A Critical Investigation into the Document That Defines American Mental Health—and Why It May Have Already Failed
Contents
- Introduction: The Controversial Bible
- Part I: The History of a Document in Crisis
- Part II: The Anti-Psychiatry Assault and the Crisis of Legitimacy
- Part III: The Bureaucratic Counter-Revolution—DSM-III and the Checklist
- Part IV: DSM-IV and the Failed Promise of the “Germ Theory”
- Part V: The Three False Epidemics—Frances’s Confession
- Part VI: DSM-5 and the Incomplete Pivot to Spectrums
- Part VII: Borderline Personality Disorder—A Fossil of a Broken System
- Part VIII: Secrecy, NDAs, and the Politics of Committees
- Part IX: A Comprehensive Survey of Criticisms
- Part X: Observations from the Clinical Trenches
- Part XI: The Tyranny of “Functional”—Why Suffering Should Matter More Than Productivity
- Part XII: Three Conceptual Failures of the DSM System
- Part XIII: The Divorce of Psychiatry and Therapy
- Part XIV: The Neurodivergence Question—What Even Is Normal?
- Part XV: The Insurance Straitjacket
- Part XVI: A Way Forward—Narrative, Systems, and Clinical Intuition
- Bibliography
The Controversial Bible
Love it or hate it, therapists have to use the DSM. The Diagnostic and Statistical Manual of Mental Disorders, published by the American Psychiatric Association, functions as the definitive classification system for mental health conditions in the United States. Every diagnosis we give, every insurance claim we file, every treatment plan we justify—all of it flows through the DSM’s categorical architecture. It is, for all practical purposes, the bible of American psychiatry.
And yet, the fact that we have to diagnose under its criteria is one of the most controversial issues I have encountered in the field. Off the record, approximately half of the therapists I’ve spoken with over my career have enormous problems with the document—not with the idea of diagnosis or diagnostic criteria itself, but with the value structure, the operating assumptions, and the contradictions built into the Evidence Based Practice model as it currently exists.
To understand these cross-purpose assumptions, the shifting scope of conceptualizations, and the seeming contradictions of what the DSM has become, we must look at the history of the thing itself and the forces that it has responded to across its development. What emerges from this investigation is not a story of scientific progress, but a chronicle of defensive reactions—a document shaped more by professional insecurity, insurance mandates, and pharmaceutical economics than by the pure pursuit of understanding human suffering.
“The DSM is not a description of nature. It is a description of what American healthcare requires nature to be.”
This is not an argument against diagnosis. It is not an argument against science. It is an argument that we should look for problems with the way we conduct science in order to make it more scientific—and that we should make diagnostic criteria capable of confronting the mental health crisis we are now presented with, rather than serving the profit motives of healthcare corporations and the nonsensical hierarchies of academia.
Part I: The History of a Document in Crisis
The Dynamic Era: DSM-I and DSM-II (1952–1980)
To understand the significance of the “checklist” model that dominates contemporary psychiatry, one must first understand what it replaced. The first edition of the DSM, published in 1952, and its successor, DSM-II (1968), were fundamentally different documents from the manuals used today. They were products of their time, heavily influenced by the psychodynamic and psychoanalytic theories that dominated American psychiatry in the post-World War II era.1
In this “dynamic” paradigm, mental disorders were not viewed as discrete, static disease entities analogous to distinct bacterial infections. Instead, they were conceptualized as “reactions”—fluid, dynamic processes resulting from the interplay between an individual’s internal personality structure and environmental stressors. The nomenclature of DSM-I explicitly used the term “reaction” for many conditions (e.g., “Schizophrenic reaction,” “Depressive reaction”), reflecting the belief that symptoms were a manifestation of the patient’s struggle to adapt to psychological conflict.2
This model was inherently dimensional in its philosophy, albeit not in a mathematical sense. It viewed pathology as a matter of degree rather than kind. A “neurosis” was not a separate species of existence but an exaggeration of normal defense mechanisms. The diagnosis required a deep, interpretive understanding of the patient’s life history, unconscious conflicts, and personality dynamics.
The diagnostic criteria in DSM-I and DSM-II were not lists of symptoms but narrative paragraphs—short descriptions of a prototype that the clinician was expected to match against the patient’s presentation. This relied heavily on the clinician’s interpretive skill and theoretical orientation. A psychiatrist trained in Freudian psychoanalysis might interpret a patient’s silence as “resistance” rooted in an anal-retentive personality structure, while a psychiatrist with a more biological or social orientation might see it differently.3 The first version of the DSM stated explicitly that the document would never be used for reimbursement or billing, but that did not last long.
The Reliability Crisis
While this approach offered a rich, humanistic, and individualized view of suffering, it failed the fundamental test of scientific medicine: reliability. Reliability refers to the consistency of a measurement; if two psychiatrists see the same patient, they should arrive at the same diagnosis. Throughout the 1960s and 1970s, a series of landmark studies exposed the catastrophic lack of reliability in the dynamic model.
The most famous of these was the US-UK Diagnostic Project, which compared diagnostic practices in New York and London. The study found that American psychiatrists diagnosed schizophrenia much more frequently than their British counterparts, who were more likely to diagnose manic-depressive illness (bipolar disorder) for the same clinical presentation.4 This demonstrated that “schizophrenia” in the DSM-II era was not a stable biological entity but a culturally and theoretically dependent construct.
The collapse of reliability was not just an academic embarrassment; it was an existential threat to psychiatry. Without a reliable diagnostic system, epidemiology was impossible—researchers could not count how many people had a disorder if they couldn’t agree on what the disorder was.
Part II: The Anti-Psychiatry Assault and the Crisis of Legitimacy
By the 1960s, the insularity of psychiatry was shattered. The cultural revolution of the decade brought all forms of authority into question, and the psychiatrist—as the arbiter of normality—became a prime target.
R.D. Laing and the Intelligibility of Madness
R.D. Laing, a Scottish psychiatrist, struck at the heart of the medical model’s assumption that mental illness was a “breakdown” of function. In seminal works like The Divided Self (1960), Laing argued that what looked like “madness” was often a sane, intelligible strategy for surviving an unlivable situation.5
Laing posited that the “schizophrenic” was not a broken machine but an existential voyager. He suggested that the bizarre speech and behavior of the psychotic were coded communications about the “double binds” and mystifications imposed by their families and society. “The divided self,” Laing wrote, was a protective reaction to a world that demanded a false self.5
This perspective was terrifying to the mainstream psychiatric establishment because it dissolved the boundary between doctor and patient. If the patient’s delusions were actually poetic truths about their oppression, then the psychiatrist’s attempt to “cure” them with drugs or shock therapy was not medical benevolence, but political violence. Laing’s work suggested that the diagnosis itself was the problem—an act of alienation that stripped the subject of their agency and humanity.
Thomas Szasz and the Myth of Mental Illness
While Laing attacked from the left (existentialism/socialism), Thomas Szasz attacked from the right (libertarianism). In The Myth of Mental Illness (1961), Szasz dismantled the logical coherence of the psychiatric enterprise. He argued that the concept of “mental illness” was a category error, a semantic trap.7
Szasz’s syllogism was ruthless:
1. Illness is a structural or functional deviation of the body (pathology).
2. The “mind” is not a physical organ; it is a concept.
3. Therefore, there can be no “illness” of the mind, only “problems in living.”—Thomas Szasz, The Myth of Mental Illness (1961)
Szasz contended that psychiatry was a pseudoscience used by the state to police social deviance. By labeling behaviors as “illnesses,” society avoided the difficult ethical work of dealing with conflict. The “mental illness” label allowed the state to incarcerate innocent people (involuntary commitment) without the due process of the criminal justice system.9
For the founders of the modern DSM, Szasz was not just a critic; he was an existential threat who denied the very reality of the phenomena they treated.
Rosenhan and the “Thud” Experiment
If Laing and Szasz provided the theoretical indictment of psychiatry, David Rosenhan provided the empirical conviction. His 1973 study, published in Science under the title “On Being Sane in Insane Places,” was a masterstroke of experimental sociology that targeted the “subjective intuition” of the clinician.10
Rosenhan’s protocol was deceptively simple. He recruited eight “pseudopatients”—sane individuals with no history of mental illness, including a psychology graduate student, a pediatrician, a psychiatrist, a painter, and a housewife. Their instructions were precise: present to a psychiatric hospital admissions office and complain of hearing voices. The voices are unfamiliar, of the same sex, and say only three words: “empty,” “hollow,” and “thud.”11
Beyond this single fabrication (and falsifying their names/occupations), they were to be completely truthful about their life histories and behave normally. The choice of words—”empty, hollow, thud”—was calculated. Rosenhan chose them because they suggested existential distress (a Laingian crisis of meaning) rather than typical psychotic content. They were abstract, ambiguous signals.
12 of 12 students were psychiatrically admitted
All twelve admissions resulted in a diagnosis of serious mental illness—eleven as schizophrenia, one as manic-depressive psychosis.
The most damning finding was not the admission itself (doctors are trained to err on the side of caution), but the stickiness of the label. Once the pseudopatients were admitted, they ceased simulating symptoms. They spoke normally, behaved cooperatively, and told the staff they felt fine. Yet, the staff—blinded by the diagnostic label—reinterpreted their normal behavior as pathological.12
When pseudopatients took notes on their experiences, nurses recorded this in the chart: “Patient engages in writing behavior,” interpreting it as a compulsive symptom of their psychosis. Boredom-induced walking was seen as “nervousness” or agitation. The average daily contact with doctors was 6.8 minutes.12
When they were finally discharged—after an average of 19 days, with one staying 52 days—they were not declared “sane” or “misdiagnosed.” They were discharged with a diagnosis of “Schizophrenia in Remission.”13 The label was indelible. The implication was that the illness was still there, lurking, merely dormant.
Rosenhan’s conclusion was stark: “The salient characteristics that lead to diagnosis reside in the patients’ environments and not within the patients themselves.”10 He had proven that the “clinical gaze”—the intuitive ability of the expert to see the illness in the patient—was a myth. The context (the “insane place”) overpowered the reality of the person.
