The Archaeology of a Label: What We Forgot About Diagnosis and Why It Matters Now
By Joel Blackstock, LICSW-S | Clinical Director, Taproot Therapy Collective
Part II of A Critical Investigation into the Document That Defines American Mental Health
Contents
We Have to Go Back Further
In Part I of this investigation, we walked through the history of the DSM version by version. We traced the arc from the dynamic “reaction” model of DSM-I, through the checklist revolution of DSM-III, the false epidemics of DSM-IV, and the fractured compromise of DSM-5. We saw how each revision responded to different pressures: insurance companies, pharmaceutical interests, the anti-psychiatry movement, and the NIMH’s demands for biomarkers. We saw a document shaped more by professional survival than by scientific discovery.
But I realized, sitting with all of this, that we were missing something. We were examining the DSM as if it invented the idea of psychiatric diagnosis. It didn’t. The DSM inherited a set of assumptions about what diagnosis is, what it’s for, and what kind of thing a “mental disorder” even is. And those assumptions go back centuries. In some cases, millennia. If we want to understand why the DSM fails in the ways it fails, we have to understand what it thinks it’s doing when it diagnoses someone. We have to ask: what is the history of labeling human suffering?
This is not an argument for returning to shamanism or mysticism or Freudian free association. It’s an argument that the ancient healers, the medieval physicians, and even the early psychoanalysts understood something that the checklist model of Evidence Based Practice has systematically forgotten. They understood that naming a condition is never neutral. The act of diagnosis is always embedded in a theory of what humans are, what they’re for, and what “health” even means. The DSM claims to be “atheoretical,” just describing symptoms without taking a position on causes. But that claim is itself a theory, and a deeply impoverished one.
The thesis of this essay is simple: American psychiatry in the 1970s was on the verge of losing its scientific legitimacy entirely. Internally, many doctors suspected it was pseudoscience. Externally, the public increasingly saw it as a system of repressive social control. What saved the profession was, ironically, the most severe mental illnesses: schizophrenia and extreme bipolar disorder. These were conditions where you could give someone a pill and watch something dramatic happen. The dopamine disorders legitimized the pill. But in the process of saving itself, psychiatry amputated the therapeutic relationship from the diagnostic process. It traded meaning for reliability. And we’re still living with the consequences.
Checklists could work, in principle. But they have to work forward, not backward. You have to start with symptoms, with observations, with data about how human suffering actually clusters, and then figure out what the categories are. Robert Spitzer did the opposite. He started with the categories that psychiatrists already believed in and worked backward to define them. This was politics, not science. And it locked us into a system that cannot be fixed from within because its foundations are compromised.
Part I: What Is a Diagnosis, Anyway?
The Ancient Problem: When the Gods Made You Mad
Before there were psychiatrists, there were priests. And before there were diagnostic manuals, there were myths.
The ancient Greeks had a word for what we now call mental illness: mania. But mania didn’t mean what we mean by it. When Dionysus drove the women of Thebes to tear King Pentheus limb from limb, that was mania. When Ajax slaughtered a flock of sheep believing them to be his enemies, that was mania. When the Oracle at Delphi spoke in tongues, possessed by Apollo, that too was a kind of divine madness.
The crucial point is this: for the ancients, madness was not a malfunction. It was a communication. The gods were speaking through the afflicted person. The “symptoms” were messages that required interpretation, not suppression. The healer’s job was not to eliminate the madness but to understand what it meant. What did the gods want? What did the person’s soul require?
This is alien to our modern sensibility, but sit with it for a moment. If you believed that hearing voices meant a god was trying to tell you something, your entire approach to treatment would be different. You wouldn’t try to make the voices stop. You’d try to figure out what they were saying. You might fast, or pray, or go on a pilgrimage. The “disorder” would be understood as a crisis of meaning, not a broken neurotransmitter.
I’m not saying the Greeks were right. I’m saying they had a coherent framework that gave suffering a place in the cosmic order. The DSM has no such framework. It just lists symptoms.
The Hippocratic Turn: From Gods to Humors
Around the fifth century BCE, something shifted. The Hippocratic physicians, the founders of Western medicine, started arguing that madness wasn’t divine. It was natural. Specifically, it was a disorder of the four humors: blood, phlegm, yellow bile, and black bile.
The famous Hippocratic text On the Sacred Disease (about epilepsy) makes this argument explicitly. The author is furious at people who attribute seizures to the gods. “It is not, in my opinion, any more divine or sacred than other diseases,” he writes, “but has a natural cause.” The cause, he argues, is an excess of phlegm in the brain.
This was revolutionary. By relocating madness from the heavens to the body, the Hippocratics created the conceptual space for medicine. But notice what they kept: the idea that the patient’s condition means something. The humors weren’t just chemicals. They were connected to the seasons, the elements, the temperaments. A melancholic person (too much black bile) wasn’t just sick. They had a particular kind of soul, a particular relationship to the world. The diagnosis told you something about who they were.
The humoral system dominated Western medicine for nearly two thousand years. Galen systematized it in the second century. Medieval physicians refined it. Even into the Renaissance, doctors were still prescribing bloodletting to reduce excess blood, or purgatives to eliminate black bile. The treatments were often useless or harmful, but the framework was coherent. Illness was an imbalance. Health was harmony. The doctor’s job was to restore the patient’s proper relationship to their own nature and to the cosmos.
The Enlightenment Rupture: Mind as Machine
Then came Descartes, and everything fell apart.
Descartes’ famous division of reality into res cogitans (thinking stuff) and res extensa (extended stuff) created a philosophical puzzle that we still haven’t solved. The body was a machine, operating according to mechanical laws. The mind was something else. A ghost in the machine. Immaterial, indivisible, free.
This dualism made modern science possible. By declaring the body to be pure mechanism, Descartes gave permission to dissect it, measure it, experiment on it without worrying about the soul. But it created a massive problem for psychiatry. If the mind is immaterial, how can it be sick? If mental illness is real, where exactly is it located?
The nineteenth century tried various answers. Phrenologists thought mental faculties were located in specific brain regions that you could feel through the skull. Asylum doctors looked for brain lesions in their deceased patients. But the results were disappointing. You could find brain damage in some cases of madness, but not in others. Many conditions that looked like diseases, such as melancholia, hysteria, and neurasthenia, seemed to have no physical basis at all.
This is the dirty secret that haunts psychiatry to this day: we still don’t have biomarkers for most mental disorders. After 150 years of looking, we cannot point to a blood test or a brain scan that definitively diagnoses depression, or anxiety, or PTSD. The DSM knows this. The committees know this. But the whole edifice of “medical model” psychiatry is built on the assumption that such markers exist and will eventually be found. The biomarkers have been “coming soon” since 1980.
Kraepelin and the Birth of the Checklist
The modern psychiatric diagnosis was essentially invented by one man: Emil Kraepelin, a German psychiatrist working in the late nineteenth and early twentieth century.
Kraepelin’s innovation was simple but profound. He stopped trying to find the cause of mental illness and focused instead on the course. He spent decades meticulously observing patients in asylums, tracking their symptoms over time. He noticed that certain clusters of symptoms tended to hang together and follow predictable trajectories. Some patients got sick young, deteriorated steadily, and never recovered. Others had episodes of illness followed by periods of relative health.
From these observations, Kraepelin carved out the two great categories that still structure psychiatry today: dementia praecox (later renamed schizophrenia) and manic-depressive illness (later split into bipolar disorder and major depression). His method was purely descriptive. He didn’t claim to know what caused these conditions or what was happening in the brain. He just described what he saw.
This Kraepelinian approach, describing symptoms without explaining them, is exactly what Robert Spitzer would resurrect in DSM-III. But there’s a crucial difference. Kraepelin spent decades watching patients before he drew any conclusions. He knew his patients intimately. Spitzer’s checklists were designed to make that kind of intimate knowledge unnecessary. You don’t need to know the patient; you just need to count their symptoms.
Freud and the Rebellion Against Labels
Before Spitzer, before the checklists, there was Freud. And whatever else you want to say about Freud, he understood something that the DSM has forgotten: symptoms are not just problems to be eliminated. They’re solutions to deeper problems. They mean something.
Freud’s great insight, one that has been validated over and over by trauma research, even as his specific theories have been abandoned, is that psychological symptoms often represent the return of experiences that couldn’t be processed when they occurred. The hysterical paralysis isn’t random; it’s connected to a memory, a conflict, a wish that couldn’t be acknowledged. The obsessive ritual isn’t meaningless; it’s an attempt to bind anxiety that would otherwise be overwhelming.
In this framework, diagnosis is less important than understanding. What matters is not which box the patient fits into, but what their particular symptoms mean in the context of their particular life. Two patients with identical symptoms might have completely different dynamics. One might be depressed because of unresolved grief; another might be depressed because of suppressed rage; a third might be depressed because their entire way of understanding themselves has collapsed. The checklist sees three cases of “Major Depressive Disorder.” Freud would see three entirely different problems requiring three entirely different approaches.
This is what the DSM threw away. In the name of reliability, getting doctors to agree, it sacrificed meaning. And in doing so, it made itself scientifically useless for finding cures.
Part II: The DSM Chronicle
DSM-I (1952): Medical 203 and the Military Origins
Here’s something that should be a scandal but somehow isn’t: the DSM didn’t emerge from hospitals or research universities. It emerged from the U.S. Army’s need to process soldiers during World War II.
The military had a problem. Millions of young men were being drafted, and a significant percentage of them were cracking under the stress of combat. The Army needed to figure out who was fit for duty, who should be discharged, and who was entitled to a pension. They couldn’t have 500 different psychiatrists writing long essays about each soldier’s childhood. They needed codes. They needed to turn complex human beings into standardized units of data that could be processed by a clerk in Washington.
The solution was Technical Bulletin Medical 203, issued by the War Department in 1943. This document created a standardized nomenclature for psychiatric conditions, the first time American psychiatry had anything like a common language. After the war, the Veterans Administration adopted it. And when the American Psychiatric Association decided to create a unified diagnostic manual in 1952, they essentially copied Medical 203 with minor modifications.
This is the origin story of the DSM. Not a hospital. Not a laboratory. A military bureaucracy trying to manage a logistics problem.
The Gentlemen’s Club: Inside the Committees
If we look inside the closed doors of the committees for the DSM-I and DSM-II, the vibe wasn’t “military processing” at all. It was a gentlemen’s club. The controversies inside those rooms weren’t about data or NDAs. They were intellectual brawls between conflicting philosophies of the soul.
The biggest controversy inside the DSM-I (1952) committee was that the people writing the book didn’t actually believe in diagnosis. The dominant figure was the spirit of Adolf Meyer, the “Dean of American Psychiatry.” Meyer hated labels. He believed every patient was a unique biopsychosocial story.
On one side, you had the Census Bureau types who wanted distinct boxes (“Schizophrenia,” “Manic Depression”) to count people. On the other side, you had the Meyerians who argued that putting a label on a patient was an insult to their complexity.
The committee solved this by adding the word “Reaction” to almost everything. You didn’t have “Schizophrenia” (a static disease). You had “Schizophrenic Reaction” (a temporary response to life). This was a philosophical coup. It effectively codified the idea that mental illness is not inside the brain, but in the interaction with the world. It was a victory for the “poets” over the “biologists.”
But there was also a power play. The Chair of the DSM-I committee wasn’t just a doctor; he was Brigadier General William Menninger. He had run psychiatry for the US Army during WWII and developed Medical 203. He essentially marched into the civilian committee and said, “This is what the Army uses. Adopt it.”
The civilian academics, East Coast elites, resented the military encroaching on their turf. They viewed the military system as too crude. But Menninger won because he had the prestige of the war victory. The DSM-I is largely a copy-paste of the Army’s “Medical 203.” The controversy was effectively Military Pragmatism conquering Civilian Theory.
The Imperial Unconscious of the DSM-I
If you read the DSM-I with fresh eyes, you’ll notice something uncomfortable: it’s saturated with the assumptions of mid-century American empire.
Start with homosexuality. In DSM-I, it was listed under “Sociopathic Personality Disturbance,” grouped with antisocial behavior and sexual deviations. This wasn’t just ignorance; it was ideology. Gay people were defined as having no moral compass, as fundamentally disordered in their relationship to society. The diagnosis served a function: it justified denying gay people security clearances, government jobs, and basic civil rights.
