For decades, psychiatry operated on the belief that the brain was a fortress, completely isolated from the rest of the body by the blood-brain barrier. If you were depressed, it was a “chemical imbalance” in your head. If you were anxious, it was a firing error in your amygdala. But a revolution in modern neuroscience has shattered this isolationist view. We now know that the brain is intimately connected to the gut, the immune system, and the body’s inflammatory response. This connection is so strong that many researchers are now asking a radical question: Is depression actually an allergic reaction to inflammation?
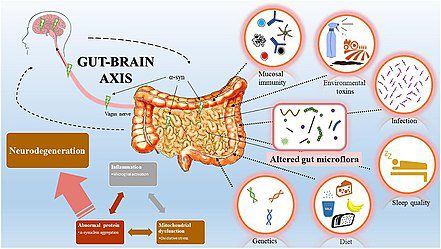
The “Gut-Brain Axis” is the bi-directional communication highway between your central nervous system and your enteric nervous system (the “second brain” in your gut). This highway is paved with the Vagus Nerve, but it is trafficked by immune cells and neurotransmitters. In fact, 95% of your body’s serotonin—the “happy chemical” targeted by antidepressants—is produced in your intestines, not your brain. This means that what you eat doesn’t just fuel your body; it builds your mood. When we consume highly inflammatory foods, we aren’t just bloating our bellies; we are inflaming our brains.
The Mechanism: How Inflammation “Slows” the Brain
When the body detects an intruder (like a virus or a toxin), it launches an inflammatory response to kill it. This is healthy in the short term. But when inflammation becomes chronic—due to stress, poor diet, or environmental toxins—it crosses the blood-brain barrier. Once in the brain, inflammatory cytokines attack the microglia (the brain’s immune cells). This triggers a state called “Sickness Behavior.”
Think about the last time you had the flu. You felt tired, unmotivated, foggy, and you wanted to withdraw from people. Evolutionarily, this is smart; your body is forcing you to rest so it can heal. But chronic inflammation tricks the brain into being “permanently sick.” You feel the lethargy, the brain fog, and the social withdrawal of the flu, but without the fever. We call this “Clinical Depression.” This is why traditional talk therapy sometimes fails; you cannot talk a brain out of being inflamed any more than you can talk a knee out of being swollen.
The Culprits: Gluten, Sugar, and the Leaky Gut
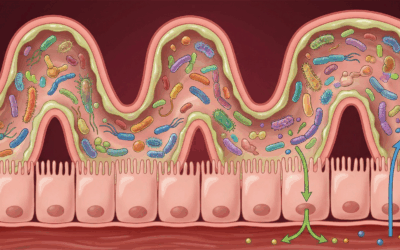
While every body is different, certain foods are notorious for triggering this systemic inflammation. Gluten is a primary suspect. For sensitive individuals, gluten triggers the release of zonulin, a protein that opens the tight junctions of the gut lining. This “Leaky Gut” allows undigested food particles and bacteria to escape into the bloodstream, putting the immune system on high alert. The result? A systemic fire that manifests as anxiety, irritability, and the classic “brain fog.”
Sugar is the other major offender. High sugar intake spikes insulin and feeds harmful gut bacteria (dysbiosis), which crowd out the beneficial bacteria responsible for making GABA and dopamine. This creates a rollercoaster of energy crashes and mood swings that mimics—and exacerbates—anxiety disorders and ADHD.
The Antidote: Feeding the Brain
The good news is that if food is the poison, food is also the medicine. By switching to an anti-inflammatory diet, you can often lift the “fog” in a matter of weeks. This is the foundation of Nutritional Psychiatry.
1. Heal the Gut Lining
To stop the inflammation, you must close the gates. Collagen-rich foods like bone broth, along with supplements like L-Glutamine, can help repair the gut wall. Removing irritants like gluten and processed seed oils is the first step to letting the fire die down.
2. The “Big Three” Micronutrients
Most mental health struggles are worsened by specific deficiencies:
- Vitamin B12 & Folate: Essential for methylation, the process that makes neurotransmitters. A deficiency here mimics severe depression and paranoia.
- Zinc: Critical for regulating the stress response. Low zinc is strongly linked to treatment-resistant depression.
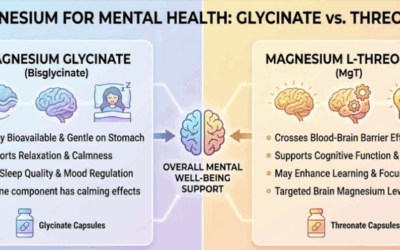
- Magnesium: The body’s “relaxant.” It blocks excess cortisol from damaging the brain. Most anxious people are severely magnesium deficient.
3. Omega-3 Fatty Acids
Your brain is 60% fat. It needs high-quality fats to build cell membranes that are flexible and receptive to serotonin. Omega-3s (found in fish oil, walnuts, and flax) are powerful anti-inflammatories that have been shown to rival antidepressants in some clinical trials.
Mental health is not just “all in your head.” It is in your stomach, your immune system, and your grocery cart. If you have been treating your depression solely as a psychological issue without success, it may be time to look at the physiological roots. At our clinic, we integrate holistic nutrition with psychotherapy because we know that you cannot build a healthy mind on an inflamed foundation.
Select Bibliography
- Perlmutter, D. (2013). Grain Brain: The Surprising Truth about Wheat, Carbs, and Sugar–Your Brain’s Silent Killers. Little, Brown Spark.
- Bullmore, E. (2018). The Inflamed Mind: A Radical New Approach to Depression. Picador.
- Mayer, E. (2016). The Mind-Gut Connection. Harper Wave.
- Naidoo, U. (2020). This Is Your Brain on Food. Little, Brown Spark.

















0 Comments