Table 1: The Rosenhan Effect on Diagnostic Practice
| Rosenhan’s Element | The “Anti-Psychiatry” Implication | The DSM-III “Bureaucratic” Counter-Measure |
|---|---|---|
| “Empty, Hollow, Thud” | Existential distress (Laingian meaning) can be misread as psychosis | Specific Hallucination Criteria: Voices must be “distinct,” distinct from one’s own thoughts; bizarre vs. non-bizarre distinctions added |
| “In Remission” | The label is sticky; the person is permanently marked as “insane” | Course Specifiers: Explicit rules for “Full Remission,” “Partial Remission,” requiring specific timeframes (e.g., no symptoms for 6 months) |
| Writing as Symptom | Context (the hospital) pathologizes normal behavior | Exclusion Criteria: “The behavior is not better explained by…” (Attempt to force clinicians to rule out context) |
| Subjective Intuition | Doctors rely on “feeling” rather than facts | The Checklist: Remove the “feeling.” If criteria A, B, and C are met, the diagnosis is mandatory (in theory) |
The Forces Converging on Psychiatry
By the early 1970s, these intellectual critiques had coalesced into a full-blown crisis of legitimacy. Psychiatry was under siege from multiple directions:
| Force | Their Critique |
|---|---|
| Civil Rights Activists | Viewed involuntary commitment as a violation of liberty |
| Gay Rights Activists | Challenged the classification of homosexuality as a disorder |
| The Public | Influenced by films like One Flew Over the Cuckoo’s Nest, saw psychiatrists as authoritarian enforcers |
| Scientific Researchers | Studies showed inter-rater reliability was abysmal |
| Insurance Companies | Unwilling to pay for vague “reactions” or open-ended psychoanalysis |
| Pharmaceutical Industry | Needed homogenous patient populations for randomized controlled trials |
The profession was viewed as “soft,” subjective, and politically compromised. The stage was set for a counter-revolution.
Part III: The Bureaucratic Counter-Revolution—DSM-III and the Checklist
Robert Spitzer and the “Data-Oriented” Outsider
The publication of DSM-III in 1980 is widely regarded as a watershed moment in the history of psychiatry, often termed the “Neo-Kraepelinian revolution” (named after Emil Kraepelin, the father of descriptive psychiatry). Its architect, Robert Spitzer, designed it as a fortress of Reliability to withstand the siege on Validity.
Robert Spitzer was the singularity at the center of the DSM-III universe. A professor at Columbia University, he was described by colleagues as a brilliant but socially awkward “outsider.”14 He had undergone psychoanalytic training, but he never fit the mold of the empathetic, interpretative analyst. Spitzer was uncomfortable with ambiguity. In the hazy world of 1970s psychiatry, he was a man obsessed with categorization and data. He had been “kicked upstairs” to administrative roles because he lacked the clinical warmth prized by the establishment, a rejection that perhaps fueled his desire to dismantle the system that had marginalized him.15
The “Atheoretical” Compromise
Spitzer’s strategic genius was the decision to make the DSM-III “atheoretical.”16
The problem was that the field was fractured. Psychoanalysts believed depression was caused by anger turned inward; biological psychiatrists believed it was a chemical imbalance; behaviorists believed it was learned helplessness. They could not agree on cause (etiology).
Spitzer’s reaction: propose a manual that ignored cause entirely. It would focus solely on description. It didn’t matter why the patient was depressed; it only mattered that they had “depressed mood, insomnia, weight loss, and fatigue for 2 weeks.”17
This was a diplomatic masterstroke. It allowed Freudians and biological psychiatrists to use the same codes. But it was also a philosophical retreat. By abandoning the “why” (the reaction paradigm), the DSM-III stripped the diagnosis of its meaning. It became a taxonomy of surfaces.
The Checklist: Bureaucracy as Science
The core innovation of DSM-III was the introduction of Operational Criteria (checklists). This methodology was imported from the “Feighner Criteria” (1972) and the “Research Diagnostic Criteria” (RDC), developed by a group of “Neo-Kraepelinians” at Washington University in St. Louis.18
This group believed that psychiatry’s only hope for scientific status was to emulate the descriptive rigor of Emil Kraepelin. They rejected the “vague” descriptions of DSM-II in favor of explicit rules:
Inclusion Criteria: “At least 4 of the following 8 symptoms…”
Exclusion Criteria: “Not due to a physical disorder…”
Duration Criteria: “Symptoms present for at least 6 months…”
Why was this considered “more scientific”? The founders conflated Reliability with Validity.19
Table 2: Reliability vs. Validity—The Fundamental Trade-off
| Concept | Definition | The DSM-III Choice | The Long-Term Result |
|---|---|---|---|
| Reliability | The extent to which two clinicians agree on a diagnosis (Kappa score) | PRIORITIZED: Checklists ensure Dr. A and Dr. B agree | False Consensus: Doctors agree on labels that may not be real diseases (e.g., “DSM Schizophrenia”) |
| Validity | The extent to which the diagnosis represents a real, distinct biological entity | SACRIFICED: “Atheoretical” approach ignored cause to achieve consensus | Scientific Stagnation: Research on heterogeneous groups yielded no biomarkers after 40 years |
The Rosenhan experiment had destroyed psychiatry’s reliability. The checklist was the fix. If Dr. A and Dr. B both had to check off the same boxes, they would likely agree on the diagnosis. The Kappa statistic (a measure of agreement) became the god of the DSM-III task force.19
This shift to bureaucratic methodology—the “tick-the-box” approach—was a direct reaction to the “subjective intuition” trap. It removed the clinician’s judgment from the equation. If the patient met the criteria, they had the disorder, regardless of the clinician’s “feeling” about the case. It was a defense mechanism: “I didn’t diagnose you; the Manual did.”
The Reification of Disorder
The checklist system succeeded brilliantly in its primary goal: improving inter-rater reliability. By focusing on surface-level symptoms (“what the patient says and does”) rather than deep structure (“why the patient does it”), clinicians could achieve high rates of agreement.20
However, this victory came at a significant cost: validity. Critics argued that DSM-III prioritized reliability over validity. By carving up the landscape of mental distress into discrete categories based on surface symptoms, the DSM created the illusion that these disorders were “natural kinds”—distinct diseases like tuberculosis or diabetes—when in fact they were merely clusters of symptoms that often co-occurred.21
This era saw the “reification” of psychiatric disorders. A diagnosis of “Major Depression” became treated as a thing that a person has, rather than a description of what a person is experiencing. This reification was immensely profitable for the pharmaceutical industry. The clear-cut categories provided specific targets for drug development and marketing. If a drug could be shown to reduce the symptom count on the checklist, it could be approved and marketed for that specific disorder.22
The Forces of Enforcement: Insurance and Pharma
This bureaucratic turn was not just an intellectual preference; it was an economic necessity required by the external forces Spitzer was combatting.
The Insurance Mandate: By the 1970s, third-party payers (insurance companies) were refusing to reimburse for vague diagnoses like “anxiety reaction” or open-ended psychoanalysis.16 They demanded accountability. The “atheoretical” codes of DSM-III provided the specific “products” that insurers could price and track. The checklist turned mental illness into a billable unit.
The Pharmaceutical Capture: Spitzer later admitted, “the pharmaceuticals were delighted” with the DSM-III.23 The checklist system created a perfect target for drug development.
In the 1970s, the drug company Upjohn developed Xanax. They wanted a specific indication for it, separate from general anxiety (which was crowded with Valium). Spitzer, working closely with researchers funded by Upjohn, carved “Panic Disorder” out of “Anxiety Neurosis.” Despite objections from experts like Isaac Marks (who argued panic was situational), Spitzer pushed it through.24 The new “bureaucratic” category created a billion-dollar market for Xanax. The “scientific” distinction was, in part, a corporate product.
The Death of Phenomenology
The victory of DSM-III was total. It saved the profession, re-medicalized the field, and satisfied the insurers. But it came at a terrible cost: the “Death of Phenomenology.”25
Nancy Andreasen, a leading psychiatrist, argued that by focusing entirely on “observable behaviors” (to satisfy reliability), clinicians lost the ability to see the subtle, internal experiences of the patient. The deep, empathetic interviewing skills of the earlier era atrophied. Psychiatry became a clerical task of symptom counting. The “thud” was no longer heard; it was just tallied.
Part IV: DSM-IV and the Failed Promise of the “Germ Theory”
The Unspoken Wager
Implicit in the DSM-III revolution was a wager: if we just define the phenotypes (symptoms) reliably, the genotypes (genes) and biological mechanisms would eventually be found. The categorical system was a placeholder—a pragmatic holding pattern while neuroscience caught up.
The assumption, never fully articulated but pervading the research community, was that psychiatry would soon have its own “germ theory.” Just as medicine discovered specific pathogens for specific diseases, psychiatry would discover specific brain lesions, neurotransmitter imbalances, or genetic markers for specific mental disorders. The DSM categories would eventually be validated by biology.
This did not happen.
The Problem of Comorbidity
As the checklist system matured through DSM-III-R (1987) and DSM-IV (1994), cracks began to appear in the categorical facade. The primary problem was “comorbidity.” In a true categorical system (like the periodic table of elements), entities are distinct; an atom is either gold or lead, not both. In DSM-IV, however, it was the norm for patients to meet the criteria for multiple disorders simultaneously—a patient might have Major Depression, Generalized Anxiety Disorder, and Panic Disorder all at once.26
This massive comorbidity suggested that the boundaries between these “discrete” disorders were artificial. Furthermore, a huge proportion of patients failed to fit the strict checklists and were diagnosed with “Not Otherwise Specified” (NOS) categories (e.g., PDD-NOS, ED-NOS). The NOS diagnosis became the most common diagnosis in many clinics, a silent admission that the rigid templates of the checklist failed to capture the messy reality of human psychopathology.27
Allen Frances and the Conservative Reaction
By the early 1990s, the “reaction” of DSM-III had generated its own crisis: Diagnostic Inflation. The checklists were so easy to use, and so divorced from context, that the boundaries of mental illness were expanding rapidly. “Normal” human suffering—grief, shyness, boisterousness—was being captured by the bureaucratic net of the DSM.
Allen Frances, the chair of the DSM-IV task force, was a student of Spitzer, but his insecurity was different. He feared that the DSM was becoming a victim of its own success, expanding “the boundary of psychiatry far beyond its competence.”28
Frances explicitly framed DSM-IV as a “conservative” reaction. His goal was to “hold the line” against the proliferation of new disorders. He imposed strict evidentiary standards: no new diagnosis would be added without overwhelming scientific proof that it would do more good than harm.29
Part V: The Three False Epidemics—Frances’s Confession
Despite his conservative intentions, Allen Frances later publicly apologized for “failing to predict or prevent three new false epidemics” that emerged from the DSM-IV. This confession from the chair of the task force himself is perhaps the most damning indictment of the diagnostic system.
Table 3: The Three False Epidemics Created by DSM-IV
| The Epidemic | The Mechanism of Inflation | The “Reaction” Failure |
|---|---|---|
| ADHD | Criteria allowed diagnosis based on school performance constraints and subjective teacher reports | 10% of US children diagnosed; driven by Pharma marketing to parents and schools28 |
| Bipolar II | Loosening of criteria for “hypomania” (milder highs) that captured ordinary mood swings | Captured patients with normal mood variability; drove massive sales of mood stabilizers and antipsychotics67 |
| Autism/Asperger’s | Introduction of Asperger’s Disorder as a milder form of autism | Expanded the “spectrum” to include high-functioning eccentricity; diagnostic rates skyrocketed68 |
ADHD: The Medicalization of Childhood
The ADHD epidemic is perhaps the most visible example of diagnostic inflation. The criteria in DSM-IV allowed diagnosis based heavily on reports from teachers about classroom behavior—inattention, fidgeting, difficulty following instructions. In a school system with increasing demands for standardized testing and decreasing tolerance for behavioral variation, normal childhood restlessness became pathology.
