A Genealogical History of How External Forces Transformed the Therapy Patient—and Why It Matters Now More Than Ever
The history of psychotherapy is often told as a history of “great men”—Freud, Jung, Rogers, Beck—and their competing theories of mind. However, a more revealing history lies in the evolution of the person sitting across from them. The conceptualization of the patient has never been a static medical fact; it is a fluid cultural construct, shaped continuously by the interplay of language, economic imperatives, and the shifting resolution of the brain-mind problem.
Over the last century, the entity seeking help has undergone a profound ontological transformation. They began in the early 20th century as the Neurotic, a tragically conflicted soul whose suffering was an index of depth, requiring what the early analysts called a “cure of souls” through insight. In the post-war optimism of the 1950s, they became the Client, a democratic citizen engaged in a project of self-actualization. By the 1980s, under the twin pressures of the biological revolution and the insurance industry, they were re-engineered into a Patient with a Disorder, a biological machine suffering from a “broken part” or chemical imbalance. In the contemporary digital era, this figure has morphed yet again into the User—a consumer of on-demand mental health content, navigating an algorithmic marketplace of commodified care.
This article traces this evolution decade by decade. It argues that the “progress” of the field has not been a linear march toward scientific truth, but rather—as I’ve written about in The Illusion of Progress: How Psychotherapy Lost Its Way—a series of adaptations to material forces: the rise of the pharmaceutical industry, the dominance of managed care, and what we might call the “uberization” of the gig economy. Furthermore, it examines the current counter-movement: a resurgence of models that view the patient as a complex system of “underlying forces,” such as Internal Family Systems and somatic trauma therapies, which seek to reclaim the interiority lost to the biomedical model.
The Age of the Neurotic (1900s–1930s)
The Architecture of Conflict
At the turn of the 20th century, the dominant conceptualization of the patient was defined by the nascent field of psychoanalysis. The patient was a Neurotic. This term, while rooted in the 18th-century medical nosology of William Cullen, was radically repurposed by Sigmund Freud. For the early psychoanalysts, “neurosis” was not merely a nervous condition; it was a structure of the personality.
The neurotic was conceptualized as a divided subject—a theater of war where a civil conflict raged between the biological drives of the id, the internalized moral prohibitions of the superego, and the mediating executive functions of the ego. In this model, the patient’s symptoms—whether the paralysis of a hysterical limb or the ritual of an obsessive thought—were not random biological glitches. They were symbols. They were the “compromise formations” of a psyche navigating the impossible demands of civilization.
The patient of this era possessed depth. Their suffering was intelligible only through excavation—what Jung would later call “shadow work.” The “cure” was not symptom removal—which Freud viewed as superficial and likely to lead to “symptom substitution”—but insight. The mechanism of change was the making conscious of the unconscious, allowing the ego to reclaim territory from the id.
Divergent Views Among the Founders
While Freud emphasized the sexual and aggressive drives as the bedrock of the neurotic’s struggle, his contemporaries offered nuances that would echo for decades. Alfred Adler re-conceptualized the neurotic not as a victim of drive conflict but as a discouraged social actor. For Adler, the patient was defined by their “style of life” and the presence or absence of Gemeinschaftsgefühl (social interest). The neurotic was characterized by egocentricity and a “mistaken” striving for superiority to compensate for feelings of inferiority.
Carl Jung expanded the patient’s interiority even further, viewing the neurotic symptom not just as a pathological failure but as a thwarted attempt at individuation. For Jung, the patient was a spiritual seeker whose neurosis was a “calling” to integrate the shadow and the collective unconscious.
Despite these differences, all three conceptualized the patient as a being of profound complexity, whose current state was determined by a personal history of “underlying forces” that had to be understood, not merely managed. This is a crucial distinction that we have largely abandoned—to our patients’ detriment.