Or consider the treatment of women. “Hysteria,” a diagnosis applied almost exclusively to women, was still very much alive. The term comes from the Greek word for uterus; the ancient assumption was that women’s mental disturbances came from their wandering wombs. By 1952, nobody believed that literally anymore, but the diagnosis persisted, and it was still gendered. Women who didn’t fit the expected mold, who were too emotional, too sexual, too independent, could be pathologized.
Or consider the implicit racial assumptions. The early DSM had nothing to say about how racism might affect mental health. It couldn’t even conceive of the question. The patient was always an isolated individual with an internal disorder. The social environment was backdrop, not cause. If a Black man in Jim Crow Alabama was depressed, that was his neurochemistry, not his circumstances.
This is what I mean by the imperial unconscious. The DSM-I was written by a small group of white men who took their own worldview as the default human condition. They built a system for categorizing deviance from a norm that was never examined because it didn’t need to be. It was just “how things are.” And we inherited that system.
DSM-II (1968): The International Brawl and the Revolt
By the time of the DSM-II (1968), the committee was fighting a new war: Globalism.
The World Health Organization had just published the ICD-8. They told the Americans: “Stop using your weird Freudian terms. Align with the rest of the world.”
Inside the committee, there was a split. The Internationalists wanted to adopt the European/ICD terms, which were more biological and Kraepelinian. The American Freudians refused to give up terms like “Neurosis” and “Hysteria.” They argued that European psychiatry was “superficial” because it ignored the unconscious mind.
The committee spent months arguing over the word “Hysteria.” The Europeans had banned it, calling it antiquated. The Americans insisted on keeping it. They kept “Hysterical Neurosis” in the DSM-II to appease the American analysts, making the US look scientifically backward compared to Europe.
The biggest difference between these committees and the later ones was the complete lack of data. They didn’t run trials. They sent out letters to prominent psychiatrists asking, “What do you think?” For the DSM-II, they surveyed 12,000 psychiatrists. Only about 10% bothered to reply. The committee shrugged and decided to write what they thought was best anyway.
This cemented the idea that the DSM was just “The Opinions of a Few Old Men in a Room.” There was no mechanism to challenge them because they claimed authority based on Prestige (who they were), not Evidence (what they proved).
The Storm Breaks: Anti-Psychiatry
The 1960s brought everything into question, and psychiatry was not spared.
Thomas Szasz published The Myth of Mental Illness in 1961, arguing that “mental illness” was a category error. The mind isn’t an organ; it can’t be sick the way a liver can be sick. What we call “mental illness” is really just problems in living: moral, social, personal conflicts that we’ve medicalized to avoid dealing with them honestly. Szasz argued that psychiatry was a form of social control masquerading as medicine, allowing the state to lock up inconvenient people without the due process that the criminal justice system would require.
Michel Foucault, in Madness and Civilization, traced the history of how “madness” became “mental illness,” how the asylum replaced the leper colony, how doctors replaced priests, how the “clinical gaze” created new forms of discipline and surveillance. For Foucault, the DSM wasn’t a scientific document; it was a technology of power.
R.D. Laing went further, suggesting that what looked like “madness” might actually be a sane response to an insane world. The schizophrenic wasn’t broken; they were a kind of voyager, someone whose extreme sensitivity to the contradictions of modern life had pushed them into a different way of being. Laing suggested that the psychiatrist’s attempt to “cure” such a person was itself a form of violence.
Laing’s work on schizophrenia was particularly influential. In The Divided Self (1960) and Sanity, Madness, and the Family (1964, with Aaron Esterson), Laing proposed that schizophrenic symptoms were intelligible responses to impossible family situations, particularly “double binds” where the patient received contradictory messages that made any response wrong. This was a direct challenge to the biological model: if schizophrenia was a response to context rather than a brain disease, then the entire medical framework was wrong.
These critiques would have been easy to dismiss if they had remained in the academy. But they didn’t. They reached the public. One Flew Over the Cuckoo’s Nest (both the novel and the film) depicted psychiatrists as agents of conformity, using diagnosis and treatment to crush the human spirit. The image of psychiatry shifted from benevolent healer to authoritarian enforcer.
Rosenhan: The Emperor Has No Clothes
Then came David Rosenhan, and everything broke.
Rosenhan’s 1973 study, “On Being Sane in Insane Places,” was a masterpiece of experimental humiliation. He recruited eight healthy people, including a psychiatrist, a pediatrician, a painter, and a housewife, and sent them to psychiatric hospitals with the same complaint: they were hearing a voice that said “empty,” “hollow,” “thud.”
Beyond that single fabrication, they were instructed to behave completely normally. They gave truthful answers about their lives. They didn’t simulate any other symptoms. They acted exactly as they would in ordinary life.
All eight were admitted. All were diagnosed with serious mental illness: seven with schizophrenia, one with manic-depressive psychosis. And here’s the thing that really stung: once they were admitted and stopped reporting the hallucination, the staff couldn’t tell they were sane. Normal behaviors were reinterpreted as pathological. When they took notes, the nurses recorded “patient engages in writing behavior.” When they paced out of boredom, it was documented as “agitation.”
The average hospital stay was 19 days. One person was held for 52 days. When they were finally released, they weren’t declared sane. They were diagnosed “schizophrenia in remission.” The label was permanent, just temporarily inactive.
Rosenhan’s conclusion was devastating: “It is clear that we cannot distinguish the sane from the insane in psychiatric hospitals.” The supposed expertise of the psychiatrist was a myth. The diagnosis resided in the context, the “insane place,” not in the patient.
The Homosexuality Vote
The final blow came from an unexpected direction: gay rights activists.
In DSM-II, homosexuality was listed as a “Sexual Deviation.” This wasn’t just a theoretical category; it had real consequences. Gay people couldn’t get security clearances. They couldn’t hold certain government jobs. They could be involuntarily committed. The diagnosis was a weapon.
Activists led by Frank Kameny realized that as long as they were officially “sick,” they would never achieve civil rights. So they went to war. They didn’t write polite letters. They stormed the stage at the 1970 APA convention in San Francisco, grabbed the microphone, and shouted at the assembled psychiatrists.
And it worked.
Robert Spitzer, then a young committee member, brokered a compromise. In 1973, the APA voted to remove homosexuality from the DSM. It was the first time a “disease” had been cured by a political vote.
This might sound like progress, and it was. But it also proved something that the critics had been saying all along: the DSM wasn’t science. It was politics. The disorders weren’t discovered in nature; they were voted into existence by committees. What the vote could give, the vote could take away.
The Dopamine Miracle: Schizophrenia Saves Psychiatry
Here’s the irony that nobody talks about: what actually saved psychiatry wasn’t the checklists. It was schizophrenia. In the 90’s ADHD was the focus of psychiatry, in the aughts it was autism, now it is trauma. In the 1970s schizophrenia represented the most broad encounter point for the public to see mental illness and the biggest expenditure of the psychiatric mental health system.
By the early 1970s, psychiatry was in crisis. The anti-psychiatry movement had devastated public trust. Rosenhan had humiliated the profession. Insurance companies were questioning why they should pay for treatments that seemed indistinguishable from philosophy. The field was on the verge of losing its medical legitimacy entirely.
And then the antipsychotics started working.
Chlorpromazine (Thorazine) had been introduced in the 1950s, but it took time for its implications to sink in. By the 1970s, psychiatrists could do something dramatic with severe psychotic disorders. You could take a person who was homeless, hallucinating, completely unable to function, give them a pill, and watch them stabilize. A patient could go from raving to coherent in a matter of days. All of the 1960s research, mainly by the VA about talk therapy and psychoanalysis for schizophrenia proved that it did next to nothing to reduce the symptoms of schizophrenia. This research plays an enormous part in the shift from psychiatry from therapy to medicine. If schizophrenia could be cured with a pill maybe everything could. We just needed to find more pills to treat more conditions.
Medication made progress that was visible. This was measurable. This was undeniable. Whatever the critics said about psychiatry being social control or pseudoscience, you couldn’t argue with a psychotic patient who got better on medication.
The dopamine hypothesis of schizophrenia emerged from this clinical success. All the effective antipsychotics blocked dopamine receptors. Drugs that increased dopamine (like amphetamines) could trigger psychotic symptoms. Therefore, the theory went, schizophrenia must involve dopamine dysfunction.
This was enormously important for the profession’s self-image. For the first time, psychiatry had something that looked like real medicine: a biological theory, a drug that targeted that biology, and clinical results that seemed to validate the whole enterprise.
The Legitimization Cascade
The success with schizophrenia and severe bipolar disorder became psychiatry’s trump card. It legitimized everything else.
The logic went something like this: we can treat schizophrenia with medication that affects brain chemistry. Therefore, mental illnesses are brain diseases. Therefore, all our diagnostic categories must correspond to real biological entities. Therefore, the DSM is scientific.
But notice the leap. The fact that antipsychotics help with schizophrenia doesn’t prove that “major depressive disorder” or “generalized anxiety disorder” are also biological entities in the same way. The success with the dopamine disorders was used to justify the entire medical model, even for conditions where the evidence was much weaker.
This is what saved psychiatry in the 1970s. Not the checklists. Not scientific rigor. The fact that you could show a skeptic a psychotic patient, give them a pill, and demonstrate improvement. The most dramatic cases provided cover for the entire enterprise.
But the price was enormous. In rushing to embrace the biological model, psychiatry abandoned the therapeutic relationship. If mental illness is just brain chemistry, then treatment is just medication management. You don’t need to understand the patient’s life story. You don’t need to sit with them for an hour exploring their fears and hopes. You just need to identify the symptoms, pick the right drug, and adjust the dose.
The thing that worked (medication for severe mental illness) legitimized the abandonment of the thing that also worked (therapy). And we’ve been living with that trade-off ever since.
DSM-III (1980): Spitzer’s Revolution
The Crisis of Reliability
Two major events made the need for revision urgent.
The Rosenhan Experiment showed that psychiatrists couldn’t distinguish the sane from the insane. The US-UK Diagnostic Project showed that American doctors diagnosed schizophrenia twice as often as British doctors for the exact same patients. The labels meant different things depending on which side of the Atlantic you were on.
The APA realized that if two doctors couldn’t agree on a diagnosis, the whole system would collapse. Insurance companies would stop paying. Research would be impossible. The government would stop funding.
The Wartime General
Into this chaos walked Robert Spitzer.
Spitzer was an unlikely revolutionary. He was awkward, obsessive, lacking in social graces. He had trained as a psychoanalyst but never really fit the mold. He was too concrete, too focused on measurable things. He had been “kicked upstairs” to administrative roles because he lacked the clinical warmth the profession prized. But that rejection may have fueled his desire to remake the entire system.
The APA gave him the job because he had proven he could navigate political minefields. He had brokered the homosexuality compromise. He had shown he could rewrite the bible without destroying the organization. Now they needed someone who could save the profession itself.
Spitzer was obsessed with inter-rater reliability, getting doctors to agree. He had already developed the Research Diagnostic Criteria (RDC), which used checklists instead of vague feelings. The APA needed that checklist style to survive.
The Atheoretical Compromise
Until Spitzer, the DSM was heavily influenced by Freudian psychoanalysis. It described disorders based on causes: “unconscious conflict,” “neurosis,” “depression as anger turned inward.” You couldn’t make a diagnosis without taking a position on etiology, on what was happening in the patient’s unconscious mind.
Spitzer hated this. You can’t measure an unconscious conflict. You can’t get two analysts to agree on what’s being repressed. The whole framework was too subjective, too literary, too much like poetry.
His solution was radical: make the DSM “atheoretical.” Don’t say why people are depressed, whether it’s their mother, their childhood, their brain chemistry. Just list symptoms. If you have five of nine symptoms for two weeks, you have Major Depressive Disorder. Period.
This was a diplomatic masterstroke. It allowed Freudians and biological psychiatrists to use the same codes. They could disagree about causes while agreeing on descriptions.
But it was also a philosophical retreat. By abandoning the “why,” the DSM stripped diagnosis of its meaning. It became a taxonomy of surfaces.
The Typewriter Parties
This is where it gets weird. Spitzer would gather experts in a room, sometimes at Columbia, sometimes at his house, and essentially hold symptom-shouting contests.
Imagine the scene. A dozen psychiatrists who have been arguing about “depression” for thirty years. Spitzer at his typewriter. He throws out a symptom: “Feeling worthless.”
“Okay, if the patient feels worthless on Tuesday but not Wednesday, does that count?”
Someone says yes. Someone says no. They argue.
“If he feels worthless because he just lost his job, is that a symptom or just a normal reaction? VOTE!”
More arguing. Spitzer types whatever the majority agrees on.
“How many weeks of sadness before it’s Major Depression? Two? Four? Six?”