Sami Timimi, a child psychiatrist and critic of the ADHD construct, argues that there is no biomarker for ADHD—no blood test, no brain scan, no genetic assay that can diagnose it. He contends that the diagnosis serves a social function: it “exonerates” parents and schools. By labeling a distracted child as “diseased,” the school avoids changing its rigid curriculum, and parents avoid blame for family dysfunction. It repackages social problems as a biological defect in the child.55 Adult ADHD has similarly exploded as a diagnosis, often overlapping with the effects of modern technology.
Bipolar II: Capturing Normal Mood
The expansion of the bipolar spectrum to include “Bipolar II”—characterized by depressive episodes and milder “hypomanic” episodes—opened the floodgates. The criteria for hypomania were vague enough that periods of elevated mood, increased productivity, or decreased need for sleep (common experiences during exciting life events) could qualify.
This had massive pharmaceutical implications. Patients who might previously have been diagnosed with depression were now diagnosed with Bipolar II, which changed their treatment protocol entirely—from antidepressants to mood stabilizers and antipsychotics, drugs with far more significant side effect profiles and higher profit margins.
Autism: From Rare to Common
The introduction of Asperger’s Disorder in DSM-IV expanded the autism umbrella to include individuals with social difficulties but without language delays or intellectual disability. While this brought services to many who needed them, it also captured a vast population of socially awkward but fundamentally neurotypical individuals. The diagnostic rate of autism went from approximately 1 in 2,500 in the 1980s to 1 in 36 today.60 This has led to many adults asking, “Have you always felt different?” and seeking late-in-life diagnosis.
The lesson of DSM-IV was that bureaucratic methodologies are inherently inflationary. Once a checklist exists, the pressure from patients (seeking validation), parents (seeking school services), and pharmaceutical companies (seeking customers) forces the gate open.
Part VI: DSM-5 and the Incomplete Pivot to Spectrums
The Ambition of Dimensionality
The development of DSM-5, which began in 1999, was driven by a desire to integrate the emerging insights of neuroscience and genetics. Research indicated that mental disorders were not discrete silos but shared significant genetic risks and neural circuit disruptions. The DSM-5 Task Force, led by David Kupfer, initially aimed for a “paradigm shift” toward dimensional measures.31
The goal was to replace the binary “present/absent” logic of the checklist with a “spectrum” approach. This would acknowledge that traits like anxiety, psychosis, and mood dysregulation are distributed continuously in the population, much like hypertension or obesity. A “spectrum” model would allow clinicians to rate the severity of symptoms and cross-cutting domains (e.g., sleep, cognition) regardless of the primary diagnosis.32
The Collision with Reality
Despite high aspirations, the publication of DSM-5 in 2013 was met with widespread disappointment and controversy. The ambitious dimensional models were largely scaled back or relegated to the appendix (Section III), and the main text (Section II) retained the familiar categorical structure, albeit with some “spectrum” rebranding.33
Table 4: Comparative Analysis of Diagnostic Paradigms
| Feature | Dynamic/Process Era (DSM-I/II) | Categorical/Checklist Era (DSM-III/IV) | Nominal Spectrum Era (DSM-5/5-TR) |
|---|---|---|---|
| Core Unit | Reaction / Process | Discrete Disorder Category | Spectrum / Umbrella Category |
| Diagnostic Logic | Interpretive / Narrative | Algorithmic / Threshold (n of x symptoms) | Hybrid (Threshold + Severity Specifiers) |
| Reliability | Low (Subjective) | High (Operationalized) | Moderate (Variable by Spectrum) |
| Validity | Low (Theory-bound) | Low (Artifactual boundaries) | Mixed (Conceptual improvement, operational lag) |
| Underlying Theory | Psychoanalytic / Psychodynamic | Atheoretical / Descriptive | Biopsychosocial / Dimensional (Aspirational) |
| Primary Driver | Clinical intuition, Defense mechanisms | Inter-rater agreement, Research categorization | Integration of genetics, Comorbidity reduction |
Case Study 1: The Autism Spectrum Consolidation
The most visible shift to spectrum terminology in DSM-5 was the creation of Autism Spectrum Disorder (ASD). This new diagnosis absorbed four separate DSM-IV categories: Autistic Disorder, Asperger’s Disorder, Childhood Disintegrative Disorder, and Pervasive Developmental Disorder-Not Otherwise Specified (PDD-NOS).27
The scientific rationale for this consolidation was robust. Longitudinal and cluster analysis data suggested that the distinction between “Autism” and “Asperger’s” was largely artificial. Clinicians at different sites were applying these labels inconsistently. Dr. Catherine Lord, a key member of the Neurodevelopmental Work Group, famously remarked that trying to separate these conditions was like “trying to carve meatloaf at the joints”—an impossible task because no natural boundaries existed.34 This shift has helped in illuminating the kaleidoscope of neurodivergence, but implementation has been messy.
However, the operationalization of the ASD spectrum raised significant concerns. Research indicated that while the specificity of the DSM-5 criteria was superior (0.97 vs. 0.86 for DSM-IV), the sensitivity was lower (0.81 vs. 0.95).35 This meant that a significant subset of individuals—particularly those with higher cognitive functioning or those previously diagnosed with PDD-NOS—might lose their diagnosis and access to services under the new “spectrum” rules.
In practice, the Autism Spectrum is a Nominal Spectrum. It uses dimensional language (“Levels 1, 2, 3”) but retains a binary gatekeeping function. One is either “on the spectrum” (meeting the threshold criteria) or “off.” The severity levels are broad administrative buckets rather than precise quantitative measures.36
Case Study 2: Schizophrenia and the Ghost of Attenuated Psychosis
DSM-IV divided Schizophrenia into distinct subtypes: Paranoid, Disorganized, Catatonic, Undifferentiated, and Residual. The DSM-5 abolished these subtypes entirely, as they had poor diagnostic stability and failed to predict treatment response.37 Understanding Schizophrenia remains a challenge when the diagnostic criteria shift so dramatically between editions.
In place of subtypes, DSM-5 introduced the concept of a “Schizophrenia Spectrum and Other Psychotic Disorders.” However, the implementation of this spectrum was severely compromised by the rejection of Attenuated Psychosis Syndrome (APS) from the main text. APS was designed to capture the “prodromal” phase of psychosis—individuals exhibiting mild or transient psychotic symptoms who are at high risk for developing full-blown schizophrenia. Including APS would have been the cornerstone of a true spectrum model.38
Critics, including Allen Frances, argued that diagnosing “Attenuated Psychosis” would lead to the massive medicalization of weird or eccentric adolescents. The false-positive rate for predicting conversion to full psychosis is high (around 70% of “high risk” individuals do not convert within two years), raising the specter of thousands of teenagers being unnecessarily treated with potent antipsychotic drugs.39
The decision to relegate APS to Section III (“Conditions for Further Study”) effectively maintained the binary wall between “Normal” and “Psychotic.” While the chapter title says “Spectrum,” the diagnostic criteria remain rigidly categorical.
Case Study 3: The Civil War Over Personality Disorders
The tension between the “checklist” and the “spectrum” reached its apex in the Personality Disorders (PD) Work Group. This conflict provides the clearest evidence of the institutional inertia preventing true dimensional reform.
The DSM-IV model of personality disorders (10 distinct categories like Narcissistic, Borderline, Avoidant) was widely recognized as scientifically bankrupt. The comorbidity rates were astronomical; patients meeting criteria for one PD routinely met criteria for three or four others. The most common diagnosis was “PD-NOS.”40
The PD Work Group proposed a radical overhaul: the Alternative Model for Personality Disorders (AMPD). This model was fully dimensional, based on the robust “Big Five” trait theory of personality. It consisted of two main components:41
Criterion A: Level of Personality Functioning (a 0-4 rating of impairments in Self and Interpersonal functioning).
Criterion B: Pathological Personality Traits (25 specific trait facets organized into 5 domains: Negative Affectivity, Detachment, Antagonism, Disinhibition, and Psychoticism).
This model was backed by extensive factor analysis and empirical data. It solved the comorbidity problem by describing a patient’s unique profile of traits rather than forcing them into a category.42
The Administrative Veto: Despite the scientific consensus of the Work Group, the APA Board of Trustees voted to reject the AMPD for the main text of DSM-5. The model was exiled to Section III. Section II retained the old, scientifically inferior DSM-IV categories—the very checklists the Work Group had spent a decade proving were invalid.40
The reasons cited for this veto were revealing. The Board argued that the dimensional model was “too complex” for average clinicians to use in routine practice and would be “unworkable” for coding and billing.41 They prioritized clinical utility (familiarity, ease of use) and administrative stability over scientific validity.
“This decision is the ‘smoking gun’ of the DSM-5’s failure to realize a spectrum approach. When presented with a scientifically superior spectrum model, the institution chose to stick with the checklist because the checklist is the currency of the mental health economy.”
The NIMH Abandonment
The final and most devastating reaction came from the federal government. On the eve of DSM-5’s publication, Thomas Insel, Director of the National Institute of Mental Health (NIMH), announced that the institute would no longer use DSM categories to fund research.43
Insel’s critique was direct: while the DSM had achieved Reliability (the DSM-III goal), it had failed at Validity.
“The strength of each of the editions of DSM has been ‘reliability’… The weakness is its lack of validity… We cannot succeed if we use DSM categories as the ‘gold standard.'”
—Thomas Insel, 2013
The NIMH launched the Research Domain Criteria (RDoC), a framework that ignores DSM diagnoses entirely in favor of studying basic biological constructs (like “Fear Circuitry” or “Working Memory”).44
This was the full circle. The system built to save psychiatry (DSM-III) was now rejected by the highest scientific body as the primary obstacle to progress.
Part VII: Borderline Personality Disorder—A Fossil of a Broken System
If you want to understand everything wrong with the DSM in a single diagnosis, look at Borderline Personality Disorder. It is a fossil—an artifact of an older conceptual system that has been carried forward through successive revisions despite being scientifically incoherent.