The Brain-Mind Problem: The Psychic Triumph
In this era, the brain-mind problem was resolved decisively in favor of the Mind. While Freud began as a neurologist and always believed that a biological substrate existed, he concluded that the technology of the time was insufficient to map the mind to the brain. Therefore, the “psychological” was granted autonomy. The patient’s problem was a “software” problem, not a “hardware” problem. This allowed for a conceptualization of the patient that was deeply humanistic and literary, rather than medical and mechanistic.
Material Forces: The Economics of the Private Cure
The material conditions of the early 20th century were essential to this conceptualization. Psychotherapy was an unregulated, cash-based private enterprise. The “patient” was typically drawn from the educated urban bourgeoisie—those with the time and resources to engage in an analysis that could last years, with sessions occurring four to six times a week.
There were no third-party payers—no insurance companies or government agencies—to demand efficiency, diagnosis, or “medical necessity.” The economic transaction was strictly dyadic: between the doctor and the patient. This financial independence allowed the definition of “neurosis” to remain broad and fluid. It could encompass everything from debilitating paralysis to vague existential malaise. There was no bureaucratic need to distinguish between the “worried well” and the “mentally ill,” because the state was not paying for the treatment. This era established the “long-term” model of care, where the relationship itself was the vehicle of transformation, shielded from the scrutiny of external auditors.
The Humanistic Revolt and the Birth of the “Client” (1940s–1950s)
From Patient to Person
In the wake of World War II, a revolution in nomenclature occurred that signaled a profound shift in power. Carl Rogers, a psychologist rather than a psychiatrist, challenged the medical hierarchy implicit in the term “patient.” He argued that “patient” denoted a passive, sick individual waiting to be cured by an expert. In his seminal works, Rogers introduced the term Client.
This was not merely a semantic adjustment; it was a political act. The “Client” was conceptualized as a person possessing an innate “actualizing tendency”—a biological drive toward growth, maturity, and autonomy. In the Rogerian view, the client was the expert on their own life. The therapist’s role was not to diagnose or interpret (as the analyst did) but to provide the “necessary and sufficient conditions”—empathy, congruence, and unconditional positive regard—for the client to heal themselves.
The Neo-Freudians and the Social Self
Simultaneously, the “Neo-Freudians” were reshaping the psychoanalytic view. While they often retained the term “patient,” they re-conceptualized the etiology of neurosis, moving away from Freud’s biological determinism toward a cultural and interpersonal model. Karen Horney argued that neurosis arose from “basic anxiety” caused by interpersonal isolation and helplessness in a hostile world, often stemming from parental indifference. Harry Stack Sullivan defined psychiatry as the study of interpersonal relations, arguing that the “self” is not a contained entity but a collection of “reflected appraisals” from others.
The patient of the 1950s, whether a “client” or a “social neurotic,” was an inherently relational being. Their pathology was located in the space between people, and the cure was a new kind of relationship.
The Behavioral Turn and the Erosion of Depth (1960s–1970s)
The Patient as Organism: The End of “Underlying Forces”
While the Humanists were celebrating the client’s potential, a starkly different conceptualization was emerging from the psychology laboratories: Behaviorism. Figures like B.F. Skinner and Joseph Wolpe attacked both the “unconscious” of the analysts and the “self” of the humanists as unscientific “black boxes.”
For the behaviorist, the patient was an Organism governed by the laws of learning. Pathology was not a symbol of deep conflict; it was simply a “maladaptive habit” acquired through conditioning. A phobia of cats was not a displacement of sexual fear; it was a conditioned response to a stimulus. The behaviorists argued that if you removed the symptom, you cured the neurosis, famously quipping that “neurosis is nothing but the symptoms.”
This marked a radical flattening of the patient. The dimension of depth—the idea that the surface symptom pointed to a deeper truth—was rejected. The patient was a machine that had learned the wrong program.
The Cognitive Revolution: The Patient as Computer
By the 1970s, strict behaviorism evolved into Cognitive Behavioral Therapy (CBT), pioneered by Aaron Beck. Beck, a disillusioned psychoanalyst, proposed that depression was caused not by “anger turned inward” (the Freudian view) but by “cognitive distortions”—systematic errors in information processing.