Shouting. Horse-trading. Finally someone yells, “Two weeks!” and Spitzer types it before anyone can object.
This was not science. This was politics. It was a feat of consensus-building, a way of getting stubborn experts to agree on something, anything, so that the paperwork could be standardized. Spitzer was chasing a statistic called Kappa (a measure of how often two raters agree on a diagnosis), and he realized the only way to get high Kappa was to remove judgment from the equation. Strip away the nuance. Force binary choices. Turn the doctors into robots following a checklist.
The Purge of the Analysts
Spitzer had another agenda, one that was more personal: he wanted to destroy the power of the psychoanalysts.
Until DSM-III, the language of psychiatry was Freudian. Disorders were defined by causes. “Neurosis” implied unconscious conflict. “Hysteria” implied repressed sexuality. “Depression” was described as “anger turned inward.” You couldn’t make a diagnosis without taking a position on what was happening in the patient’s mind.
Spitzer stripped it all out. DSM-III was “atheoretical.” It didn’t say why you were depressed. It just listed symptoms. If you met criteria, you had the disorder.
The psychoanalysts were furious. They saw this as a coup, a hostile takeover disguised as science. And they weren’t entirely wrong. Spitzer wasn’t discovering that their approach was false; he was declaring that their approach didn’t count anymore. The new rules simply excluded the kind of knowledge they had.
The Backwards Method and Why It Matters
Here’s the thing nobody talks about: Spitzer’s method was completely backwards from how science is supposed to work.
The scientific ideal would be to gather data first. You would observe thousands of patients, record all their symptoms, and use statistical methods to see which symptoms cluster together. Maybe you’d discover that what everyone calls “depression” is actually three different conditions that need different names. Maybe you’d find that “anxiety” and “depression” overlap so much they shouldn’t be separate categories. You’d let the data tell you where the boundaries are.
This approach has a name: factor analysis. It’s what the HiTOP model does today. And if Spitzer had done it this way, the DSM would look completely different.
We probably wouldn’t have separate categories for Depression and Anxiety. The statistics show they’re almost always comorbid. We might have a giant category called “Negative Affect” instead.
And the dopamine disorders would look completely different. We might have a spectrum of “Psychosis Proneness” rather than the rigid wall between Schizophrenia and Bipolar. Because here’s what clinicians know but the DSM obscures: these conditions share a common neurological route. Even if we don’t understand that route completely, even if the exact mechanisms remain fuzzy, we know they’re based on very similar processes. The same medications often work for both. The same neurotransmitter systems are implicated. Patients sometimes shift from one diagnosis to the other over the course of their illness, which shouldn’t happen if these were truly distinct diseases.
The walls between Schizophrenia and Bipolar aren’t big walls. They’re not like the wall between a broken leg and pneumonia. They’re more like the wall between slightly different presentations of the same underlying vulnerability. Clinicians know this because the conditions are sometimes genuinely hard to tell apart. A patient in a manic episode with psychotic features looks a lot like a patient with schizoaffective disorder. A patient with schizophrenia who has prominent mood symptoms blurs into bipolar territory. The DSM draws sharp lines, but the clinical reality is fuzzy.
If we had started with symptoms and let them cluster naturally, we might have ended up with a “psychosis spectrum” that captured the underlying commonality. We might have dimensional measures of thought disorder, mood instability, negative symptoms, and cognitive impairment that could be combined in different ways for different patients. Instead, we have categorical boxes that force clinicians to make arbitrary distinctions that don’t map onto biology or treatment response.
Why Spitzer Worked Backwards
But Spitzer couldn’t do it this way. Why? Because the establishment already existed. Psychiatrists had been using terms like “schizophrenia” and “depression” and “anxiety” for decades. They had built their careers around these categories. Their textbooks were organized around them. If Spitzer had announced that factor analysis revealed “schizophrenia” wasn’t real, that it was actually three different things with three different names, the profession would have rejected his book entirely. Nobody would use it.
So Spitzer worked backwards. He started with the names, the categories that psychiatrists already believed in, and then tried to get them to agree on what symptoms defined each name.
Step 1: Take a diagnosis that psychiatrists already “felt” was real (e.g., “Melancholia” or “Schizophrenia”).
Step 2: Gather a room full of experts on that specific topic.
Step 3: Ask them, “When you see a patient with this, what does it look like?”
Step 4: Argue until they agree on a list of roughly 5 to 9 symptoms that are easy to spot.
He didn’t find the symptoms and build the house; he had the house (the label) and looked for bricks (symptoms) to build the walls.
The Political Problem
If Spitzer had done it the right way, starting with symptoms and letting them cluster naturally, the political complications would have been enormous.
Imagine presenting a room full of psychiatrists with a patient and asking: “What would you diagnose this person with?” If they disagreed, which they inevitably would, it would expose the unreliability of the whole system. It would be another Rosenhan experiment, showing that doctors couldn’t agree.
But if you instead asked, “For patients YOU have already diagnosed with depression, what symptoms do you see?”, you could get agreement. The doctors weren’t being tested. They were being consulted. Their expertise was being respected, not challenged.
This is why the typewriter parties worked. One psychiatrist might say, “You have a depression for at least two weeks.” Another might say, “No, that could just be a dysregulation; it has to be at least four weeks.” Spitzer would sit them down and make them compromise. “Let’s say two weeks, but we’ll add duration criteria and exclusions.”
This was a feat of politics, not science. It produced reliability (doctors agreeing with each other) but not validity (the categories mapping onto reality).
Checklists Can Work, But Only Forward
Here’s the crucial point: checklists aren’t inherently bad. They can be a valid scientific tool. But they have to work forward, not backward.
A forward checklist starts with observations. You observe hundreds or thousands of patients. You record every symptom you see. You use statistics to find patterns: which symptoms tend to appear together, which predict certain outcomes, which respond to certain treatments. Then you define your categories based on what you found.
A backward checklist starts with the categories you already believe in and defines them however you can get people to agree. This is what Spitzer did. It’s not discovery; it’s codification of existing prejudices.
The DSM’s checklists were backwards from day one. They locked in the assumptions of mid-20th century psychiatry and made them very difficult to change. Every subsequent revision has been constrained by what Spitzer set up. You can’t easily dissolve “Depression” and “Anxiety” into a single spectrum because the entire infrastructure, the textbooks, the billing codes, the treatment guidelines, is built around them being separate.
This is the trap we’re still in. The backwards method created a system that resists correction. The more entrenched the categories become, the harder they are to question. And the harder they are to question, the more entrenched they become.
DSM-IV (1994): The Conservative Correction and the False Epidemics
Allen Frances, who chaired the DSM-IV task force, explicitly did not want to be Robert Spitzer.
Spitzer’s revolution had been explosive, a massive expansion of diagnostic categories, a complete restructuring of psychiatric thinking. Frances wanted the opposite: stabilization. His mantra was “no new diagnoses without hard data.” He ran a conservative, committee-heavy process designed to prevent the reckless expansion of the manual.
And yet, despite his caution, DSM-IV triggered three massive epidemics that Frances has spent the rest of his career apologizing for: ADHD, Bipolar II, and Autism. Frances spent the rest of his career apologizing for this and explaining why he thought it happened. In essence, Frances maintains that any change in the manual that can be misused will be misused, and he expresses regret that the DSM-IV inadvertently opened the door to pathologizing normal human variation, leading to unnecessary treatment and potential harm. I don’t think he’s wrong. I think that people follow incentive structures and the profit motive will always follow one incentive structure.
How did this happen? The committees loosened criteria slightly, not dramatically, just slightly, and the results cascaded beyond anything they anticipated.
The ADHD Explosion
ADHD could now be diagnosed based heavily on teacher reports about classroom behavior. In a school system with increasing demands for standardized testing and decreasing tolerance for behavioral variation, normal childhood restlessness became pathology.
Sami Timimi, a child psychiatrist and critic of the ADHD construct, points out that there is no biomarker for ADHD. No blood test, no brain scan, no genetic assay can diagnose it. The diagnosis serves a social function: it “exonerates” parents and schools. By labeling a distracted child as “diseased,” the school avoids changing its rigid curriculum, and parents avoid blame for family dysfunction. It repackages social problems as a biological defect in the child.
The diagnosis rate exploded. Roughly 10% of American children are now diagnosed with ADHD. Drug companies marketed medications directly to parents and schools. Stimulant prescriptions increased by orders of magnitude. Whatever the DSM-IV committee intended, they created a diagnostic category that could be exploited. This phenomenon has extended into adulthood, with the rise of adult ADHD diagnosis reflecting similar pressures.
The Bipolar II Expansion
The expansion of the bipolar spectrum to include Bipolar II, characterized by depressive episodes and milder “hypomanic” episodes, opened the floodgates. The criteria for hypomania were vague enough that periods of elevated mood, increased productivity, or decreased need for sleep (common experiences during exciting life events) could qualify.
This had massive pharmaceutical implications. Patients who might previously have been diagnosed with depression were now diagnosed with Bipolar II, which changed their treatment protocol entirely, from antidepressants to mood stabilizers and antipsychotics, drugs with far more significant side effect profiles and higher profit margins.
The Autism Spectrum
The introduction of Asperger’s Disorder in DSM-IV expanded the autism umbrella to include individuals with social difficulties but without language delays or intellectual disability. While this brought services to many who needed them, it also captured a vast population of socially awkward but fundamentally neurotypical individuals.
The diagnostic rate went from approximately 1 in 2,500 in the 1980s to 1 in 36 today. This is a staggering increase that cannot be explained by better detection alone. The category expanded to capture more and more of human variation.
The Lesson
Frances learned a bitter lesson: bureaucratic methodologies are inherently inflationary. Once a checklist exists, the pressure from patients (seeking validation), parents (seeking school services), and pharmaceutical companies (seeking customers) forces the gate open.
The conservative couldn’t hold the line because the incentives were all pushing in one direction. Every stakeholder except the patients themselves benefited from broader categories. The criteria became porous. The epidemics resulted.
DSM-5 (2013): The Failed Biological Shift and the NIMH Divorce
The Broken Promise
The DSM-5 Task Force had promised the NIMH something revolutionary. They said: “Give us money and time, and we will find the biomarkers, the genes, the brain scans, that prove these disorders are real.”
They spent fourteen years and $25 million. They failed.
The DSM-5 came out, and it was still just a list of symptoms. Still no real neurobiological markers for any condition or real tests. The science had plenty of data that there were lots of biomarkers for mental health but not in the direction that the DSM-5 was following. Still no biological validation. The categories were still just descriptions of what patients say and do, with no proven connection to underlying biology.
The Bombshell
April 29, 2013. Two weeks before the DSM-5 was scheduled to launch.
Thomas Insel, Director of the National Institute of Mental Health, published a blog post that should have been front-page news. The NIMH, the agency that funds almost all mental health research in the United States, announced that it would no longer use DSM categories to guide its research funding.
Insel wrote: “While DSM has been described as a ‘Bible’ for the field, it is, at best, a dictionary… The weakness is its lack of validity.”
This was extraordinary. The federal government was publicly declaring that the diagnostic manual used by every clinician in America was scientifically invalid. Why are they still using it? This was a clear signal by the arbitrators of science that the field guide was no longer scientific.
Why This Should Have Been Bigger News
Think about what this means. For three decades, the NIMH had forced researchers to use DSM categories. If you wanted a grant to study depression, you had to study “DSM Depression,” patients who met the specific checklist criteria. If you wanted to study schizophrenia, you had to study “DSM Schizophrenia.”
But Insel realized this was sabotaging the research. He called it the “bucket of sludge” problem.
Imagine trying to find a cure for “fever.” You gather a thousand patients who all have elevated body temperature. Some have the flu. Some have cancer. Some have heat stroke. Some have autoimmune disorders. You mix them all together and run drug trials.
The trials will fail. Of course they’ll fail. You’re studying ten different biological problems as if they were one thing. The drug that works for the flu patient will do nothing for the cancer patient. Your statistics will show no effect because the effects are being averaged across unrelated conditions. I for one believe that PTSD is a useless diagnosis because it is really 3 different disorders. Bessel Van der Kolk’s suggestion that “Complex Trauma” be included was ignored by the committee.
This is exactly what’s been happening in psychiatric research. “Major Depressive Disorder” is not one thing. It’s a dozen different things, different genetics, different neural circuits, different causes, all lumped together because they share surface symptoms. No wonder we haven’t found cures. We’ve been looking for a single key to open a dozen different locks.