The Origin of “Borderline”
The term “borderline” emerged in the psychoanalytic era to describe patients who seemed to exist on the “border” between neurosis and psychosis—not quite sick enough for the asylum, but too disturbed for ordinary talk therapy. It was, from the beginning, a wastebasket diagnosis—a category for patients who didn’t fit anywhere else.40
When DSM-III arrived with its checklist revolution, Borderline Personality Disorder was codified with specific criteria: a pattern of instability in relationships, self-image, and affects, along with marked impulsivity. Nine criteria, five required for diagnosis. It looked scientific. It wasn’t.
The Comorbidity Catastrophe
The problems with BPD illustrate the fundamental failure of the categorical model:
Table 5: The Comorbidity Problem with Borderline Personality Disorder
| Issue | Evidence | Implication |
|---|---|---|
| Massive Comorbidity | Patients meeting BPD criteria routinely meet criteria for 3-4 other personality disorders simultaneously | The “boundaries” between disorders are artificial; is BPD really multiple disorders? |
| Gender Bias | BPD is diagnosed in women at approximately 3:1 ratio compared to men | The criteria may be capturing gendered expressions of distress rather than a biological entity, often ignoring the Medea Complex and feminine rage. |
| Trauma Overlap | 70-80% of BPD patients have histories of childhood abuse or neglect | BPD may be better understood as a trauma response than a “personality” pathology, overlapping heavily with narcissistic abuse recovery. |
| Heterogeneity | 256 different symptom combinations can qualify for BPD diagnosis | Two patients with BPD may share only one symptom in common |
| Poor Inter-rater Reliability | DSM-5 field trials showed Kappa of 0.54 for BPD—barely better than chance | Clinicians still can’t agree on who has it, despite 40 years of “operational criteria” |
The Stigma Machine
BPD has become one of the most stigmatized diagnoses in mental health—not just among the public, but among clinicians themselves. Studies have shown that mental health professionals view BPD patients as more “difficult,” less deserving of empathy, and less likely to benefit from treatment compared to patients with other diagnoses.69
This stigma is built into the diagnostic criteria themselves. Terms like “manipulative,” “attention-seeking,” and “unstable” are coded into the clinical description, transforming a description of suffering into a moral judgment. The diagnosis pathologizes the patient’s character, not just their symptoms.
What BPD Actually Is: A Trauma Response Misnamed
Bessel van der Kolk and others have argued that what we call BPD is, in most cases, better understood as Complex PTSD or Developmental Trauma Disorder—the long-term effects of chronic childhood abuse, neglect, or invalidation. Van der Kolk fought to include Developmental Trauma Disorder in DSM-5 specifically to provide an alternative framework for these patients. The APA rejected it.56 Patients with these symptoms are often navigating the echoes of trauma in a way the manual fails to capture.
Why? Because acknowledging that BPD is a trauma response would implicate the caregiving system. A biological label like “Borderline Personality” locates the problem in the patient’s “broken brain” or “bad character”—effectively exonerating the parents and the social environment from their role in the patient’s distress. It is easier to say someone has a disordered personality than to say they were systematically harmed by the people who were supposed to protect them.
The Fossil Persists
The Alternative Model for Personality Disorders (AMPD) would have dissolved BPD into a dimensional profile of traits—high Negative Affectivity, high Disinhibition, high Antagonism, with specific impairments in identity and interpersonal functioning. This would have been more scientifically accurate and less stigmatizing.
But the APA Board rejected the AMPD. So the fossil remains in Section II, used every day to label and stigmatize patients whose primary crime was being hurt as children. BPD is not a scientific category. It is a monument to the DSM’s failure to evolve.
Part VIII: Secrecy, NDAs, and the Politics of Committees
One of the most troubling aspects of the DSM development process is its opacity. The creation of diagnostic criteria that will affect millions of lives occurs largely behind closed doors, shielded by non-disclosure agreements and institutional secrecy.
Gary Greenberg, a psychotherapist who embedded himself in the DSM-5 process, exposed the “horse-trading” that characterizes these deliberations. He documents how diagnoses were voted into existence based on professional rivalries rather than data—exchanges that amounted to “I’ll give you your diagnosis if you give me mine.”45
James Davies, a medical anthropologist, interviewed DSM task force members who admitted they had no scientific proof for where to draw the line between “normal” and “disorder.” He highlights the 1973 vote on homosexuality as proof that the manual reflects changing cultural values, not biological truths. In that vote, homosexuality was removed from the DSM—not because new scientific evidence had emerged about the condition, but because the membership of the APA voted to declassify it following pressure from gay rights activists.46 This echoes the legacy of Dr. John E. Fryer, whose testimony changed the field.
The secrecy surrounding the DSM-5 development was particularly notable. Members of the work groups were required to sign non-disclosure agreements, preventing them from discussing the deliberations publicly. This meant that the reasoning behind many controversial decisions—the rejection of the AMPD, the creation of new diagnoses like Disruptive Mood Dysregulation Disorder—remained hidden from the profession and the public.
Perhaps we should acknowledge that the system of making the DSM itself is not terribly scientific. After all, in the effort to make psychiatry a hard science, what we’ve done is created a committee of people who sit around and—without real hard science to guide them—use their subjective judgment to create these criteria anyway. The committees simply aggregate subjective opinions and call the result objective. This is a recurring theme in the weird history of psychotherapy.
Table 6: The Cycle of Reactions in DSM History
| Phase | The Insecurity (Internal Crisis) | The Force Combatting (External Threat) | The Reaction (Methodology) | The Unintended Consequence |
|---|---|---|---|---|
| DSM-I & II (1952-1970) | Subjectivity: Lack of agreement; “dirty secret” of unreliability | Anti-Psychiatry (Laing, Szasz); Rosenhan Study (1973) | Defense of the Medical Model: Rejection of “Reaction” term; search for rigor | Legitimacy crisis; public perception of fraudulence |
| DSM-III (1980) | Illegitimacy: Fear of being “pseudoscience”; Rosenhan’s humiliation | Insurance mandates; Gay Rights; “Pseudoscience” charges | Bureaucracy: Operational Criteria (Checklists); “Atheoretical” stance; Reliability focus | “Death of Phenomenology”: Loss of meaning; Pharma capture; Diagnostic Inflation |
| DSM-IV (1994) | Inflation: Fear of “medicalizing normality”; expanding boundaries | Rising healthcare costs; public skepticism of “fads” | Conservatism: “Clinical Significance Criterion” (Impairment clause); High evidentiary thresholds | False Epidemics: Failure to contain ADHD, Bipolar II, Autism; Subjectivity of “impairment” |
| DSM-5 (2013) | Invalidity: Criteria don’t match Neuroscience/Genetics | NIMH (Insel); Stagnation of drug development | Abortive Dimensionality: Failed attempt to add spectra; Retreat to categories | Fragmentation: NIMH “divorce” (RDoC); Civil war within psychiatry |
Part IX: A Comprehensive Survey of Criticisms
Criticisms of the DSM have been vast and sustained, coming from virtually every field that touches on mental health—neuroscience, sociology, philosophy, clinical psychology, and the survivor/consumer movement. Here I present the major critics and their arguments, organized by the type of challenge they pose.
The Epistemological Critique: The Crisis of Validity
These critics argue that the DSM fails the basic tests of science: it prioritizes consensus (voting) over discovery (biology).
In a landmark 2013 statement, Insel dealt a massive blow to the DSM’s scientific credibility. He announced the NIMH would shift funding away from DSM categories because they lacked validity. He famously argued that the DSM is “at best a dictionary,” noting that unlike the rest of medicine, which diagnoses based on biological causes (e.g., blood tests, EKGs), the DSM relies on consensus votes about symptom clusters.43
His 1973 experiment, “On Being Sane in Insane Places,” proved that psychiatric diagnosis resides in the mind of the observer, not the patient. Rosenhan sent healthy “pseudopatients” to hospitals claiming to hear a voice saying “thud.” All were admitted and diagnosed with schizophrenia. Once inside, they acted normally, yet their behaviors were interpreted by staff as symptoms of their illness. This demonstrated that the diagnostic labels created a lens that distorted reality, rendering the sane indistinguishable from the insane within the medical system.10 When the State Became the Patient, the diagnostic process became a tool of power.
Author of On the Heels of Ignorance, Whooley argues that psychiatry is defined by “collective ignorance.” He contends that the successive revisions of the DSM (III, IV, 5) were not scientific advancements but “professional reinventions” designed to mask the fact that the field has failed to find the biological causes of mental illness. He views the DSM as a rhetorical tool: by standardizing the language of description, psychiatry hid its lack of explanation, maintaining its authority in the face of an “epistemic void.”47
Author of The Rise and Fall of the Biopsychosocial Model, Ghaemi critiques the DSM for being “anti-scientific” due to its reliance on a “dogmatic eclecticism” (the Bio-Psycho-Social model). He argues that by trying to include every perspective, the DSM explains nothing. He asserts that the manual lacks Karl Popper’s criterion of “falsifiability”—the definitions are so broad and malleable that they cannot be proven wrong.48
Author of Mind Fixers, Harrington documents how the “biological revolution” of the 1980s was a narrative constructed to save psychiatry from irrelevance, not a result of scientific breakthrough. She argues the field “overreached,” promising biological cures (the “chemical imbalance” theory) without the science to back them up. She shows how DSM categories were often constructed to align with available pharmaceutical products rather than the drugs being developed to treat identified diseases.49
Author of Madness Explained, Bentall argues that “Schizophrenia” is a scientifically meaningless concept. It groups together people with vastly different symptoms (hallucinations vs. withdrawal) and outcomes who share no common biological marker. He notes that in DSM-5 field trials, the inter-rater reliability for schizophrenia was a “derisory” 0.46. He proposes abandoning the syndrome model entirely to study specific symptoms (e.g., “voice hearing”) which have distinct psychological mechanisms.50
The Ontological Critique: “Myth,” “Construct,” and “Meaning”
These critics argue that “mental illness” is a metaphor or social tool, not a medical fact.
Szasz is the grandfather of the critique. In The Myth of Mental Illness (1961), he argued that the mind is a concept, not an organ, and therefore cannot be “diseased” (lesioned). He contended that “mental illness” is a metaphor for “problems in living” (moral, social, or personal conflicts). He viewed the DSM as a tool of state control, using medical language to disguise the policing of social deviance. For Szasz, diagnosis is a “semantic blackjack” used to strip individuals of liberty and responsibility.7
In Madness and Civilization, Foucault argued that “madness” is a historical construct, not a scientific fact. He traced how the “medical gaze” of the modern era replaced the chains of the asylum with the invisible discipline of diagnosis. The DSM functions as a tool of biopower, regulating the population by categorizing non-conforming behaviors (e.g., lack of productivity) as “illness.” It silences the “unreason” of the mad by invalidating their speech as mere symptoms.51 The psychology of Foucault provides a crucial lens for deconstructing these power dynamics.