The patient was re-conceptualized as a Rational Agent with faulty logic. The mind was viewed through the metaphor of the computer (the dominant technology of the era): the hardware was fine, but the software (beliefs/schemas) was buggy. The therapeutic relationship shifted from a “transferential vessel” to “collaborative empiricism,” where therapist and patient worked like scientists to test the validity of the patient’s thoughts.
Material Forces: The Demand for Accountability
The rise of Behaviorism and CBT was not just an intellectual evolution; it was an adaptation to the changing marketplace. As third-party insurance began to cover mental health, payers became skeptical of open-ended “growth” therapies. They wanted results that could be measured. Behavior therapy offered quantifiable outcomes that psychoanalysis could not. This alignment with the “technocratic rationality” of the Cold War era gave these models a significant institutional advantage—an advantage that would only grow.
The Great Categorical Rupture (1980)
DSM-III and the Death of Neurosis
The year 1980 represents the most significant watershed in the history of patient conceptualization. The publication of the Diagnostic and Statistical Manual of Mental Disorders, Third Edition (DSM-III), revolutionized psychiatry. Led by Robert Spitzer and a “neo-Kraepelinian” task force, the DSM-III aimed to save psychiatry from “ideology” and establish “reliability.”
The most contested symbolic battle of this revolution was the removal of the term “Neurosis” from the nomenclature. For 80 years, “neurosis” had been the organizing principle of outpatient therapy. It implied a continuum between health and illness and pointed to a specific etiology: unconscious conflict. Spitzer and his colleagues argued that “neurosis” was a theoretical term, not a descriptive one. To make psychiatry “scientific” (and medical), diagnoses had to be based on “observable signs and symptoms,” not invisible causes. Despite fierce outcry from the psychoanalytic community, the term was excised.
The Patient as a Checklist
The “Neurotic” was replaced by the Patient with a Disorder. The patient was now defined by a categorical checklist: Do you have 5 of these 9 symptoms for at least two weeks? If yes, you “have” Major Depressive Disorder.
This shift had profound consequences:
- Reification: It turned fluid human suffering into static “things” (disorders) that one “has,” like a virus.
- Self-Estrangement: As Nancy McWilliams notes, this encouraged a disowning of the self. A patient says, “I have Social Anxiety Disorder,” rather than “I am a painfully shy person.” The diagnosis becomes an alien entity attacking the self, rather than a description of the self’s structure.
- Loss of Context: The “checklist” approach stripped the symptom of its context. It didn’t matter why you were depressed; if you met the criteria, you had the disorder.
Material Forces: The Needs of Pharma and Insurance
The DSM-III was not just scientific; it was a document of political economy. As I’ve explored in Is the Corporatization of Healthcare and Academia Ruining Psychotherapy?, the incentive structures of our field have been systematically corrupted by external economic forces.
The Pharmaceutical Imperative: The 1980s saw the rise of the blockbuster psychiatric drug industry. To gain FDA approval, companies needed homogenous patient populations for clinical trials. They needed to prove a drug worked for “Depression,” not for “neurotic misery.” The DSM-III provided the “cookie-cutter” categories that allowed Big Pharma to recruit subjects and market drugs like Prozac to specific “target” disorders.
The Insurance Mandate: Insurers needed a standardized language to process claims. They could not reject a claim for “neurosis” easily, as it was vague. But they could reject a claim if the patient didn’t meet the specific criteria for a DSM disorder. The manual became the codebook for reimbursement.
The Managed Care Era and the “Consumer” (1990s)
The Decade of the Brain and the Chemical Imbalance
In 1990, President George H.W. Bush signed a resolution declaring the 1990s the “Decade of the Brain.” This political act consecrated the biomedical model as the state religion of mental health. The National Institute of Mental Health (NIMH) fundamentally shifted its funding priorities. As former NIMH Director Thomas Insel later admitted, the agency spent billions on neuroscience and genetics, moving away from psychosocial research—and, as he conceded, the “needle” on mental health outcomes never moved.