RDoC: The Empty Matrix
When the NIMH walked away from the DSM, they announced a replacement: the Research Domain Criteria (RDoC).
RDoC is not a diagnostic manual. You can’t use it to diagnose a patient or bill insurance. It’s a research framework, a grid with rows (constructs like “Fear,” “Working Memory,” “Reward Responsiveness”) and columns (units of analysis like “Genes,” “Molecules,” “Circuits,” “Behavior”).
Most of the boxes in that grid are empty. That’s the point. The NIMH’s message to researchers was: “Stop studying ‘Depression.’ Start studying the specific brain circuits that control mood. We don’t know what goes in these boxes yet. Your job is to find out.”
This was intellectually honest and scientifically sound. But it left clinicians stranded.
A therapist in 2013 couldn’t say to a patient, “You have a deficit in your Negative Valence System.” Insurance companies couldn’t bill for “Acute Threat Circuitry Malfunction.” The DSM might be scientifically invalid, but it was the only game in town for actually treating people.
So the field split in half. Clinicians kept using DSM-5 because they had no alternative. Researchers moved to RDoC because that’s where the grant money went. The people studying mental illness and the people treating it were now operating in different paradigms.
It’s worth noting that the NIMH itself said that RDoC was not ready for the task that they were now assigning it. They had so little faith in the DSM they were now turning to a system that they said would probably be completed in about two decades. It wasn’t completed and they still thought that it was a better system than the DSM-5. Not only that, it was a system that they were saying was two decades from being robust, two decades. The NIMH still thought that it was better than the direction that the DSM committee was moving in. And this is all before the book was even published.
DSM History Summary Table
| DSM Version & Year | The Dominant Paradigm & Ideology | Primary Driving Forces & Pressures | Defining Characteristics & Methodology | Major Historical & Cultural Outcomes |
| DSM-I (1952) | The Psychodynamic “Reaction” Model Influenced by Adolf Meyer; viewed disorders not as static diseases but as dynamic responses to life and environment. |
Military Pragmatism: Emerged directly from the US Army’s WWII need to process soldiers (Technical Bulletin Medical 203) and post-war VA administration needs. Gentlemen’s Club Politics: A clash between military pragmatists (Gen. Menninger) and academic civilian theorists. |
The “Imperial Unconscious”: Saturated with mid-century American assumptions (e.g., homosexuality as “sociopathic,” gendered views of hysteria, ignorance of racial context). The “Reaction” Suffix: Almost all diagnoses were labelled reactions (e.g., “Schizophrenic Reaction”), codifying the idea that illness was in the interaction with the world, not just inside the brain. |
Established the first standardized nomenclature for American psychiatry, fundamentally rooted in military logistics rather than clinical research or hospital data. |
| DSM-II (1968) | Fractured Psychoanalytic Retained Freudian language but increasingly disconnected from its original depth; a “gentlemen’s club” relying on prestige rather than data. |
Globalism & WHO Pressure: The need to align American terms with the international ICD-8, which was more biological/European. Internal Conflict: A brawl between “Internationalists” wanting alignment and American analysts refusing to give up terms like “Neurosis.” |
Data-Free Consensus: Based on surveys with abysmal response rates (10%), resulting in the “opinions of a few old men in a room.” Retaining “Hysteria”: Kept antiquated psychoanalytic terms to appease American analysts, making the US look scientifically backward compared to Europe. |
The 1973 Gay Rights Victory: Following activist protests, Robert Spitzer brokered a political compromise to remove homosexuality as a disorder, proving definitively that diagnoses were political votes, not natural discoveries. |
| DSM-III (1980) | The “Atheoretical” Checklist Revolution A philosophical retreat from etiology (cause) to surface description. The resurrection of Kraepelin’s descriptive method without his long-term observation. |
The Crisis of Legitimacy: Psychiatry was threatened by anti-psychiatry critiques (Szasz, Foucault), the Rosenhan experiment exposing unreliability, and insurance companies demanding standardized criteria for payment. | Spitzer’s “Backwards Method”: Started with pre-existing labels and used consensus-building (“typewriter parties” with shouting experts) to define symptoms. Reliability Over Validity: Prioritized getting doctors to agree (Kappa scores) over ensuring the categories were true. Purged psychodynamic causality to create an “atheoretical” common language. |
The Gilded Cage is Built: Saved the profession’s medical legitimacy and enabled the insurance/pharmaceutical industry boom, but amputated meaning and narrative from diagnosis. Created the infrastructure for the 15-minute med check forced by the RUC. |
| DSM-IV (1994) | The Conservative Correction (That Failed) Intended as a stabilization effort to stop reckless expansion, led by Allen Frances with the mantra “no new diagnoses without hard data.” |
Pharmaceutical & Educational Pressures: Massive external incentives from drug companies seeking new markets and school systems needing standardized labels for services overwhelmed the committee’s conservative intentions. | Bureaucratic Inflation: Demonstrated that bureaucratic methodologies are inherently inflationary. Slight loosening of criteria made diagnostic gates porous when faced with external demand from parents, patients, and industry. | The “False Epidemics”: Triggered massive, unexpected explosions in diagnoses for ADHD (teacher reports), Bipolar II (monetizing vague hypomania), and Autism (Asperger’s expansion), which Frances later apologized for. |
| DSM-5 (2013) | The Failed Biological Shift / Fractured Compromise The explicit goal was to move beyond symptoms to biomarkers (genetics, brain scans) to validate disorders as brain diseases. |
NIMH Demands for Science: The National Institute of Mental Health pressured the APA to provide biological proof of their categories after decades of promises. The Failure of Discovery: After 14 years and $25 million, no validating biomarkers were found for any major disorder. |
Moving the Goalposts: Faced with failed field trials showing poor reliability for major disorders like Depression, standards were lowered to ensure publication. Reshuffling the Deck: Remained a symptom checklist manual, failing its primary mandate to become a biological document. |
The “NIMH Divorce”: Two weeks before publication, the NIMH director publicly declared the DSM scientifically invalid (“a dictionary at best”) and shifted research funding to the (not-yet-ready) RDoC framework, splitting research and clinical practice. |
Part III: The Philosophical Critique
Theodore Porter and the Technology of Distrust
Why Soft Sciences Love Numbers
Theodore Porter’s book Trust in Numbers offers maybe the most penetrating analysis of what the DSM actually is.
Porter’s central insight is counterintuitive: rigid rules and quantification are not signs of scientific strength. They’re signs of weakness. The strongest scientists, the ones with the most authority and public trust, don’t need checklists. A physicist doesn’t need a checklist to prove gravity exists. Everyone just believes physicists. They have authority.
Psychiatrists don’t have that authority. They never did. From the beginning, the profession has been looked down upon by “real” doctors, the surgeons and internists who deal with “real” diseases in “real” organs. Psychiatry has always been the soft underbelly of medicine, vulnerable to accusations of being unscientific, subjective, maybe even fraudulent.
When you lack authority, you reach for mechanical objectivity. You create checklists and codes and rigorous-seeming procedures. Not because they reveal truth, but because they protect you from criticism. If someone challenges your diagnosis, you can point to the checklist: “I didn’t make this up. I followed the criteria.” The DSM is a technology of self-defense.
Quantification as Distrust
Porter’s most famous concept is that “quantification is a technology of distrust.” We reach for numbers when we don’t trust the people doing the work.
Think about it. A village doctor who has known his patient for twenty years doesn’t need a checklist. He uses judgment, intuition, relationship. We trust him because of his social position, his track record, his embeddedness in the community.
But the Army can’t trust thousands of random psychiatrists drafted from all over the country. Insurance companies can’t trust the judgment of doctors they’ve never met. Pharmaceutical companies can’t run drug trials if every site uses different diagnostic criteria. These institutions need standardization. They need to remove the judgment from the equation.
The DSM accomplishes this. It turns diagnosis into a bureaucratic procedure that produces the same result regardless of who performs it. It doesn’t matter if you’re a wise clinician or an idiot with a checklist; you’ll get the same diagnosis as long as you count the symptoms correctly.
This is useful for administration. It’s terrible for understanding.
The Genealogy of Authority
Porter’s analysis connects to a deeper pattern that Nietzsche identified: the genealogy of authority.
When institutions lack confidence in their own foundations, they try to ground themselves in something beyond question. Churches trace their authority to divine revelation. Royal families construct genealogies linking them to mythical ancestors. Saddam Hussein famously fabricated a lineage connecting him to the Prophet Muhammad and ancient Babylonian kings.
Psychiatry does the same thing. It tries to ground its authority in “science,” in biology, neuroscience, genetics. It imports the prestige of the hard sciences to cover for its own uncertainty. The checklists are dressed up as “operationalized criteria.” The symptom counts are presented as “scientific measurement.” The whole apparatus is designed to look like medicine.
But here’s Nietzsche’s insight: the intensity of the claim to authority often reveals the depth of the insecurity. The more desperately you insist that your knowledge is objective and scientific, the more you’re revealing that you know it isn’t. A secure discipline doesn’t need to constantly prove itself. An insecure one is always generating data, publishing studies, adding more criteria to the checklist, trying to prove that this time it’s really, truly science.
The Assumption Problem
Here’s the deeper issue that neither the DSM nor its critics want to face: you have to start somewhere. Every science rests on assumptions that can’t be proven within the science itself. Physics assumes that the universe is regular and comprehensible. Biology assumes that living things can be explained mechanistically. Psychology has to assume something about what minds are, how they work, what “health” means.
The DSM’s problem is not that it makes assumptions. It’s that it pretends not to. By claiming to be “atheoretical,” by refusing to say why symptoms cluster the way they do, the manual hides its assumptions rather than examining them.
What are those hidden assumptions? That mental disorders are discrete categories rather than continuous dimensions. That symptoms can be meaningfully separated from the contexts that produce them. That reliability (agreement) matters more than validity (truth). That suffering can be measured without being interpreted. That the individual is the proper unit of analysis rather than the family, the community, or the social system.
Every one of these assumptions is debatable. Many are probably wrong. But because the DSM doesn’t acknowledge them as assumptions, they can’t be examined or revised. They’ve become invisible, the water the fish doesn’t notice.
Porter and Nietzsche would both say: you have to be able to justify your assumptions. You have to say “this is how we think the brain operates” and be willing to defend it. Hiding behind the checklist, generating ever more data to avoid the question, is a form of bad faith. It’s using the appearance of science to avoid doing the work of science.
Soft sciences generate tons of data to legitimize opinions that they don’t have the ability to justify directly. You can’t just say “this is self-evident and we can agree on it.” Even though you have to start with assumptions, even if they’re wrong, you have to start somewhere. But because they don’t want to do that, because they want to seem as certain as physics, they dig deeper and deeper and pretend their assumptions are handed down by God rather than chosen by humans.
It’s not just psychiatry. Churches do this. Royal families do this. Emperors construct elaborate genealogies to make their rule seem inevitable. The pattern is universal. When you can’t justify your authority directly, you try to make it seem like it comes from somewhere beyond question.
But we have to recognize what this really is: fundamental insecurity. The profession needs to pretend that its assumptions are something everyone has to accept rather than justifying why they’re good assumptions. That’s what psychiatry has to learn to do. It has to be able to say: “This is how we think the brain operates. Here’s our reasoning. We might be wrong, but this is our best guess, and here’s why.”
Rebecca Goldstein and the Mattering Problem
What Mental Health Actually Is
Maybe we need to stop and ask a basic question: what is mental health?
The DSM defines disorders but never defines health. It tells you what’s wrong but not what’s right. This is strange. In regular medicine, we know what healthy organs look like. We can describe normal blood pressure, normal heart function, normal kidney filtration. The diagnosis of disease is deviation from a known baseline. In psychiatry, we’ve never established the baseline.
Philosopher Rebecca Goldstein offers a crucial insight here with her concept of the “Mattering Map.” She argues that humans are driven by a need to matter—to feel significant to ourselves and others. We map our lives according to what gives us this sense of significance.
In The Mind-Body Problem, she writes: “The map in fact is a projection of its inhabitants’ perceptions. A person’s location on it is determined by what matters to him, matters overwhelmingly… who are the nobodies and who the somebodies.”
When this map breaks—when a person can no longer find a way to matter, or when the map they have been following leads them into a dead end—we call it “mental illness.” Clinical depression, in Goldstein’s view, is the conviction that “you don’t and will never matter.” It is the collapse of the map.
Resistance to Change as the Core Pathology
If we view mental health through this lens, pathology isn’t just a list of symptoms; it’s a rigidity in the Mattering Map. It’s when a person cannot update their map to match reality.