This group rejects the DSM’s assumption that hearing voices is always a symptom of pathology (Schizophrenia). They argue it is a meaningful human experience, often rooted in trauma or adverse life events. They contend that the DSM pathologizes their reality and distracts from understanding the meaning of the voices. They advocate for a “coping” model rather than a “curing” model that relies on suppression.52
Lead author of the Power Threat Meaning Framework (PTMF), Johnstone argues the DSM is a “failed paradigm” that should be abandoned. She contends that asking “What is wrong with you?” (diagnosis) is scientifically invalid. Instead, the PTMF asks: “What happened to you?” (Power), “How did it affect you?” (Threat), and “What sense did you make of it?” (Meaning). This framework replaces the “disease” model with a “meaning” model, linking distress directly to social determinants like poverty and abuse.53
The Political and Economic Critique
These critics focus on the external pressures—insurance, profit, and guild interests—that shape the manual.
Author of The Book of Woe, Greenberg embedded himself in the DSM-5 process to expose its “horse-trading.” He describes the DSM as a “book of billable codes”—a “noble lie” clinicians tell to get insurance coverage for patients. He reveals how the boundaries of illness are arbitrary statistical cutoffs designed to fit billing algorithms.45
Author of Cracked, Davies argues the DSM is a product of “guild interests”—expanding the manual expands the territory of psychiatry and its revenue. He interviewed task force members who admitted they had no scientific proof for where to draw the line between “normal” and “disorder.”46
Co-author of The Loss of Sadness, Horwitz argues the DSM systematically ignores context. By defining “Major Depression” purely by a symptom checklist, the DSM cannot distinguish between a biological disorder and “normal sadness” caused by a breakup or job loss. He argues this creates massive “false positives,” inflating prevalence rates and treating normal human sorrow as a medical disease requiring drugs.54
The Pediatric and Systemic Critique
These critics argue that diagnosis is used to absolve parents and schools of responsibility for the environments they create.
Timimi argues ADHD is a “cultural construct,” not a medical reality, noting there is no biomarker for the disorder. He argues the diagnosis serves a social function: it “exonerates” parents and schools. By labeling a distracted child as “diseased,” the school avoids changing its rigid curriculum, and parents avoid blame for family dysfunction. It repackages social problems as a biological defect in the child.55 Working with kids in therapy often reveals that the “symptom” is the child’s reaction to the system.
Author of The Body Keeps the Score, van der Kolk fought to include “Developmental Trauma Disorder” (DTD) in the DSM-5 to describe children with chronic abuse/neglect. The APA rejected it. He argues the DSM prefers to fragment these children into comorbidities (ADHD + Bipolar + ODD) because acknowledging trauma implicates the caregiving system. A biological label like “Bipolar” locates the problem in the child’s “broken brain,” effectively exonerating the parents and the social environment from their role in the child’s distress.56 (See: The Body Keeps the Score 2).
The Pharmaceutical Complex Critique
These critics focus on the corruption of the evidence base by the pharmaceutical industry.
Co-chair of Critical Psychiatry Network, Moncrieff’s 2022 systematic review debunked the “serotonin theory” of depression. She argues that because the biological justification (low serotonin) is false, the DSM categories based on it are invalid. She views psychiatric drugs not as “curing” a disease but as “inducing” an altered state (the “drug-centred model”). The DSM validates the prescription of these drugs by creating the illusion of a specific disease target.57
Author of Anatomy of an Epidemic, Whitaker argues that the DSM and the drugs it justifies are creating a chronic illness epidemic. He cites long-term data showing that medicated patients often have worse functional outcomes than unmedicated ones. He argues the “chemical imbalance” narrative was a marketing lie promoted by pharma and the APA to sell SSRIs and antipsychotics, transforming episodic distress into lifelong disability.58
Author of Deadly Psychiatry, Gøtzsche compares the pharmaceutical industry to “organized crime,” citing massive fraud settlements. He argues the DSM is a vehicle for “disease mongering”—widening diagnostic criteria to create new markets for drugs. He highlights the “organized denial” in psychiatry regarding the harms of drugs (suicide, brain shrinkage), maintained by the financial conflict of interest of DSM panel members (over 60% of whom have industry ties).59
Part X: Observations from the Clinical Trenches
In my time as a therapist and clinical director, I have seen growing hostility to the DSM. This is not merely an academic exercise for me—it is something I encounter daily in supervision, in training, and in the treatment room.
In training, I was shocked when some supervisors told me that diagnosis “didn’t matter because it was all wrong anyway.” These were veteran therapists with decades of experience, expressing deeply held grievances: CPTSD not being included (it remains in Section III), Reactive Attachment Disorder being so restrictive as to be useless, the removal of Asperger’s erasing an identity. These were shocking things to hear from respected clinicians early in my career, coming out of grad school where the document was treated with reverence as the thing that pointed us back to evidence-based practice.
The issues I have observed can be grouped into several patterns:
Diagnosis as Identity and Diagnosis as Meaningless
The DSM system has created a paradox where diagnosis is treated as both profoundly identity-defining and utterly meaningless at the same time.
A lot of people treat a diagnosis like a horoscope—or worse, an excuse to behave however they want. “I have ADHD, so I can’t help being late.” “I’m on the spectrum, so I can’t be expected to read social cues.” The diagnosis becomes an identity, a fixed thing that explains everything and excuses anything.
Other people cling to it and use it to define themselves entirely, organizing their whole self-concept around a diagnostic label they received at age 8 or 22. They join communities based on diagnosis, read about their disorder obsessively, and interpret every life experience through that lens. This often leads to a simulation of self rather than a true experience of selfhood.
Meanwhile, other therapists and patients have been diagnosed with so many different things over the course of their encounter with mental health that they no longer believe the diagnosis has any meaning. I’ve seen patients with charts containing ADHD, Bipolar II, Major Depression, Generalized Anxiety, PTSD, and Borderline Personality Disorder—diagnoses given weeks or months apart, often contradicting each other. At some point, the diagnostic process becomes a Rorschach test revealing more about the clinician than the patient.
The Misconception of Permanent Record
There also seems to be a pervasive belief among patients that diagnosis is a permanent thing that all clinicians have access to and follows you throughout your life. This isn’t really true. A diagnosis might go in your medical record at one health system, but that isn’t something every other organization has access to. The fragmentation of American healthcare means your psychiatrist, your therapist, your primary care doctor, and your hospital may all have different records with different diagnoses. This seems to be a pretty big misconception among patients, if not among therapists.
Part XI: The Tyranny of “Functional”—Why Suffering Should Matter More Than Productivity
One of the most destructive aspects of the DSM system is the “Clinical Significance Criterion”—the requirement that symptoms cause “clinically significant distress or impairment in social, occupational, or other important areas of functioning.” This criterion, introduced in DSM-IV as a gate against diagnostic inflation, has become a mechanism for denying care to people who are suffering immensely but still managing to function.
The Criterion That Excludes the Suffering
To combat the inflation caused by the checklists, Allen Frances and the DSM-IV task force introduced the “Clinical Significance Criterion.”30 The rule: to receive a diagnosis, the symptoms must cause “clinically significant distress or impairment in social, occupational, or other important areas of functioning.”
The intent was to create a gatekeeping mechanism—to prevent the “worried well” from being pathologized. A person could have all the symptoms of depression, but if they were still functioning at work, the “impairment” clause would theoretically block the diagnosis.
In practice, this criterion has become a tool for denying care to people who need it most.
The Problem: Psychology Exists to Treat Suffering, Not Optimize Productivity
There are many people who are suffering immensely who are failed by cognitive and behavioral therapy because they are “functioning well.” The DSM’s functional criterion betrays a fundamental confusion about what psychology is for.
The purpose of psychotherapy is not to prepare people to be better cogs and grease in a capitalist steam engine. It is not to optimize worker productivity. It is not to ensure that human beings continue to perform their economic functions despite their internal anguish.
The purpose of psychotherapy is to reduce suffering.
A person can be profoundly suffering—experiencing existential despair, disconnection from meaning, chronic emotional pain—while still maintaining their job, their relationships, their basic functioning. High-functioning depression, high-functioning anxiety, high-functioning trauma responses are real and common. These people often suffer more, not less, because they receive no external validation of their pain. They’re told, explicitly or implicitly, that because they can still perform, their suffering doesn’t count. This is often where we see functional freeze taking over.
The Functional Criterion Serves Capital, Not Patients
Who benefits from a diagnostic system that only recognizes suffering when it impairs productivity?
Insurance companies benefit. They don’t have to pay for treatment if the patient is still “functional.”
Employers benefit. They don’t have to accommodate workers whose suffering doesn’t affect output.
The economy benefits. Human beings continue to produce, regardless of their inner experience. (See: The Shadow Economy: Collective Repression and Financial Systems).
Who doesn’t benefit? The patient. The human being who is suffering but is told their suffering doesn’t count because they can still work.
This is not a neutral scientific criterion. It is an ideological choice—a choice that privileges productivity over wellbeing, function over experience, economic output over human flourishing. It reflects a vision of mental health as a maintenance system for labor capacity, not a practice of healing.
What Would a Humane Criterion Look Like?
A truly patient-centered diagnostic system would not ask: “Can you still work?” It would ask: “Are you suffering?”
If the answer is yes, that should be enough. Suffering is the indication for treatment. Not impairment. Not dysfunction. Not failure to meet productivity targets. Suffering.
Perhaps it’s better to just say that everyone deserves therapy, that therapy is a medical necessity for every human being. Because if we take that view, we can realize that everyone’s thought process could use improvement or a tune-up, and that you don’t have to be a “hurt puppy” to come to therapy. You don’t have to be broken. You don’t have to be failing. You just have to be a human being who wants to understand yourself better, suffer less, live more fully.
The DSM’s functional criterion is not science. It is ideology masquerading as science. And it is causing real harm to real people who are suffering but cannot access care because they are still productive enough to be denied it.
Part XII: Three Conceptual Failures of the DSM System
Beyond the historical and political problems, the DSM has several deep conceptual problems that make it fundamentally unsuited to the task of understanding human mental suffering.
Failure One: Not Treating These Things as Dynamic Systems
We know that the brain is mesh networks. We know that things like trauma and PTSD are reductive diagnoses because there are different types of trauma—somatic, narrative-based, re-experiencing—and a lot of the time they have nothing in common. To put them all in one diagnosis and then do a research study saying that something “treats PTSD” doesn’t really tell you any useful information.
What type of trauma, in what type of memory? Is it relational trauma with unfair expectations? Is it a shifting mood? Is it flashback re-experiences? In my experience as a therapist, you have to treat these things with completely different approaches and modalities. So knowing that a patient “has PTSD” doesn’t tell me where to look or what to do. That takes intuition and subjectivity that the checklist model seems to actively discourage.
