurcation: Polyvagal Theory remains highly useful as a clinical heuristic and metaphor for regulation, even if its neuroanatomical literalism is scientifically contested. Practitioners are advised to use the framework for its therapeutic utility while being cautious about making precise neurobiological claims. This pragmatic position is increasingly common in the field.
Neuromodulation: Technology Meets Trauma
The technological frontier of bottom-up therapy involves directly modulating brain activity without requiring cognitive engagement.
Neurofeedback provides the brain with real-time information about its own electrical activity, training neural circuits toward regulation. Alpha-Theta training, which aims to increase theta waves relative to alpha waves, induces a state of deep relaxation where traumatic imagery can be processed without accompanying hyperarousal. Meta-analyses from 2024 suggest neurofeedback has moderate-to-large effects on PTSD symptoms compared to waitlist controls, though sham-controlled studies show mixed results, indicating a potential placebo component.
Infra-Low Frequency (ILF) neurofeedback targets ultra-slow brain fluctuations believed to regulate the core arousal architecture of the brainstem. While clinical reports describe rapid stabilization of unstable nervous systems, the RCT evidence for ILF is still sparse compared to standard band training. We’ve explored these approaches in our discussion of QEEG brain mapping and neurostimulation.
Transcranial Magnetic Stimulation (TMS) uses magnetic fields to induce electrical currents in targeted brain regions, typically the dorsolateral prefrontal cortex. A massive 2025 multisite study of 756 veterans found that intermittent Theta Burst Stimulation (which takes only 3 minutes per session compared to 37 minutes for standard TMS) was non-inferior to standard protocols, with response rates for PTSD around 65% and remission around 48%. VA research confirms these findings.
Neuroimaging suggests TMS works by strengthening functional connectivity between the Executive Control Network and the Default Mode Network, which is often disrupted in PTSD. Despite promising results, the VA/DoD guidelines still classify TMS evidence as “insufficient” to recommend as standalone first-line treatment, largely due to heterogeneity of protocols and lack of long-term follow-up data. TMS is currently best positioned as an augmentation strategy for treatment-resistant cases.
Stellate Ganglion Block (SGB) involves injecting a local anesthetic into sympathetic nerve tissue in the neck, conceptualized as a “physiological reset” for the sympathetic nervous system. Evidence is mixed: a major RCT found no significant difference between SGB and sham injection at one month, suggesting a strong placebo effect, while case series report high satisfaction and immediate relief.
The emerging view is that SGB may function as a window of opportunity: by temporarily lowering physiological noise, it may enable patients to engage in trauma-focused therapy they were previously too dysregulated to tolerate. This “SGB-facilitated PE” is a growing area of investigation. We interviewed Dr. James Lynch about SGB for those interested in this approach.
The Future: Biotypes and Personalized Medicine
The most profound insight emerging from 2025 research is that the search for a single “best” therapy is a category error. PTSD is biologically heterogeneous. The failure of MDMA-assisted therapy to gain FDA approval in 2024, due to concerns over functional unblinding, has accelerated the pivot toward stratified psychiatry.
Researchers are now using QEEG and fMRI to identify biotypes:
The Hyperarousal Biotype: Characterized by excessive beta activity and amygdala reactivity. These patients may respond best to SGB, alpha-theta neurofeedback, or exposure therapies that prioritize habituation.
The Dissociative Biotype: Characterized by excessive delta/theta activity and midline cortical inhibition. These patients often fail standard PE (due to emotional numbing) and may respond better to stabilization therapies like DBT-PTSD, Brainspotting, or ILF neurofeedback.
The future lies in precision medicine: assessing a patient’s neural and physiological profile before assigning treatment. The days of assigning every patient to CPT because “it’s the guideline” are ending, replaced by algorithms that match the biological pattern to the mechanism of the therapy.
This aligns with how we understand trauma as fundamentally heterogeneous. Different traumas create different patterns in different nervous systems. Matching treatment to pattern is more important than declaring any single therapy the universal answer.
Clinical Implications: What This Means for Treatment
For clinicians, the mandate is integration. The structural rigor of CBT protocols remains valuable, but it must be embedded within a somatic understanding of safety and regulation. No single approach serves all patients.
For patients who can tolerate exposure and whose trauma is primarily fear-based, PE and CPT remain excellent options with deep evidence bases. Written Exposure Therapy offers a briefer, better-tolerated alternative for those who struggle with the homework demands of traditional protocols.
For patients with complex trauma, childhood abuse, or significant affect dysregulation, DBT-PTSD or stabilization-first approaches are likely superior. The data no longer supports forcing these patients into exposure before they have the regulatory capacity to tolerate it.
For patients with primarily somatic presentations, chronic pain comorbidity, or a history of treatment dropout, Somatic Experiencing and EMDR offer paths that don’t require extensive verbal processing of the narrative.
For patients with dissociative presentations or pre-verbal trauma, Brainspotting may access material that other approaches miss, though clinicians should be transparent about its emerging evidence base.
For treatment-resistant cases, neuromodulation (TMS, neurofeedback) offers augmentation strategies that can shift the biological substrate enough to make psychological treatment effective.
The path forward for trauma treatment is not choosing sides in “therapy wars.” It is the rigorous validation of biomarkers that can predict which patient needs which therapy, finally closing the gap between the promise of our protocols and the reality of our outcomes.
The Bottom Line
The landscape of trauma therapy in 2025 is defined by a productive tension between rigor and innovation. Prolonged Exposure and CPT remain the academic anchors, supported by the deepest evidence base. But the field has decisively moved past the idea that these protocols are sufficient for all sufferers.
Somatic Experiencing and EMDR have cemented their place as essential alternatives, particularly for those with somatic comorbidities or a history of treatment dropout. Brainspotting and neurofeedback, while still maturing in their empirical validation, offer critical tools for accessing the subcortical substrates of trauma that talk therapy cannot reach. DBT-PTSD has set a new standard for Complex PTSD, proving that integrated, phase-based care is superior to pure exposure for the most vulnerable patients.
The research is clear: the brain cannot function without proper regulation. Trauma is not just a disorder of memory or cognition. It is a disorder of the autonomic nervous system, the body-brain, the entire organism. Effective treatment must address all of these levels.
And increasingly, we have the tools to do so.
References and Further Reading
Established Protocols:
VA PTSD: Cognitive Processing Therapy
APA: PTSD Treatment Guidelines
ISTSS: International Practice Guidelines
VA PTSD: Written Exposure Therapy
The Efficacy-Effectiveness Gap:
PMC: Dropout Rates in Community PTSD Treatment
PMC: Non-Response Rates in PTSD Treatment
PMC: Top-Down to Bottom-Up Processing
Somatic and Eye-Based Therapies:
PubMed: Somatic Experiencing RCT (Brom et al.)
PMC: Somatic Experiencing Effectiveness Review
PMC: Somatic Therapy Acceptability in Safety-Net Settings
PubMed: EMDR vs TF-CBT Meta-Analysis
Mediterranean Journal of Clinical Psychology: Brainspotting vs EMDR
PMC: Brainspotting Efficacy Research
Complex PTSD:
PMC: DBT-PTSD vs CPT Trial (Bohus et al.)
PMC: DBT Variants for PTSD Meta-Analysis
Neuromodulation:
PMC: Neurofeedback for PTSD Meta-Analysis
PubMed: TMS Theta Burst Stimulation for PTSD
NCBI: Stellate Ganglion Block Evidence
Theoretical Frameworks:
PubMed: Polyvagal Theory Critiques
Journal of Psychiatry Reform: Polyvagal in Practice
PMC: PTSD Biotypes and Neural Biomarkers


















0 Comments