This reframes everything. Depression isn’t just “five symptoms for two weeks.” It’s a state where the person’s capacity for adaptive change has collapsed. Anxiety isn’t just “excessive worry.” It’s fear blocking the changes the person wants to make to their map. Personality disorders aren’t just clusters of traits. They’re rigid patterns that prevent development.
This is what therapists already know. Anyone who does therapy understands that the work is about facilitating change: helping people update old patterns, release outdated beliefs, become more flexible. The DSM diagnosis is often beside the point. What matters is what’s stuck and what would help it move.
The Patient-Centered Question
And here’s the simplest test, essentially what Albert Ellis asked: Is what you’re doing working for you?
Not “do you meet criteria for a disorder,” but “are your beliefs and behaviors helping you live the life you want?”
If the answer is no, if the person’s patterns are making them miserable, if they’re stuck and can’t move, then maybe they could use some help. It doesn’t matter if we call it a “disorder” or a “problem in living” or just “being human.” What matters is whether they’re suffering and whether we can help.
Part IV: The Shadow Tradition
Joseph Campbell and the Hero’s Journey in a Checklist World
Something remarkable happened in American culture at almost exactly the moment psychiatry was abandoning narrative. A scholar named Joseph Campbell became famous.
Campbell’s book The Hero with a Thousand Faces was published in 1949, but it didn’t become a cultural phenomenon until the 1970s and 1980s. George Lucas explicitly credited Campbell’s work as the template for Star Wars. Bill Moyers’ 1988 PBS series The Power of Myth, filmed shortly before Campbell’s death, reached millions of viewers. Suddenly everyone was talking about the monomyth, the hero’s journey, the call to adventure.
Campbell was drawing on Jung. His concept of the hero’s journey was deeply informed by Jungian archetypes: the shadow, the anima/animus, the wise old man, the threshold guardian. But Campbell made Jung accessible. He stripped away the clinical language and the dense Germanic prose. He talked about Star Wars and fairy tales and ancient myths. He made depth psychology into a story you could understand.
And people were hungry for it.
The Hunger for Meaning
Why did Campbell resonate so powerfully at exactly this historical moment?
Because psychiatry had stopped providing meaning.
The DSM-III revolution stripped the “why” out of diagnosis. It didn’t matter what your symptoms meant or where they came from. All that mattered was whether you met criteria A, B, and C. The human story, the narrative of suffering and growth, was irrelevant to the diagnostic process.
Campbell offered something different. He offered a framework for understanding life as a journey, suffering as initiation, crisis as the call to adventure. In Campbell’s telling, the dark night of the soul wasn’t a disorder to be medicated away. It was a necessary phase of transformation. The dragon you had to face wasn’t a symptom to be eliminated. It was the guardian of the treasure you needed to claim.
This was the opposite of the DSM’s approach. Where the checklist saw pathology, Campbell saw potential. Where psychiatry saw broken brains, Campbell saw heroes in the making.
What Psychiatry Forgot
The appeal of Campbell, and of the Jungian tradition more broadly, was an appeal to story, adventure, progress, and growth. It addressed something that the DSM could not: the question of what life is for.
The checklist model treats mental health as the absence of disorder. If you don’t meet criteria for any diagnosis, you’re healthy. That’s it. There’s no positive vision of flourishing, no account of what a well-lived life might look like, no framework for understanding psychological growth and development.
Campbell offered exactly that. He described psychological development as a journey with recognizable stages: the departure from the ordinary world, the crossing of the threshold, the road of trials, the encounter with the goddess, the atonement with the father, the apotheosis, the return. This gave people a map. It told them where they were and where they might be going.
Psychiatry had once offered something similar. The psychodynamic tradition had a developmental theory. It understood psychological growth as a process of integration, of coming to terms with unconscious material, of expanding the ego’s capacity to tolerate reality. This wasn’t just about fixing symptoms; it was about becoming more fully human.
The DSM threw all that away. And the public went elsewhere to find it.

The Shadow Tradition: Experiential Therapy Takes Root
This cultural wave of narrative and meaning didn’t just stay in Hollywood. It seeped into the practice of therapy, creating a “Shadow Tradition” of somatic and experiential models that flourished outside the academic mainstream.
While the DSM was flattening patients into checklists, therapists were discovering that healing often required somatic experiencing and parts work. The concepts of Jung and Campbell became the unacknowledged DNA of models like:
- Internal Family Systems (IFS): Richard Schwartz’s model of “parts” (Managers, Firefighters, Exiles) is essentially a systematic way of doing inner child work and shadow integration. It treats the psyche as a multiplicity of characters, much like a mythic story, rather than a singular broken machine.
- Gestalt Therapy: Fritz Perls focused on the “here and now” experience and the integration of fragmented parts of the self. The “empty chair” technique is a way of dialoguing with internal archetypes.
- AEDP (Accelerated Experiential Dynamic Psychotherapy): Diana Fosha’s model explicitly uses the concept of “transformance”—a drive toward healing and growth that mirrors Campbell’s heroic drive—to undo aloneness and process emotion.
These models are now exploding in popularity because they work. They speak to the human need for narrative and integration that the DSM ignores. They treat the patient as a protagonist in a meaningful struggle, not a carrier of a diagnostic code.
Jung, Joyce, and the Diving-Drowning Problem
There’s a famous case that illustrates the complexity of mental illness beautifully: Carl Jung’s treatment of Lucia Joyce, the daughter of James Joyce.
In the 1930s, Jung treated Lucia for what was then called schizophrenia. She was the daughter of one of the twentieth century’s most celebrated literary modernists, a man whose work (Ulysses, Finnegans Wake) deliberately plunged into the depths of the unconscious mind. Joyce’s writing was a controlled descent into chaos, a systematic exploration of stream-of-consciousness, dream logic, and linguistic fragmentation.
Jung saw something troubling in the parallel between father and daughter. He famously described them as two people heading to the bottom of a river, except that Joyce was diving while Lucia was drowning. Joyce could access the unconscious voluntarily, for his art, and return. Lucia was pulled under involuntarily and couldn’t find her way back.
This image of the diver versus the drowning person became one of the most powerful ways that Jungian conceptualization entered non-Jungian audiences. Joseph Campbell, who did more than anyone to popularize Jung’s ideas for the general public, drew heavily on this distinction. When Campbell talked about the hero’s journey into the underworld, about the descent into darkness that precedes transformation, he was drawing on Jung’s understanding that some people can navigate the unconscious and return while others get lost there. The artist as controlled diver, the psychotic as uncontrolled drowning victim: this formulation almost certainly has its roots in Jung’s work with the Joyce family, even when Campbell didn’t cite it directly.
Jung’s interpretation was that Joyce, as an untethered modernist and bohemian, had never taught his daughter how to handle the unconscious. Joyce retreated into those depths of the unconscious on a whim for his work, but he had the capacity for return; his daughter lacked that capacity. Jung was probably sensing, subjectively, that part of Lucia’s condition was hereditary (she may have shared some of her father’s unusual relationship to primary process thinking) and part was environmental (her father’s inability to structure his own life or model psychological groundedness). Joyce approached the unconscious like a psychonaut; Lucia needed a guide, and her father couldn’t be one because he was exploring the same territory without a map.
Was Jung right? We can’t know for certain. His interpretation was subjective, based on clinical intuition rather than data. The psychoanalytic method, for all its depth, couldn’t distinguish between what Lucia inherited biologically and what she learned environmentally. Jung could feel that both factors were present, but he couldn’t prove it or quantify it.
The Populist Revolt and Its Limits
Van der Kolk and Maté: The Therapists the Establishment Laughs At
Here’s a strange phenomenon: the mental health professionals with the biggest public followings are often the ones the academic establishment dismisses.
Bessel van der Kolk wrote The Body Keeps the Score, which has sold millions of copies and shaped how a generation thinks about trauma. Gabor Maté, with In the Realm of Hungry Ghosts and The Myth of Normal, has become a global figure whose talks fill auditoriums. These are serious clinicians with decades of experience and, in van der Kolk’s case, substantial research credentials.
But within academic psychiatry, they’re often treated as popularizers at best, cranks at worst. Van der Kolk’s push to include Developmental Trauma Disorder in DSM-5 was rejected. Maté’s emphasis on childhood adversity and the role of environment in addiction doesn’t fit the brain-disease model that dominates research funding.
Why does the public love them while the establishment dismisses them? Because they’re talking about meaning. They’re asking what happened to you, not just what’s wrong with you. They’re connecting symptoms to stories, suffering to context, disorder to the lived experience of being human in a difficult world.
This is what the DSM stripped away and what RDoC ignores entirely. The public hunger for Van der Kolk and Maté is a hunger for the meaning that the official system refuses to provide.
The Limits of Populism
But here’s the problem: you can’t fix psychiatry through bestsellers.
Van der Kolk can convince millions of readers that trauma matters. He can’t rewrite the diagnostic criteria. He can’t change how insurance reimburses. He can’t restructure medical education or residency training. He’s operating outside the system that actually shapes practice.
There’s a fantasy in some circles that if enough people read the right books, listen to the right podcasts, understand the critique, then change will somehow happen. But institutional change doesn’t work that way. The DSM isn’t going to be revised by public pressure. It’s going to be revised by the APA’s Task Force, by the committees and workgroups, by the same professional structures that created the current mess.
The public can’t vote on the DSM-6. The reform has to come from inside. And the insiders are increasingly disconnected from the critics.
The Critical Mass Problem
As more and more people insecurely cleave to the system, as more careers depend on the current categories, as more infrastructure gets built around existing diagnoses, it becomes harder and harder for there to be a critical mass within mainstream psychology that’s able to fix it.
This is a huge problem. You can’t have a bunch of people listen to a podcast and then write their own manual. That’s not going to happen. You can’t read a bunch of critiques and then have the public vote on the DSM-6. You have to have critical mass within the academic body.
And the academic body is splitting from clinical practice. The researchers are doing one thing; the practitioners are doing another; the public is reading a third thing; and nobody’s talking to each other. This is terrifying because it means the system might just keep grinding along, getting worse, until some external shock forces change.
Part V: The Gilded Cage
The RUC: The Cartel in the Basement
While Spitzer was having his typewriter parties, a much quieter, deadlier revolution was happening in the basement of American medicine. This revolution wasn’t about philosophy or diagnosis. It was about money. And unlike the DSM, which was public and controversial, this revolution happened in a room almost nobody knew existed.
It’s called the RUC: The AMA/Specialty Society Relative Value Scale Update Committee. If you’ve never heard of it, that’s by design. It is a private committee run by the American Medical Association that essentially tells the federal government how much Medicare should pay for every medical procedure. Because private insurance companies almost universally follow Medicare’s lead, this committee effectively sets the price for all healthcare in America. If therapists did this it would be illegal but because the RUC is just advising—making a recommendation that is accepted 90% of the time—the RUC is not considered a cartel legally. Many argue that it actually functions as one.
The RUC is exempt from the laws that would normally prevent this kind of behavior. In any other industry, if a group of competitors (surgeons, cardiologists, psychiatrists) got together in a room to decide what to charge for their services, the Department of Justice would arrest them for price-fixing. It’s a violation of the Sherman Antitrust Act. But the RUC operates under a unique regulatory shelter that allows it to function as a legal cartel.
The Chilling Effect: Procedures Over People
The RUC is dominated by specialists who perform procedures—surgeons, radiologists, anesthesiologists. Their bias is structural and overwhelming: they value “doing things to people” (cutting, scanning, injecting) far more highly than “talking to people” (diagnosing, counseling, managing complex chronic conditions).
In the late 1980s and early 90s, when the Resource-Based Relative Value Scale (RBRVS) was being implemented, psychiatry had to fight for its slice of the pie. The pie is fixed—Medicare is a zero-sum game. If you pay surgeons more, you have to pay someone else less.
Remember too that it was at this point that schizophrenia was vanishing when people were being given antipsychotics and so the assumption was that eventually psychiatry could retreat into materialism and that a pill would solve everything. We now know that that isn’t true. There are neurobiological conditions, there are genetic conditions, there are conditions that respond better to medication, there are conditions that respond better to therapy, and there are systems that affect people. Not all of this can or should be medicated.
The psychiatric representatives on the RUC made a fateful, perhaps desperate, calculation. They realized they couldn’t compete with the proceduralists if they emphasized talk therapy. Talk therapy looks “easy” to a surgeon. It’s “just talking.” It doesn’t use expensive machines. It doesn’t involve blood. Modern analysis of competence in the industry proved that this is not true and the lack of pay means that people who could do therapy probably don’t learn to do it well. They do something else that would pay the bills. If therapy was revalued as a profession and held to a higher standard with more comprehensive training that does include the things that I’m advocating for here, then it would become valuable. But in order to become valuable, therapy has to become effective again.