Neuroscience and cognitive science are allowed to have conceptualizations of consciousness as competing drives and mesh networks. They’re allowed to understand these interoceptive processes that rise up from the body. So why is Blue Cross Blue Shield saying that treating them isn’t “evidence-based”? Why can’t psychotherapy have the same conceptual flexibility as the harder sciences that study the same organ?
Failure Two: The Absurd Belief That Checklists Make Psychology a Hard Science
At this point, you can look in the computer of any major medical system and see that any frequent flyer has hundreds of diagnoses, sometimes given weeks or days apart, that are completely different. You can follow any patient across their history and see how many different diagnoses they’ve accumulated.
We have to admit that the checklist system does not make psychotherapy more scientific, because psychiatrists still can’t agree on what you have. Either the model itself doesn’t work because the idea of clustering things into symptom buckets does not result in a uniform diagnosis when done properly—or we have to admit that American medicine itself is not structured in a way where it can diagnose as required by insurance, given the time constraints and systemic pressures. Maybe a little bit of both.
Either way, many clinicians and patients have started to find that the diagnosis system is absurd and that ultimately it just relies on whether or not the subjective intuition of the diagnoser is very good. That was the system that we started with—the one that DSM-III tried to move away from due to insecurity—but it seems to have not made the system any more scientific.
The problem with the checklist is that it’s based on the idea that we can do this stuff quickly. The reality of psychology is that we can’t. As a therapist, I often can’t tell the difference between trauma and low insight, because when someone’s nervous system is not regulated, they’re not at baseline. And you don’t know what their baseline is until you’ve known them a while. This is why tools like qEEG Brain Mapping can sometimes offer better insights than a checklist.
Failure Three: Contradicting Assumptions Sandwiched Together
The document itself has multiple contradicting assumptions. It often tries to pivot in one direction, but those pivots get held up in a committee that can’t agree on things, so we end up with incomplete visions and conflicting directions wrapped up into one document for clinicians to sit with.
The modern DSM essentially represents three competing assumptions sandwiched together that don’t work:
Table 7: Three Competing Assumptions in the Modern DSM
| Era | Operating Assumption | Still Present in DSM-5? |
|---|---|---|
| DSM-I/II (Dynamic) | Disorders are fluid processes, reactions to conflict | Vestigially, in some descriptive language |
| DSM-III/IV (Categorical) | Disorders are discrete entities with clear boundaries | Yes—the checklists remain the operational core |
| DSM-5 (Dimensional) | Disorders exist on spectrums with no clear boundaries | Nominally—the language is used, but the mechanics aren’t |
It’s three different things with competing operating assumptions that have been Dagwood-sandwiched together to suit the needs of what America needs mental health to be at any given point.
The proponents of the spectrum model noted that too many people would be pathologized if truly implemented—that normal behavior would become pathology and vast chunks of the country would suddenly have a mental illness. I’m not going to say that lots of people in this country have a mental illness, but I will say that lots of them probably have blind spots on how they’re thinking, neuroses and overreactions that cause suffering.
Perhaps it’s better to just say that everyone deserves therapy, that therapy is a medical necessity for every human being. Because of that, we have to realize that everyone’s thought process could use improvement or a tune-up, and that you don’t have to be a “hurt puppy” to come to therapy. We are all made up of mesh systems, and in this way we must go back to the understanding that the original founders of psychotherapy had: that these are dynamic processes that can be understood but can’t always be reduced to specific scientific objective things. Instead, they are lenses of understanding and modes of assumption that are sometimes useful and sometimes not.
Part XIII: The Divorce of Psychiatry and Therapy
Part of the issue is that psychiatrists used to do what I do. When you read Irvin Yalom—who was the gateway drug that brought a lot of people into the profession—he was a psychiatrist doing therapy for an hour before he prescribed medication. Psychiatrists and therapy used to share the same room, the same conversation, the same understanding of the patient.
If you meet a psychiatrist doing therapy today, they’re likely either independently wealthy or pushing 80. The economic realities of the profession have made it impossible. The insurance reimbursement for a 15-minute medication check vastly exceeds the hourly rate for therapy, when adjusted for time. So psychiatrists see patients for 10-15 minutes, ask about symptoms on a checklist, and prescribe or adjust medications. The therapeutic relationship—the thing that makes people better—has been severed from the prescribing authority.
If you find a psychiatrist in Birmingham who’s still doing therapy, they’re probably doing Ericksonian hypnosis or something similarly specialized, and they’re probably pushing 80. Those are the only ones I know.
Perhaps we need a different document for prescribing medication than we need for guiding therapy. Therapy might need different lenses than psychiatry. If you go back to a lot of the fights and feuds that happened during these DSM committees—granted, there are a lot of NDAs and we don’t know all the details—but if you look at the broad outlines, this is the fight: there’s medical psychopharmacology that wants one thing, and then there are people who want systems and environmental outlooks and therapeutic paradigms that psychiatry resists because it doesn’t help them prescribe drugs.
The DSM is very useful in clustering something like dopamine disorders together—conditions that likely share a very similar neurological route, share features, run in families, and are useful for prescribing medication. But in therapy, bipolar disorder, schizophrenia, and OCD are very different conditions that behave very differently based on the individual. You have psychiatrists who have never been in therapy and probably never done therapy now regulating how it is performed. Why?
Part XIV: The Neurodivergence Question—What Even Is Normal?
If you want to make spectrums, then how many Americans have ADHD? How many Americans are neurodivergent or have autism? Current estimates suggest that prevalence of diagnosed autism has risen to 1 in 36 children—a number that keeps climbing with each new survey.60 If we’re talking about features rather than diagnoses, the numbers are even higher.
If 30 or 40% of people are made to have features of ASD or ADHD, are they even “neurodivergent” then? Or is this just neuroreality? We are seeing the rise of concepts like AuDHD and monotropism to explain experiences that the DSM categorizes poorly. Perhaps what we’re discovering is not that more people are “disordered,” but that human cognitive diversity is far greater than the narrow band of “normal” the DSM has always assumed.
How many Americans have a personality disorder? How many Americans have undiagnosed PTSD? The numbers, depending on which studies you believe, are staggering. And if these conditions are this common, perhaps we should acknowledge that these are just systems—variations in how human minds organize themselves—rather than diseases to be treated. This is the core of neurodivergent-affirming therapy.
Part XV: The Insurance Straitjacket
Perhaps the most significant obstacle to a truly useful diagnostic system is not scientific but economic. The American mental health system is built on a foundation of categorical billing.
All psychiatric diagnoses in the US must map to codes in the International Classification of Diseases (ICD), maintained by the WHO. The ICD is a categorical system. A code represents a discrete entity. Insurance reimbursement operates on a binary logic: a condition is either present (medically necessary treatment) or absent (no coverage). A clinician cannot bill an insurance company for “75% Schizophrenia” or “Moderate Personality Dysfunction.” They must submit a specific code to get paid.61
This creates profound ethical and practical dilemmas for clinicians. A therapist treating a client with sub-threshold distress (who would exist on a “spectrum” but fails the “checklist”) often has to “upcode”—diagnose a more severe disorder than is present—to ensure the client can afford therapy.62
Because the financial engine of psychiatry requires discrete codes, the “spectrum” remains a theoretical overlay. Clinicians are forced to force-fit dimensional patients into categorical codes, rendering the nuances of the “spectrum” invisible to the administrative healthcare system.
At this point, the DSM exists exclusively because of insurance companies. But why do we give an insurance company so much power over what science is supposed to be determining for us? We have to pick science or we have to pick the profit motive. You can’t have both. They point in different directions. (See: The Hidden Economics of Healthcare).
Part XVI: A Way Forward—Narrative, Systems, and Clinical Intuition
I am writing this at a time when “experts” are trying to punish and lecture people for not following the science, for falling prey to TikTok influencers instead of seeking proper mental health care. But we have to ask ourselves, as therapists: why are people doing that?
Are we any more scientific than a wellness influencer? Or are we just another cult with better credentials? We’ve seen diminishing outcomes from following the evidence-based practice that the DSM claims. The STAR*D study—the most comprehensive taxpayer-funded study of depression treatment—claimed that 67% of patients would achieve remission through the recommended protocol of CBT and medication cycling. A forensic reanalysis revealed the true sustained recovery rate was 2.7%.63
2.7%
The actual sustained recovery rate from the STAR*D study, after forensic reanalysis—down from the claimed 67%.
If you’re doing heart surgery or cancer treatment and you have a failure rate of 97.3%, it would be national news. Yet the study that guided American psychiatry for over a decade is revealed to be essentially worthless, and no one talks about it.
There is an unhealthy attitude that because pseudoscience is becoming rampant in the mental health space, anybody who criticizes or cleaves from the DSM model must also be a pseudo-scientist. But that isn’t true. Both things can be wrong. We don’t have to find a middle ground between the DSM and somebody doing crystal healing on TikTok. We can point out things that don’t work with both models.
And before somebody tells me how hard they worked to get their PhD, or how much they care, or how much good they do—remember that cult leaders think that too. People put enormous work into belief structures that are not tied to science. They believe things because they’ve believed them for a long time. They believe things because they are traditions that are old. They believe things because they’ve put a lot of thinking and process around seeing reality through a certain lens. Academia is not an exception to this any more than a TikTok influencer is.
The Alternative: HiTOP and Dimensional Reality
If the DSM-5 represents a “nominal” spectrum, the “real” spectrum resides in the Hierarchical Taxonomy of Psychopathology (HiTOP).64
HiTOP is an alternative nosology constructed purely from factor analysis of symptom correlations, rather than committee voting. It ignores the historical boundaries of the DSM and looks at how symptoms naturally cluster in large populations. HiTOP reveals that psychopathology is structured hierarchically:
The “p-factor”: A general factor of psychopathology (like the “g-factor” in intelligence) representing overall susceptibility to mental illness.
Spectra: Broad dimensions such as Internalizing (Anxiety, Depression), Externalizing (Antisocial, Substance Use), and Thought Disorder (Psychosis).
HiTOP explains “comorbidity” not as having two diseases, but as having a high score on a single dimension. A person with “Social Anxiety” and “Depression” is simply scoring high on the “Internalizing” spectrum. This model has superior reliability and validity compared to the DSM.65
However, HiTOP faces the same administrative barrier as the AMPD: it lacks a billing interface. There are no ICD codes for “High Internalizing Score.” Until the legal and financial infrastructure of medicine changes, HiTOP will likely remain a research tool, while the DSM “checklist” remains the clinical law.
What Needs to Change
If we want to stop the exodus of patients to wellness influencers and want to heal the split between research and practice, we need structural change. We can’t just hope for better insurance reimbursement. We need to change what we consider valid science.