Because of assumptions in the 1970s, psychiatry pivoted. They emphasized the one thing they could do that psychologists and social workers couldn’t: prescribe medication. They argued that “medication management” was a complex, high-risk medical procedure requiring the specialized knowledge of a physician. They devalued their own therapeutic work to inflate the value of their prescribing work.
The Economic Straitjacket
The result was catastrophic for the soul of the profession. The RUC assigned high relative value units (RVUs) to brief medication checks (CPT code 99213 or 99214) and comparatively low values to the psychotherapy codes.
The math became brutal. A psychiatrist could see three or four patients (or more in practice) in an hour for medication checks, billing significantly more in total than they could for seeing one patient for an hour of therapy.
This created a chilling effect that froze the entire profession. Even psychiatrists who wanted to do therapy—who believed in it, who were trained in it—couldn’t afford to. They were facing medical school debt, high malpractice premiums, and the rising costs of running a practice. The “invisible hand” of the RUC pushed them inexorably toward the 15-minute med check.
This is why the “checklist” model of the DSM became not just an intellectual preference but an economic survival strategy. If you only have 15 minutes with a patient, you cannot do a dynamic formulation. You cannot explore the subtle interplay of their childhood and their current crisis. You can only do what the time allows: run down a list of symptoms, check the boxes, and write a prescription. The DSM provided the perfect administrative tool for the assembly-line medicine the RUC demanded.
The “Illegal” Legal Mechanism
The most disturbing part of this system is that it functions exactly like the “restraint of trade” tactics that antitrust laws were meant to abolish. It prevents competition. It prevents innovation. It ties the hands of everyone in the system.
If a group of innovative psychiatrists wanted to start a practice based on a different model—say, deep, slow, relational work—they are structurally penalized. They can’t just charge what the market will bear because the insurance system is rigged to the RUC’s price sheet. They can’t get reimbursed for the actual value of the time they spend.
This regulatory environment creates a monoculture. It forces everyone to practice the same way, regardless of their theoretical orientation. The psychiatrist who hates the DSM and loves Freud still has to use the DSM codes and still has to see four patients an hour, because the RUC has decided that’s what a psychiatrist is worth.
It acts as a barrier to entry for any methodology that doesn’t fit the “medicate-and-move-on” model. It effectively outlaws the practice of relationship-based psychiatry for anyone who isn’t wealthy enough to operate entirely outside the insurance system (cash-pay concierge medicine).
So when we ask “Is the DSM dying?”, we have to ask: “Is the RUC dying?” Because as long as the economic engine of American medicine pays for checklists and pills but starves relationships and meaning, the DSM will survive. It is the perfect accounting ledger for a system that values efficiency over healing.
The Divorce of Psychiatry and Therapy
They Used to Share the Same Room
Here’s something that gets overlooked in every analysis of the DSM: psychiatrists don’t do therapy anymore.
Read Irvin Yalom, the gateway drug that brought many people into the profession, and you’ll find a psychiatrist who spent hours with patients exploring their fears, their histories, their dreams. He was the prescriber and the therapist in the same relationship. He knew his patients deeply before he ever wrote a prescription.
Try to find a psychiatrist like that today. If you find one, they’re either independently wealthy or pushing 80. The economics of the profession make it impossible. Insurance reimbursement for a 15-minute medication check vastly exceeds the hourly rate for therapy when adjusted for time. A psychiatrist who does therapy is leaving money on the table.
So psychiatry split. The prescribing authority stayed with psychiatrists. The therapeutic relationship went to psychologists, social workers, counselors. The person who knows you deeply is not the person who controls your medication.
This matters more than people realize. When you separate diagnosis from relationship, you get checklist diagnosis. Of course you do. The psychiatrist doesn’t have time to understand your life. They have 15 minutes to count your symptoms and adjust your meds. The DSM is perfectly designed for this assembly-line model of care. It’s a tool for people who don’t know their patients.
The Split Between Research and Practice
This institutional divorce, between psychiatry and therapy, between prescribers and relationship-builders, maps onto the NIMH divorce. There’s now a split between the people who study mental illness and the people who treat it.
Researchers use RDoC. They study circuits and genes and neuroimaging. They’re trying to carve nature at the joints, to discover the biological foundations of suffering. I don’t think that there is a ghost in the machine to be found there because the ghost inhabits our brains, our bodies, our brainstem, and our gut. The body is not just a go-kart that carries the brain around; it is a process that is embodied in psychology itself.
Clinicians use DSM-5. They have no choice. It’s the only system that works for billing, for communication, for treatment planning. They know it’s flawed, but they need to get through the day.
The academic body and clinical practice are drifting apart. And this is terrifying, because change has to come from inside the academic body. You can’t read a bunch of podcasts and write your own DSM-6. You can’t have the public vote on diagnostic criteria. Reform requires critical mass within the profession.
But as the people who actually treat patients become disconnected from the people who do research, that critical mass becomes harder to achieve. The researchers are off studying brain circuits, producing knowledge that can’t be used in the clinic. The clinicians are drowning in paperwork and patient volumes, with no time to contribute to reform.
The insecurity Porter identified, the need to prove that psychiatry is “real” science, drives the profession further into biology and further away from the therapeutic encounter where healing actually happens.
Part VI: Alternatives and Futures
Why HiTOP Would Be Better (And Why Nobody Wants It)
The Scientific Ideal: Factor Analysis
Remember the method Spitzer should have used but couldn’t? Gather all the symptoms, use statistics to see which cluster together, and let the data tell you where the categories are?
That’s what HiTOP does.
The Hierarchical Taxonomy of Psychopathology (HiTOP) is built entirely from factor analysis. Researchers collected data on symptom correlations across massive populations. They ignored the historical DSM boundaries and just looked at how symptoms naturally cluster.
What they found is elegant. At the top level, there’s something called the “p-factor,” a general factor of psychopathology, like the “g-factor” in intelligence research. Some people are just more vulnerable to mental health problems in general, regardless of which specific form those problems take.
Below that are broad spectra: Internalizing (anxiety, depression, and related conditions), Externalizing (antisocial behavior, substance use), Thought Disorder (psychosis and related phenomena). These spectra capture the real statistical structure of mental suffering.
HiTOP explains comorbidity, the annoying fact that DSM patients almost always qualify for multiple diagnoses. In HiTOP, comorbidity isn’t a puzzle; it’s expected. A patient with “depression” and “anxiety” and “panic disorder” isn’t suffering from three diseases. They’re just high on the Internalizing spectrum. The different DSM labels were artificial boundaries carved into a continuous dimension.
Why the NIMH Doesn’t Use It
You’d think the NIMH would love HiTOP. It’s empirically derived. It solves the comorbidity problem. It maps better onto what we know about genetics and neural circuits.
But HiTOP still has the same fundamental flaw as the DSM: it’s based on symptoms. It tells you which symptoms cluster together, but it doesn’t tell you why. It doesn’t give you biomarkers. It doesn’t carve nature at the joints.
Insel and the NIMH wanted to skip symptoms entirely and go straight to biology. They didn’t want a better map of how people describe their suffering; they wanted a map of what’s happening in the brain. RDoC was their attempt to build that biological foundation from scratch.
The irony is that RDoC might never be clinically useful. It’s been over a decade since Insel’s announcement, and we still can’t diagnose anyone using brain circuits. Meanwhile, HiTOP offers a genuinely superior symptom-based system that could be implemented tomorrow. But nobody’s implementing it.
What HiTOP Could Actually Give Us
Here’s what nobody talks about: if we actually applied HiTOP systematically, we could finally get real data about the questions that have haunted psychiatry since its inception.
We could track how these disorders actually show up over time. We could examine, with genuine longitudinal data, how much of these conditions is genetic and how much is learned, how much is environmental. We could finally start to untangle the nature versus nurture knot that has made psychiatric research so frustrating.
Part of nature versus nurture will always remain a mystery. That’s just the reality of complex systems. But one of the deepest problems with current diagnoses is that they point at something that’s almost always both: a predisposition (nature) and an environmental trigger or reward (nurture) that sit on top of each other. And here’s the kicker: the genetic predisposition and the environmental trigger are often found in the same environment, because families share both genes and environments. A child inherits their parent’s neurobiology AND grows up in the household that parent creates. Trying to separate these is enormously difficult.
This is why you can’t just define the biology of every diagnosis and call it a day. The biology and the environment are confounded. They’re wrapped around each other. A child with a genetic loading for anxiety grows up with an anxious parent who models anxious behavior and creates an anxious household. Which part is the genes? Which part is the learning? The honest answer is: we don’t know, and maybe we can’t fully know, but we could know a lot more than we do now.
This is exactly where HiTOP could help. If we had dimensional data on psychosis-proneness across generations, correlated with family environments and parenting styles and creative professions and substance use, we could start to make finer judgments about these correlations. We could bring science to the questions that analysis could only address through intuition.
DSM vs HiTOP Comparison Table
| Feature/Aspect | DSM-5 (The “Flat” Categorical Model) | HiTOP (The Hierarchical Dimensional Model) |
| Fundamental Paradigm | Categorical & Binary: Mental disorders are treated as distinct “yes/no” entities, similar to medical diseases (e.g., you either have pneumonia or you don’t). | Dimensional & Spectrum-Based: Psychopathology exists on continuous dimensions ranging from normal to severe. There are no hard cut-offs between “health” and “disorder.” |
| Structural Architecture | The “Flat List”: A non-hierarchical catalog of hundreds of separate disorders, largely treated as parallel distinct categories (e.g., Major Depression is a separate box from Generalized Anxiety). | The Hierarchy: A multi-layered pyramid structure. At the top is general psychopathology (the “p-factor”). Below are broad spectra (e.g., Internalizing), subdividing into narrower syndromes and specific symptoms. |
| Method of Development | “Backwards” / Top-Down (Consensus): Committees started with pre-existing diagnostic labels (legacy concepts like “Schizophrenia”) and used political negotiation and voting (“typewriter parties”) to agree on symptom lists to define them. | “Forwards” / Bottom-Up (Empirical): Derived from analyzing massive datasets of symptom observations using statistical methods (factor analysis) to see how symptoms naturally cluster together in reality, ignoring prior labels. |
| Handling Comorbidity | The “Comorbidity Problem”: High rates of patients meeting criteria for multiple disorders (e.g., anxiety + depression) is viewed as a puzzling bug in the system, suggesting the patient has multiple distinct “diseases.” | Comorbidity as a Feature: “Comorbidity” is expected. Overlapping symptoms just mean the patient scores high on a broad underlying spectrum. Anxiety and depression often occur together because they are both facets of the “Internalizing” spectrum. |
| Scientific Validity | Low Validity (“Bucket of Sludge”): The categories rarely map cleanly onto underlying biology, genetics, or treatment response. Research fails because it studies heterogeneous groups lumped under one label. | Higher Validity: The empirically derived spectra align much better with emerging data on genetic vulnerabilities, neural circuitry dysfunction, and environmental risk factors. |
| Key Goal During Creation | Reliability (Agreement): The primary goal, especially since DSM-III, was ensuring different doctors gave the same diagnosis for the same patient, prioritizing standardized checklists over deeper understanding. | Validity (Truth): The primary goal is to create a map that accurately reflects the statistical reality of how human suffering is organized in nature. |
| Current Status & Utility | Administrative Dominance: It is the mandatory standard for insurance billing, legal proceedings, and clinical communication in the US, despite NIMH rejecting it for research. | Research Dominance / Clinical Irrelevance: It is preferred by many cutting-edge researchers (and aligns better with NIMH goals), but currently unusable for practical clinical billing or standard treatment guidelines. |
The Flattening Problem
One of the most profound failures of the checklist model is its “flattening” effect. The DSM treats all diagnoses as fundamentally the same kind of thing—a collection of symptoms that, if present, equal a disorder.
But clinicians know that some things are not like the others. Specifically, the “dopamine disorders”—Schizophrenia, Bipolar I, and Schizoaffective Disorder—share a biological reality that is fundamentally different from a personality disorder or a situational depression.
We know these disorders share similar neurological routes. We know they respond consistently to the same classes of medication (antipsychotics and mood stabilizers). And perhaps most importantly, we know that therapists have a hard time telling them apart.
When a patient is in the throes of a manic episode with psychotic features, they look remarkably like a patient with schizoaffective disorder. A patient with schizophrenia who has prominent mood symptoms blurs into bipolar territory. The DSM forces us to draw sharp lines between these conditions—you are either Bipolar OR Schizophrenic—but clinical reality is fuzzy.
This fuzziness is a signal. The fact that patients have a hard time understanding the difference, and therapists have a hard time telling them apart, should tell us something: these are likely expressions of the same underlying biological vulnerability. They are variations on a theme, not separate species.
By “flattening” these biologically robust conditions into the same checklist format as “Adjustment Disorder” or “Narcissistic Personality Disorder,” the DSM obscures the reality of both. It makes the biological conditions seem less biological (just another checklist) and the psychological conditions seem more biological (implies a disease process where there may be none).
A Different Architecture: The Layered Model
The Problem with the Flat List
The DSM treats all diagnoses as basically the same kind of thing. Depression, schizophrenia, autism, borderline personality disorder, PTSD: they’re all “mental disorders” listed in the same manual with the same checklist structure. Some are in one chapter, some in another, but they’re fundamentally parallel categories.
But this is obviously wrong. These are not the same kind of thing.
Some conditions have clear biomarkers. Neurodevelopmental disorders like intellectual disability have measurable cognitive differences. Some dopamine disorders respond so consistently to the same medications that there’s obviously a biological process involved, even if we don’t fully understand it. When you give lithium to a bipolar patient and their mood stabilizes, when you give an antipsychotic to someone with schizophrenia and the voices quiet down, something biological is happening.
Other conditions have no biomarkers and don’t respond consistently to medication. Depression is the obvious example. We’ve spent fifty years trying to find the biology of depression and mostly failed. The medications help some people sometimes, but response rates are poor and we can’t predict who will benefit. Maybe “depression” isn’t a biological category. Maybe it’s a heterogeneous collection of problems that share surface symptoms but have different causes.
Still other things in the DSM aren’t really about the individual at all. They’re about relationships, systems, environments. The “V-codes” at the back of the manual, relational problems, bereavement, abuse, are shoved into a ghetto precisely because they don’t fit the individual-pathology model. But they’re often what’s actually causing the suffering.
A Layered Model
What would a better architecture look like? Maybe something like this:
Layer 1: Neurodevelopmental conditions. Things we have biomarkers for, that are present from early life, that don’t fundamentally change. Intellectual disability. Autism (at the more severe end). These aren’t diseases that come and go; they’re differences in how the brain is structured.
Layer 2: Genetic/endogenous conditions. Things that are probably biological, that respond consistently to medication, that run in families. The dopamine disorders: schizophrenia, bipolar. We may not fully understand the mechanism, but we have external markers. Every time they take lithium they stabilize. Every time they take antipsychotics the psychosis remits. Something biological is happening.
Layer 3: Dysregulation conditions. Things that used to be the core of psychiatric diagnosis: what we now call depression, anxiety, PTSD. Here the system is out of whack, but we don’t know if the cause is biological, psychological, or social. Maybe it’s trauma. Maybe it’s a genetic vulnerability. Maybe it’s both. The key insight is that these conditions often respond to non-biological treatment. Therapy works. Sometimes it works better than medication. The disorder isn’t a brain disease; it’s a pattern of dysregulation that can be changed.
Layer 4: Characterological conditions. Things that aren’t primarily symptom-based but are about the person’s patterns of living. Personality disorders. Avoidance. Rigidity. Places where people deflect from change or avoid big parts of life. This isn’t about their brain chemistry; it’s about their assumptions, their habits, their learned responses. These are what therapists work with every day: the personality and the negative self-understanding and the lack of insight.
Layer 5: Systemic conditions. Things that aren’t in the person at all, but in their relationships and environment. Enmeshed family systems. Parental alienation. Effects of racism, poverty, discrimination. The DSM keeps wanting to pathologize these, but they’re not individual pathology. They’re about how systems affect people.
The Advantage of Layers
This layered approach lets you ask better questions. When someone comes in suffering, you ask: what layer is this primarily about?
If it’s Layer 2, if we’re dealing with schizophrenia, then medication is probably primary and therapy is support. If it’s Layer 3, dysregulation, then therapy might be the main treatment, with medication as adjunct. If it’s Layer 4, characterological, you’re looking at long-term personality work that drugs won’t touch. If it’s Layer 5, systemic, you might need family therapy, social intervention, or policy change, not individual treatment at all.
The current DSM can’t make these distinctions. Everything’s a disorder. Everything gets the same checklist. The nuance about what kind of problem this is, and therefore what kind of response makes sense, is lost.
Layered Model Table
| Layer & Title | Nature & Underlying Mechanism | Expanded Examples | Key Evidence & Scientific Basis | Treatment Implications |
| Layer 1: Neurodevelopmental Conditions | Nature: Fundamental, early-onset deviations in brain architecture and neural connectivity development. These are typically static or slow-changing, representing a neurodivergent baseline rather than an acquired disease state.
Mechanism: Disruptions in neurogenesis, neuronal migration, or synaptic pruning during critical fetal/infant developmental periods. |
• Intellectual Disability (various severities) • Autism Spectrum Disorder (especially Level 2/3) • Specific Learning Disorders (dyslexia, dyscalculia) • Rett Syndrome • Severe ADHD presentations |
Measurable Markers: • Genetic: Identifiable chromosomal abnormalities (e.g., Trisomy 21 in Down Syndrome, FMR1 mutation in Fragile X). • Neuroimaging: Structural MRI often reveals atypical brain volume or connectivity patterns (e.g., fusiform gyrus underactivation in autism facial recognition tasks). • Standardized Testing: Cognitive testing consistently showing IQ scores two standard deviations below mean (for ID). |
• Habilitation vs. Rehabilitation: Focus is on skill-building, accommodation, and support services rather than “cure.” • Early intervention therapies (speech, occupational, behavioral) are paramount to maximize developmental potential. |
| Layer 2: Genetic/Endogenous (“Dopamine Disorders”) | Nature: Strong biological, often hereditary underpinnings distinct from standard emotional dysregulation. These conditions are characterized by episodic deviations from baseline reality testing or mood stability.
Mechanism: Often linked to dysregulation in specific neurotransmitter pathways, most notably dopamine (e.g., excessive D2 receptor transmission in mesolimbic pathways linked to psychosis) and glutamate. |
• Schizophrenia Spectrum Disorders • Bipolar I Disorder • Schizoaffective Disorder • Major Depressive Disorder with Psychotic Features |
Biological & Clinical Convergence: • Heritability: High heritability rates in twin studies (~80% for schizophrenia and Bipolar I). • GWAS Data: Genome-wide association studies identify shared genetic risk loci across these disorders (e.g., CACNA1C gene). • Pharmacological Response: Consistent response to dopamine antagonists (antipsychotics) and mood stabilizers (lithium/anticonvulsants) for acute stabilization. • Clinical Overlap: High difficulty for clinicians distinguishing acute manic psychosis from schizoaffective states due to shared phenomenology. |
• Pharmacology is Primary: Medication is usually essential for stabilization and relapse prevention. • Psychosocial Adjuncts: Therapy focuses on medication adherence, insight, social rhythm therapy, and managing the functional fallout of episodes. |
| Layer 3: Dysregulation Conditions | Nature: The body’s stress-response and affect-regulation systems are chronically imbalanced due to a complex interplay of genetic vulnerability, past trauma, and current environmental stressors.
Mechanism: Dysregulation of the HPA (hypothalamic-pituitary-adrenal) axis leading to chronic cortisol elevations; amygdala hyperreactivity (fear center); reduced hippocampal volume (memory/context processing) due to chronic stress toxicity. |
• Major Depressive Disorder (non-psychotic) • Generalized Anxiety Disorder • Post-Traumatic Stress Disorder (PTSD) • Obsessive-Compulsive Disorder (OCD) • Panic Disorder |
Biopsychosocial Evidence: • Stress Biomarkers: Elevated inflammatory markers (e.g., C-reactive protein) and atypical cortisol awakening responses often found in chronic depression/PTSD. • Neuroplasticity Research: fMRI studies show that psychotherapy (like CBT or EMDR) can normalize activation in the amygdala and prefrontal cortex, demonstrating top-down neural retraining. • Epigenetics: Evidence that environmental trauma can alter gene expression related to stress response without changing DNA sequence. |
• Therapy is Primary/Equal: Psychotherapy is often the first-line treatment of choice. • Medications (SSRIs/SNRIs) act as scaffolds to lower symptom intensity enough for therapeutic work to occur, but may not address the root cause of the dysregulation. |
| Layer 4: Characterological Conditions | Nature: Rigid, pervasive patterns of perceiving, relating, and thinking that become engrained over time. These are learned maladaptive coping mechanisms that have solidified into a “personality structure.”
Mechanism: Formed through an interaction of innate temperament (e.g., high neuroticism) and early developmental environments (e.g., insecure attachment, invalidating environments), leading to fixed maladaptive schemas (core beliefs about self/world). |
• Borderline Personality Disorder (also has Layer 3 features) • Narcissistic Personality Disorder • Avoidant Personality Disorder • Obsessive-Compulsive Personality Disorder (distinct from OCD) • Chronic interpersonal difficulties |
Psychological & Developmental Evidence: • Attachment Studies: Strong correlations between disorganized or insecure early attachment styles and adult personality pathology. • Schema Research: Identification of specific, enduring negative core beliefs (e.g., “I am defective,” “People are untrustworthy”) driving behaviors across varying situations. • Medication Non-Response: Psychiatric medications rarely ameliorate core personality traits (e.g., emptiness, fear of abandonment, grandiosity). |
• Long-Term Psychotherapy: Treatment requires long-term, relational, or insight-oriented therapy (e.g., Dialectical Behavior Therapy, Schema Therapy, Psychodynamic therapy). • Goal is restructuring deeply held beliefs and developing new relational patterns, rather than symptom reduction. |
| Layer 5: Systemic Conditions | Nature: The primary driver of distress is located in the external environment, social structures, or immediate relational systems, rather than individual internal pathology.
Mechanism: “Allostatic load”—the cumulative wear and tear on the body and brain resulting from chronic exposure to fluctuating or heightened neural or neuroendocrine responses resulting from environmental challenges. |
• Chronic Poverty/Financial Stress • Systemic Racism and Discrimination • Domestic Violence/Abuse dynamics • Enmeshed or High-Conflict Family Systems • Adverse Childhood Experiences (ACEs) • Housing/Food Insecurity |
Sociological & Epidemiological Evidence: • Social Determinants of Health (SDOH): Massive data sets confirm that zip code, economic status, and systemic marginalization are stronger predictors of health outcomes than many biological factors. • ACE Study: Strong dose-response relationship between the number of Adverse Childhood Experiences and adult mental/physical health outcomes. • V-Codes: The DSM acknowledges these as “Other Conditions That May Be a Focus of Clinical Attention,” indicating they are external to psychiatric disorders yet clinically relevant. |
• Non-Clinical Interventions: Primary interventions are often social work, policy change, community organizing, legal aid, or family systems therapy. • Individual therapy focuses on coping with an unchangeable environment or empowering the individual to navigate/escape the systemic stressor. |
The Coming Crisis
The Ticking Clock
The system is unstable. It can’t hold. Younger generations are laughing at you and demanding a new therapy. They aren’t doing it because they know this history; they are doing it because they know that the current system is not working for them. The further we have followed the evidence basis in the direction that the DSM Committee interprets it, the more we have seen psychotherapy outcomes get worse.
We have a diagnostic manual that the government’s own research agency says is scientifically invalid. We have a profession split between clinicians using one paradigm and researchers using another. We have insurance companies demanding categorical diagnoses for a reality that’s dimensional. We have an epidemic of mental health problems and a workforce that can’t meet the demand.
Something will break. The question is when and how.
Porter would say that the transition will probably come during a recession, when the economic pressure on healthcare systems becomes unbearable, when someone decides we can’t afford to keep doing things the inefficient old way. That’s often when bureaucratic revolutions happen. Crisis creates the opening for change.
The danger is that whoever is positioned when that moment comes will get to design the replacement. And right now, the people positioned are not the therapists or the patients. They’re the technology companies, the pharmaceutical giants, the insurance bureaucracies. If we’re not careful, the next diagnostic system will be designed to serve their interests, not the interests of human flourishing.
Conclusion: The Synthesis We’re Waiting For
Let me try to summarize where we are.