First, we have to re-legitimize the subjective. Get rid of checklists as the sole arbiter of diagnosis and understand these things as processes. When I have to do SEO for my website, the worst thing I can do is treat it as a checklist: “What are the top 10 things I have to do? Check, check, check.” Because it doesn’t work. You have to understand these things as parts of a system that are balancing each other out, that have trade-offs, that have effects on each other. The human mind works like that too.
Second, we need to replace quantitative dominance with qualitative study. We need journals that publish rigorous, detailed accounts of what actually happens in the room when a patient gets better. We need to look at the people who are effective therapists and see what they’re doing.
Third, we need to build open-source repositories for clinical observation. Currently, the wisdom of the field is locked behind profit paywalls or lost in the private notes of isolated therapists. We need a Wikipedia of clinical practice where thousands of clinicians can document what they’re seeing in real time. If 10,000 therapists report that semantic processing helps complex trauma, that is data that rivals any randomized controlled trial—because it’s somebody who did it yesterday, not a therapy that somebody invented 10 years ago that only now is being researched.
Fourth, we need to teach philosophy, narrative, and neuroscience in graduate schools. Add anthropology while we’re at it. We’re talking about polyvagal theory and half the people don’t know what these words mean because they don’t know how the brain works. We are training technicians when we should be training healers. A therapist who knows how to read a spreadsheet but doesn’t know how to understand a story is useless to human beings in crisis.
Fifth, and most importantly, we need to replace the functional criterion with a suffering criterion. Psychology should exist to reduce human suffering, not to optimize human productivity. If someone is suffering, they deserve treatment—regardless of whether they can still show up to work.
Science Is a Story
The path forward is not about choosing between science and narrative. It’s about realizing that science is a narrative. It is the grandest and most complex and most rigorous story that we have ever tried to tell. I don’t want to attack it. I want to help it tell its story better.
We often treat mathematics as if it were the bedrock of reality itself—as if the real stuff were numbers. But numbers represent reality; they are the mirror, not the thing. The thing speaks for itself. Numbers are a way of recording it imperfectly. A p-value is not a piece of the universe like a rock or a proton.
Theodore Porter, in Trust in Numbers, reminds us that we reach for these mirrors when we do not trust our own eyes.66 But the mirror is useless without someone to look into it and interpret the reflection. Data by itself is pointless—a pile of bricks without an architect. It requires interpretation to become meaning. And interpretation is fundamentally a narrative act.
When we try to make a purely objective study, we’re still telling a story. We’re still saying “these numbers represent this phenomenon.” The problem with the STAR*D study was not the data—the data was fine. It was the interpretation, because the numbers told a story you’re not allowed to tell anymore: the system did not work.
The story that science forgot is the story of science itself. It is the story of how inquiry emerged from human communities trying to understand their world. We can recover that story. We can rebuild the connections that the academic silos have severed.
If we do not offer therapy that is human and narrative and deeply relational, we will continue to lose our patients to those who do—even if what they are offering is a lie.
Reviewing the History:
Ultimately, a historical comparative analysis suggests that DSM-III, despite its reductive flaws, may have been superior to its successors simply because it represented a consistent, unified methodological attempt to resolve the crisis of reliability. While DSM-I and DSM-II were severely limited by the scientific vacuum of their time and plagued by significant social justice failures—specifically the lack of a systems or ‘person-in-environment’ perspective and a rigid ‘normalcy assumption’—they possessed a theoretical coherence regarding human dynamics that was arguably superior to the checklist model. The tragedy of the DSM-5 lies in its bifurcation; had the dimensionally robust models relegated to Section III (the appendix) been integrated into the main text, it might have represented the pinnacle of psychiatric nosology. Instead, the manual has become epistemic shrapnel, so fragmented that it arguably defies a singular critique. The field has become as scattered as modern psychoanalysis, containing internal contradictions that betray its own foundational assumptions. As the late critic Frederick Crews might have argued, when a discipline fractures this profoundly, one must question whether it should retain its original name or be reconstituted entirely.
The trajectory of the DSM reflects a fundamental loss of singular vision. The DSM-III, for all its reductive faults, possessed a coherence imposed by the Steve Jobs-like figure of Robert Spitzer, who dictated a unified direction to save the profession from irrelevance. In stark contrast, the DSM-5 and its successors are products of competing committee visions, resembling the design-by-committee failures of the corporate world rather than a streamlined scientific instrument. This decentralized process has resulted in a document that conceptually tears itself apart, failing to point downwards to a “why” (etiology) or upwards to a “how” (treatment).
The DSM-5 essentially represents a “hung jury.”[] Lacking a consensus on the biological nature of mental illness, the committees produced a manual that is less a verdict on reality than a compromise of factions. Rather than returning to the “trial” of scientific inquiry until a clear answer (validity) emerged, the field pushed forward with publication. This rush was driven not by scientific discovery but by the structural and financial imperatives of the APA—to publish the book that pays for the committee that failed to write the book the field actually needed.
The reluctance to embrace “operating assumptions” or subjective spaces in psychology has created a paradox. The field avoids subjective discovery because it feels “pseudoscientific” without hard data, yet it lacks the hard data to validate anything else. Neuroscience and cognitive science offer potential answers, but the DSM committees frequently reject these inputs for lacking “hard data” to prove them 100% correct, ignoring that discovery often requires navigating subjective spaces before objective validation is possible. By fearing the subjective and demanding premature objective certainty, the DSM has forgotten that data is for validation, not discovery. You must pick a direction to test if you are going in the right one; the current DSM, fragmented and frozen, has ceased to move.
In summary, the field has not truly committed to and realized a spectrum approach. It has applied a “spectrum” veneer over a “checklist” chassis. The engine of diagnosis—the binary decision to treat and bill—remains unchanged from the days of DSM-III. The “spectrum” is, for now, a promise unkept, waiting for a healthcare system that can accommodate the complex, fluid reality of human mental health.
Bibliography
- American Psychiatric Association. (1952). Diagnostic and Statistical Manual of Mental Disorders (1st ed.). Washington, DC: American Psychiatric Association. https://www.psychiatry.org/psychiatrists/practice/dsm
- Grob, G. N. (1991). Origins of DSM-I: A study in appearance and reality. American Journal of Psychiatry, 148(4), 421-431. https://pubmed.ncbi.nlm.nih.gov/2006685/
- Kirk, S. A., & Kutchins, H. (1992). The Selling of DSM: The Rhetoric of Science in Psychiatry. New York: Aldine de Gruyter. https://www.routledge.com/The-Selling-of-DSM
- Cooper, J. E., et al. (1972). Psychiatric Diagnosis in New York and London: A Comparative Study of Mental Hospital Admissions. London: Oxford University Press. https://pubmed.ncbi.nlm.nih.gov/4555792/
- Laing, R. D. (1960). The Divided Self: An Existential Study in Sanity and Madness. London: Penguin Books. https://www.penguinrandomhouse.com/books/321775/the-divided-self
- Laing, R. D., & Esterson, A. (1964). Sanity, Madness and the Family. London: Tavistock Publications. https://www.routledge.com/Sanity-Madness-and-the-Family
- Szasz, T. S. (1961). The Myth of Mental Illness: Foundations of a Theory of Personal Conduct. New York: Harper & Row. https://www.harpercollins.com/products/the-myth-of-mental-illness
- Szasz, T. S. (1970). The Manufacture of Madness: A Comparative Study of the Inquisition and the Mental Health Movement. New York: Harper & Row. https://www.amazon.com/Manufacture-Madness
- Szasz, T. S. (1963). Law, Liberty, and Psychiatry: An Inquiry into the Social Uses of Mental Health Practices. New York: Macmillan. https://www.amazon.com/Law-Liberty-Psychiatry
- Rosenhan, D. L. (1973). On being sane in insane places. Science, 179(4070), 250-258. https://doi.org/10.1126/science.179.4070.250
- Rosenhan, D. L. (1973). On being sane in insane places. Science, 179(4070), 250-258. [Detailed methodology section] https://www.science.org/doi/10.1126/science.179.4070.250
- Rosenhan, D. L. (1973). On being sane in insane places. [Staff behavior observations] Science, 179(4070), 250-258. https://pubmed.ncbi.nlm.nih.gov/4683124/
- Cahalan, S. (2019). The Great Pretender: The Undercover Mission That Changed Our Understanding of Madness. New York: Grand Central Publishing. https://www.grandcentralpublishing.com/titles/susannah-cahalan/the-great-pretender
- Decker, H. S. (2013). The Making of DSM-III: A Diagnostic Manual’s Conquest of American Psychiatry. Oxford: Oxford University Press. https://global.oup.com/academic/product/the-making-of-dsm-iii
- Spiegel, A. (2005). The Dictionary of Disorder: How one man revolutionized psychiatry. The New Yorker. https://www.newyorker.com/magazine/2005/01/03/the-dictionary-of-disorder
- Mayes, R., & Horwitz, A. V. (2005). DSM-III and the revolution in the classification of mental illness. Journal of the History of the Behavioral Sciences, 41(3), 249-267. https://doi.org/10.1002/jhbs.20103
- American Psychiatric Association. (1980). Diagnostic and Statistical Manual of Mental Disorders (3rd ed.). Washington, DC: American Psychiatric Association. https://www.psychiatry.org/psychiatrists/practice/dsm/history-of-the-dsm
- Feighner, J. P., et al. (1972). Diagnostic criteria for use in psychiatric research. Archives of General Psychiatry, 26(1), 57-63. https://pubmed.ncbi.nlm.nih.gov/5009428/
- Spitzer, R. L., Fleiss, J. L., & Endicott, J. (1978). Problems of classification: reliability and validity. In Psychopharmacology: A Generation of Progress. New York: Raven Press. https://pubmed.ncbi.nlm.nih.gov/619287/
- Kirk, S. A., & Kutchins, H. (1994). The myth of the reliability of DSM. Journal of Mind and Behavior, 15(1-2), 71-86. https://www.jstor.org/stable/43854063
- Hyman, S. E. (2010). The diagnosis of mental disorders: the problem of reification. Annual Review of Clinical Psychology, 6, 155-179. https://doi.org/10.1146/annurev.clinpsy.3.022806.091532
- Cosgrove, L., & Krimsky, S. (2012). A comparison of DSM-IV and DSM-5 panel members’ financial associations with industry. PLOS Medicine, 9(3), e1001190. https://doi.org/10.1371/journal.pmed.1001190
- Shorter, E. (1997). A History of Psychiatry: From the Era of the Asylum to the Age of Prozac. New York: John Wiley & Sons. https://www.wiley.com/A+History+of+Psychiatry
- Healy, D. (2004). Let Them Eat Prozac: The Unhealthy Relationship Between the Pharmaceutical Industry and Depression. New York: NYU Press. https://nyupress.org/let-them-eat-prozac
- Andreasen, N. C. (2007). DSM and the death of phenomenology in America: An example of unintended consequences. Schizophrenia Bulletin, 33(1), 108-112. https://doi.org/10.1093/schbul/sbl054
- Krueger, R. F., & Markon, K. E. (2006). Reinterpreting comorbidity: A model-based approach to understanding and classifying psychopathology. Annual Review of Clinical Psychology, 2, 111-133. https://doi.org/10.1146/annurev.clinpsy.2.022305.095213
- Volkmar, F. R., & McPartland, J. C. (2014). From Kanner to DSM-5: Autism as an evolving diagnostic concept. Annual Review of Clinical Psychology, 10, 193-212. https://doi.org/10.1146/annurev-clinpsy-032813-153710
- Frances, A. (2013). Saving Normal: An Insider’s Revolt Against Out-of-Control Psychiatric Diagnosis, DSM-5, Big Pharma, and the Medicalization of Ordinary Life. New York: William Morrow. https://www.harpercollins.com/products/saving-normal
- Frances, A. (2009). A warning sign on the road to DSM-V: Beware of its unintended consequences. Psychiatric Times, 26(8). https://www.psychiatrictimes.com/view/warning-sign-road-dsm-v
- Spitzer, R. L., & Wakefield, J. C. (1999). DSM-IV diagnostic criterion for clinical significance: Does it help solve the false positives problem? American Journal of Psychiatry, 156(12), 1856-1864. https://pubmed.ncbi.nlm.nih.gov/10588397/
- Regier, D. A., et al. (2009). DSM-5 field trials in the United States and Canada, Part II: Test-retest reliability of selected categorical diagnoses. American Journal of Psychiatry, 170(1), 59-70. https://doi.org/10.1176/appi.ajp.2012.12070999
- Kupfer, D. J., & Regier, D. A. (2011). Neuroscience, clinical evidence, and the future of psychiatric classification in DSM-5. American Journal of Psychiatry, 168(7), 672-674. https://doi.org/10.1176/appi.ajp.2011.11020219
- Paris, J. (2015). The Intelligent Clinician’s Guide to the DSM-5. Oxford: Oxford University Press. https://global.oup.com/academic/product/the-intelligent-clinicians-guide-to-the-dsm-5
- Lord, C., et al. (2012). A multisite study of the clinical diagnosis of different autism spectrum disorders. Archives of General Psychiatry, 69(3), 306-313. https://doi.org/10.1001/archgenpsychiatry.2011.148
- Maenner, M. J., et al. (2014). Potential impact of DSM-5 criteria on autism spectrum disorder prevalence estimates. JAMA Psychiatry, 71(3), 292-300. https://doi.org/10.1001/jamapsychiatry.2013.3893
- Kulage, K. M., et al. (2014). How will DSM-5 affect autism diagnosis? A systematic literature review and meta-analysis. Journal of Autism and Developmental Disorders, 44(8), 1918-1932. https://doi.org/10.1007/s10803-014-2065-2
- Tandon, R. (2014). Schizophrenia and other psychotic disorders in DSM-5. Clinical Schizophrenia & Related Psychoses, 7(1), 16-19. https://doi.org/10.3371/CSRP.TA.032513
- Yung, A. R., et al. (2012). Whither the attenuated psychosis syndrome? Schizophrenia Bulletin, 38(6), 1130-1134. https://doi.org/10.1093/schbul/sbs108
- Carpenter, W. T. (2009). Anticipating DSM-V: Should psychosis risk become a diagnostic class? Schizophrenia Bulletin, 35(5), 841-843. https://doi.org/10.1093/schbul/sbp071
- Skodol, A. E. (2012). Personality disorders in DSM-5. Annual Review of Clinical Psychology, 8, 317-344. https://doi.org/10.1146/annurev-clinpsy-032511-143131
- Krueger, R. F., et al. (2012). Initial construction of a maladaptive personality trait model and inventory for DSM-5. Psychological Medicine, 42(9), 1879-1890. https://doi.org/10.1017/S0033291711002674
- Morey, L. C., et al. (2014). Personality disorder assessment, the challenge of construct validity, and DSM-5. Journal of Personality Assessment, 96(1), 37-44. https://doi.org/10.1080/00223891.2013.823438
- Insel, T. (2013). Director’s Blog: Transforming Diagnosis. National Institute of Mental Health. https://www.nimh.nih.gov/about/directors/thomas-insel/blog/2013/transforming-diagnosis
- Cuthbert, B. N., & Insel, T. R. (2013). Toward the future of psychiatric diagnosis: The seven pillars of RDoC. BMC Medicine, 11, 126. https://doi.org/10.1186/1741-7015-11-126
- Greenberg, G. (2013). The Book of Woe: The DSM and the Unmaking of Psychiatry. New York: Blue Rider Press. https://www.penguinrandomhouse.com/books/212374/the-book-of-woe
- Davies, J. (2013). Cracked: Why Psychiatry is Doing More Harm than Good. London: Icon Books. https://iconbooks.com/ib-title/cracked/
- Whooley, O. (2019). On the Heels of Ignorance: Psychiatry and the Politics of Not Knowing. Chicago: University of Chicago Press. https://press.uchicago.edu/ucp/books/book/chicago/O/bo35854313.html
- Ghaemi, S. N. (2009). The Rise and Fall of the Biopsychosocial Model: Reconciling Art and Science in Psychiatry. Baltimore: Johns Hopkins University Press. https://www.press.jhu.edu/books/title/9754/rise-and-fall-biopsychosocial-model
- Harrington, A. (2019). Mind Fixers: Psychiatry’s Troubled Search for the Biology of Mental Illness. New York: W.W. Norton. https://wwnorton.com/books/Mind-Fixers/
- Bentall, R. P. (2004). Madness Explained: Psychosis and Human Nature. London: Penguin Books. https://www.penguin.co.uk/books/26888/madness-explained
- Foucault, M. (1961). Madness and Civilization: A History of Insanity in the Age of Reason. Paris: Plon. English translation (1965). New York: Pantheon. https://www.penguinrandomhouse.com/books/55370/madness-and-civilization
- Corstens, D., Longden, E., McCarthy-Jones, S., Waddingham, R., & Thomas, N. (2014). Emerging perspectives from the Hearing Voices Movement: Implications for research and practice. Schizophrenia Bulletin, 40(Suppl 4), S285-S294. https://doi.org/10.1093/schbul/sbu007
- Johnstone, L., & Boyle, M. (2018). The Power Threat Meaning Framework: Towards the identification of patterns in emotional distress, unusual experiences and troubled or troubling behaviour, as an alternative to functional psychiatric diagnosis. Leicester: British Psychological Society. https://www.bps.org.uk/power-threat-meaning-framework
- Horwitz, A. V., & Wakefield, J. C. (2007). The Loss of Sadness: How Psychiatry Transformed Normal Sorrow into Depressive Disorder. Oxford: Oxford University Press. https://global.oup.com/academic/product/the-loss-of-sadness
- Timimi, S. (2017). Non-diagnostic based approaches to helping children who could be labelled ADHD and their families. International Journal of Qualitative Studies on Health and Well-being, 12(sup1), 1298270. https://doi.org/10.1080/17482631.2017.1298270
- van der Kolk, B. A., et al. (2005). Disorders of extreme stress: The empirical foundation of a complex adaptation to trauma. Journal of Traumatic Stress, 18(5), 389-399. https://doi.org/10.1002/jts.20047
- Moncrieff, J., et al. (2022). The serotonin theory of depression: A systematic umbrella review of the evidence. Molecular Psychiatry. https://doi.org/10.1038/s41380-022-01661-0
- Whitaker, R. (2010). Anatomy of an Epidemic: Magic Bullets, Psychiatric Drugs, and the Astonishing Rise of Mental Illness in America. New York: Crown. https://www.penguinrandomhouse.com/books/301770/anatomy-of-an-epidemic
- Gøtzsche, P. C. (2015). Deadly Psychiatry and Organised Denial. Copenhagen: People’s Press. https://www.deadlymedicines.dk/books/deadly-psychiatry
- Maenner, M. J., et al. (2023). Prevalence and characteristics of autism spectrum disorder among children aged 8 years—Autism and Developmental Disabilities Monitoring Network, 11 sites, United States, 2020. MMWR Surveillance Summaries, 72(2), 1-14. https://doi.org/10.15585/mmwr.ss7202a1
- World Health Organization. (2019). International Classification of Diseases, 11th Revision (ICD-11). Geneva: World Health Organization. https://icd.who.int/en
- Zimmerman, M. (2003). What should the standard of care for psychiatric diagnostic evaluations be? The Journal of Nervous and Mental Disease, 191(5), 281-286. https://pubmed.ncbi.nlm.nih.gov/12819546/
- Pigott, H. E., et al. (2010). Efficacy and effectiveness of antidepressants: Current status of research. Psychotherapy and Psychosomatics, 79(5), 267-279. https://doi.org/10.1159/000318293
- Kotov, R., et al. (2017). The Hierarchical Taxonomy of Psychopathology (HiTOP): A dimensional alternative to traditional nosologies. Journal of Abnormal Psychology, 126(4), 454-477. https://doi.org/10.1037/abn0000258
- Caspi, A., et al. (2014). The p factor: One general psychopathology factor in the structure of psychiatric disorders? Clinical Psychological Science, 2(2), 119-137. https://doi.org/10.1177/2167702613497473
- Porter, T. M. (1995). Trust in Numbers: The Pursuit of Objectivity in Science and Public Life. Princeton: Princeton University Press. https://press.princeton.edu/books/paperback/9780691029085/trust-in-numbers
- Goodwin, F. K., & Jamison, K. R. (2007). Manic-Depressive Illness: Bipolar Disorders and Recurrent Depression (2nd ed.). Oxford: Oxford University Press. https://global.oup.com/academic/product/manic-depressive-illness
- Grinker, R. R. (2007). Unstrange Minds: Remapping the World of Autism. New York: Basic Books. https://www.basicbooks.com/titles/roy-richard-grinker/unstrange-minds
- Aviram, R. B., Brodsky, B. S., & Stanley, B. (2006). Borderline personality disorder, stigma, and treatment implications. Harvard Review of Psychiatry, 14(5), 249-256. https://doi.org/10.1080/10673220600975121
Joel Blackstock, LICSW-S, is the Clinical Director of Taproot Therapy Collective in Hoover, Alabama. He specializes in complex trauma treatment and writes at GetTherapyBirmingham.com.









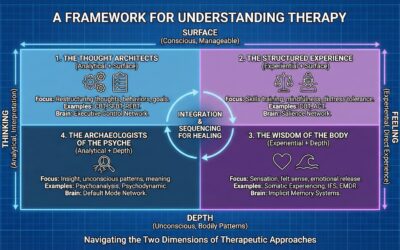















0 Comments