Part of this critique is not that many of the modern assumptions about the way we diagnose are wrong. The problem as I see it is that the modern neuroscience and clinical observations we have are being held at bay by outdated unconscious and implicit assumptions baked into the context of how the system was created and still present in the DSM-5. Stripped of conceptualizations that let psychology acknowledge and study an unconscious or implicit reactions in the therapy room, the macro system itself is not able to analyze the unconscious and implicit biases that are not evidence-based baked into its own system. Academic training largely strips this broader context out of what it teaches. Therapists and mental health professionals are taught that whatever is evidence-based or considered evidence-based at the time they are in graduate school is just the way it always will be and the way that it always should have been. We don’t learn how to analyze systems or see if they change.
We don’t learn the history and the debates within the profession. This means that we’re not able to diagnose the point in the history of science that we’re in while we learn about diagnosis, and these are all wild ironies. This explains why so many therapists continue doing what happened when they were in graduate school even if that was 1980 and don’t continue to self-educate. Continuing education is supposed to stymie this problem but it often just repeats whatever the current conception is and doesn’t look for these biases or analyze these systems. Look at how we got here. Should we still be doing things that we were doing in the 1950s? Look at the history of a diagnosis like borderline personality disorder which is essentially three conceptualizations that contradict grafted together. The three conceptualizations contradict but no one remembers the tension between them because no one remembers the history.
It is easy to sit back and blame psychopharm companies. That’s not wrong; major pharmaceutical companies have admitted at board meetings by this point that they would rather treat to treat than treat to cure because cures are not profitable. The profit motive in healthcare is definitely an incentive structure that should be kept at bay with regulations because it is not in and of itself scientific and is in many places at odds with science. However, these arguments do not go to the root of the system and they fail to understand it. In my experience it is not just these, granted nefarious forces, that cause the problems in the modern DSM.
The real root of the problem is the academic insecurity of professionals like Theodore Porter and Nietzsche diagnosed. Academics are taught to defend systems; research psychologists live solely within them. When we put garbage into these systems we get garbage out of them. Even looking at the same data the wrong way can lead you to the wrong story. The psychiatry and psychological establishment need to step back and admit that they don’t know everything because we don’t know everything yet. We need to adjust our assumptions to fit the data, not the data to fit our assumptions, and we need to do that yesterday. How little the public pays attention to these things is part of the reason why we’re in the state we’re in. It should have been national news that you had the largest scientific body saying that the DSM was no longer scientific. In my experience not even therapists know about that.
The DSM was never a description of nature. It was a set of administrative protocols created by the military, adapted by the bureaucracy, defended by a profession fighting for legitimacy, and captured by industries seeking profit. It achieved reliability by sacrificing validity. It made doctors agree on labels while ignoring the question of whether the labels meant anything.
The NIMH’s RDoC is an honest acknowledgment that the labels don’t work for science. But it’s also a retreat into pure materialism: a decision to study the machine while ignoring the ghost. It has no place for meaning, for narrative, for the human experience of suffering. It’s great for neuroscientists; it’s useless for therapists.
We’re left with a split. The DSM is a map of human stories that has no biological grounding. RDoC is a biological map that has no human stories. Neither one, alone, can guide treatment.
What would a synthesis look like? Maybe something like the layered model I sketched: different frameworks for different kinds of problems, with the biological at the bottom, the psychological in the middle, and the systemic at the top. Maybe something that starts from a definition of health—like Goldstein’s ability to matter—rather than just cataloging pathology.
Checklists could work in this synthesis. But they’d have to work forward, not backward. They’d have to start with observations and let categories emerge, rather than starting with categories and forcing observations to fit. They’d have to be tools for organizing knowledge, not substitutes for it.
Nietzsche would say: admit your assumptions. You cannot create a completely logical system as an emotional being that does not know its own blind spots. Stop pretending the DSM fell from evidence-based practice heaven. It was a product of history and the blind spots of history in the systems and bureaucracies that still run our world. If you don’t see it as such you aren’t being a scientific being you are being a child, incapable of handling the uncertainty that it takes to be an adult. Stop acting like the categories are carved in nature. Say “this is how we currently think the brain operates” and be willing to defend it and change it when it stops working.
Science isn’t a story we tell once and then repeat forever. It’s a process of telling better and better stories, of revising our maps when they stop matching the territory. The DSM has become a story that can’t be revised: a sacred text defended by institutions whose survival depends on it being true.
The story will change. It always does. The only question is whether we’ll change it carefully, thoughtfully, with attention to what’s being lost as well as what’s being gained, or whether we’ll wait until the whole thing collapses and scramble to build something new from the rubble.
I hope for the former. I fear it will be the latter.
Bibliography
- American Psychiatric Association. (1952). Diagnostic and Statistical Manual of Mental Disorders (1st ed.). Washington, DC: American Psychiatric Association.
- American Psychiatric Association. (1968). Diagnostic and Statistical Manual of Mental Disorders (2nd ed.). Washington, DC: American Psychiatric Association.
- American Psychiatric Association. (1980). Diagnostic and Statistical Manual of Mental Disorders (3rd ed.). Washington, DC: American Psychiatric Association.
- American Psychiatric Association. (1994). Diagnostic and Statistical Manual of Mental Disorders (4th ed.). Washington, DC: American Psychiatric Association.
- American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders (5th ed.). Washington, DC: American Psychiatric Association.
- Andreasen, N. C. (2007). DSM and the death of phenomenology in America: An example of unintended consequences. Schizophrenia Bulletin, 33(1), 108-112.
- Bentall, R. P. (2004). Madness Explained: Psychosis and Human Nature. London: Penguin Books.
- Campbell, J. (1949). The Hero with a Thousand Faces. New York: Pantheon Books.
- Campbell, J. (1988). The Power of Myth (with Bill Moyers). New York: Doubleday.
- Cooper, J. E., et al. (1972). Psychiatric Diagnosis in New York and London: A Comparative Study of Mental Hospital Admissions. London: Oxford University Press.
- Cosgrove, L., & Krimsky, S. (2012). A comparison of DSM-IV and DSM-5 panel members’ financial associations with industry. PLOS Medicine, 9(3), e1001190.
- Cuthbert, B. N., & Insel, T. R. (2013). Toward the future of psychiatric diagnosis: The seven pillars of RDoC. BMC Medicine, 11, 126.
- Davies, J. (2013). Cracked: Why Psychiatry is Doing More Harm than Good. London: Icon Books.
- Decker, H. S. (2013). The Making of DSM-III: A Diagnostic Manual’s Conquest of American Psychiatry. Oxford: Oxford University Press.
- Ellmann, R. (1982). James Joyce (Revised Edition). Oxford: Oxford University Press.
- Foucault, M. (1961/1965). Madness and Civilization: A History of Insanity in the Age of Reason. New York: Pantheon.
- Frances, A. (2013). Saving Normal: An Insider’s Revolt Against Out-of-Control Psychiatric Diagnosis, DSM-5, Big Pharma, and the Medicalization of Ordinary Life. New York: William Morrow.
- Ghaemi, S. N. (2009). The Rise and Fall of the Biopsychosocial Model: Reconciling Art and Science in Psychiatry. Baltimore: Johns Hopkins University Press.
- Goldstein, R. N. (1983). The Mind-Body Problem. New York: Random House.
- Goldstein, R. N. (2016). The Mattering Instinct: A Conversation With Rebecca Newberger Goldstein. Edge.org.
- Gøtzsche, P. C. (2015). Deadly Psychiatry and Organised Denial. Copenhagen: People’s Press.
- Greenberg, G. (2013). The Book of Woe: The DSM and the Unmaking of Psychiatry. New York: Blue Rider Press.
- Harrington, A. (2019). Mind Fixers: Psychiatry’s Troubled Search for the Biology of Mental Illness. New York: W.W. Norton.
- Horwitz, A. V., & Wakefield, J. C. (2007). The Loss of Sadness: How Psychiatry Transformed Normal Sorrow into Depressive Disorder. Oxford: Oxford University Press.
- Hyman, S. E. (2010). The diagnosis of mental disorders: the problem of reification. Annual Review of Clinical Psychology, 6, 155-179.
- Insel, T. (2013). Director’s Blog: Transforming Diagnosis. National Institute of Mental Health.
- Johnstone, L., & Boyle, M. (2018). The Power Threat Meaning Framework. Leicester: British Psychological Society.
- Jung, C. G. (1934). Letter to James Joyce regarding Lucia Joyce. In C. G. Jung Letters, Vol. 1.
- Kirk, S. A., & Kutchins, H. (1992). The Selling of DSM: The Rhetoric of Science in Psychiatry. New York: Aldine de Gruyter.
- Kotov, R., et al. (2017). The Hierarchical Taxonomy of Psychopathology (HiTOP): A dimensional alternative to traditional nosologies. Journal of Abnormal Psychology, 126(4), 454-477.
- Krueger, R. F., & Markon, K. E. (2006). Reinterpreting comorbidity: A model-based approach to understanding and classifying psychopathology. Annual Review of Clinical Psychology, 2, 111-133.
- Laing, R. D. (1960). The Divided Self: An Existential Study in Sanity and Madness. London: Penguin Books.
- Laing, R. D., & Esterson, A. (1964). Sanity, Madness and the Family. London: Tavistock Publications.
- Mayes, R., & Horwitz, A. V. (2005). DSM-III and the revolution in the classification of mental illness. Journal of the History of the Behavioral Sciences, 41(3), 249-267.
- Moncrieff, J., et al. (2022). The serotonin theory of depression: A systematic umbrella review of the evidence. Molecular Psychiatry.
- Porter, T. M. (1995). Trust in Numbers: The Pursuit of Objectivity in Science and Public Life. Princeton: Princeton University Press.
- Regier, D. A., et al. (2009). DSM-5 field trials in the United States and Canada, Part II: Test-retest reliability of selected categorical diagnoses. American Journal of Psychiatry, 170(1), 59-70.
- Rosenhan, D. L. (1973). On being sane in insane places. Science, 179(4070), 250-258.
- Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons.
- Skodol, A. E. (2012). Personality disorders in DSM-5. Annual Review of Clinical Psychology, 8, 317-344.
- Shloss, C. (2003). Lucia Joyce: To Dance in the Wake. New York: Farrar, Straus and Giroux.
- Szasz, T. S. (1961). The Myth of Mental Illness: Foundations of a Theory of Personal Conduct. New York: Harper & Row.
- Timimi, S. (2017). Non-diagnostic based approaches to helping children who could be labelled ADHD and their families. International Journal of Qualitative Studies on Health and Well-being, 12(sup1), 1298270.
- van der Kolk, B. A. (2014). The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma. New York: Viking.
- Whooley, O. (2019). On the Heels of Ignorance: Psychiatry and the Politics of Not Knowing. Chicago: University of Chicago Press.
- Whitaker, R. (2010). Anatomy of an Epidemic: Magic Bullets, Psychiatric Drugs, and the Astonishing Rise of Mental Illness in America. New York: Crown.
Joel Blackstock, LICSW-S, is the Clinical Director of Taproot Therapy Collective in Hoover, Alabama. He specializes in complex trauma treatment and writes at GetTherapyBirmingham.com.



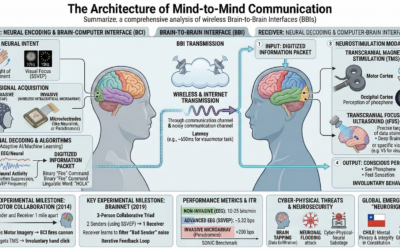














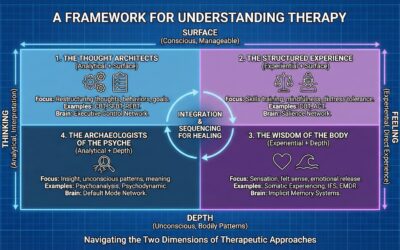
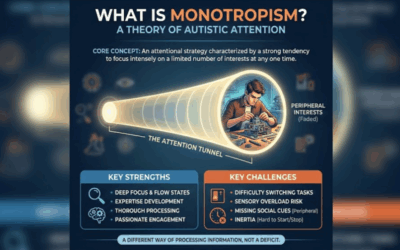

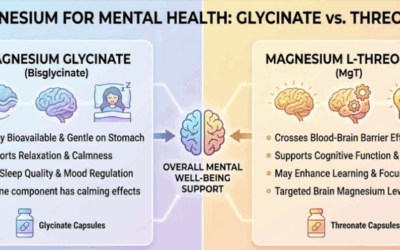



0 Comments