The patient was re-conceptualized as a Biological Unit suffering from a “Chemical Imbalance.” Direct-to-consumer advertising bombarded the public with the message that “depression is a serious medical condition that may be caused by a chemical imbalance.” The patient was told that their suffering was a “deficiency” of serotonin, akin to a diabetic needing insulin. While recent comprehensive reviews have debunked the serotonin theory as scientifically unsubstantiated, its cultural power in the 1990s was absolute. It relieved the patient of “guilt” (it’s not your fault, it’s your biology) but also robbed them of agency (only a pill can fix it).
Managed Care: The Patient as “Covered Life”
Simultaneously, the rise of Managed Care Organizations (MCOs) transformed the economics of therapy. The patient became a “Covered Life,” and the therapist became a “Provider.” MCOs introduced the concept of “Medical Necessity” as a weapon of cost containment.
Under this regime, therapy was stripped of its explorative and relational dimensions. “Medical Necessity” meant that treatment was only authorized for the “restoration of function” and “symptom reduction.” Long-term therapy for personality change or “growth” was denied. The therapeutic dyad was broken. The insurance reviewer sat invisibly in the room, dictating the length of treatment (often 6-10 sessions) and demanding a diagnosis. Therapists were forced into ethical compromises, often “upcoding” a patient’s diagnosis to a more severe disorder just to get sessions authorized. The relationship was commodified. Time was money. The “Consumer” purchased a “Behavioral Health Product” aimed at a specific “Target Symptom.”
The “Evidence-Based” Battleground (2000s)
The Hegemony of CBT and the “Evidence-Based” Patient
By the 2000s, the “Evidence-Based Practice” (EBP) movement had consolidated control over academia and training. As I’ve written in Evidence Based Practice is Bul$*%!@, Let’s Fix It!, “evidence-based” became a code word for Manualized CBT. Because CBT is structured, uniform, and short-term, it fit perfectly into the randomized controlled trial (RCT) design favored by researchers.
A generation of clinical psychologists was trained in PhD programs where psychodynamic and humanistic approaches were marginalized or eliminated entirely. The patient was conceptualized as a recipient of a “Treatment Package.” The logic was medical: “For Disorder X, administer Protocol Y.”
The Critique: The Illusion of Efficacy
Major critics, most notably Jonathan Shedler, arose to challenge this paradigm. As detailed in When Evidence Based Practice Goes Wrong and The Failure of Evidence-Based Incentive Structure, the most damning example is the STAR*D scandal—the largest antidepressant trial in history, funded by the NIMH, which reported a 67% remission rate. Independent reanalysis revealed the actual remission rate was closer to 3%. The original investigators had conflicts of interest with pharmaceutical companies and employed statistically questionable methods that inflated their results.
Shedler argued that the “Evidence-Based” label was a marketing term that misrepresented the data:
- The Efficacy Myth: In the “gold standard” NIMH depression trials, the difference between CBT and placebo was often clinically meaningless. Furthermore, relapse rates for manualized treatments were high.
- The Exclusionary Fallacy: RCTs often excluded the majority of real-world patients—those with comorbidities, personality disorders, or complex trauma—meaning the “evidence” only applied to a narrow slice of the “easy” cases.
- The “Dodo Bird” Verdict: Shedler and others reiterated the robust finding that common factors (the alliance, empathy, the therapist’s skill) account for far more variance in outcome than the specific “technique” or “brand” of therapy. By focusing on the “protocol,” the field was ignoring the human.
Despite these critiques, the institutional inertia of insurance companies (who loved the short-term nature of CBT) and universities (who relied on NIH grants for “scientific” research) maintained the dominance of the protocol-based patient. As explored in Psychotherapy’s Feuding Founders, these tensions between schools are not new—but the material forces behind them have never been stronger.
The Uberization of Mental Health and the Dangers Ahead (2010s–Present)
The Gig Economy and the Patient as “User”
With the ubiquity of the smartphone, the conceptualization of the patient shifted to the User. As I warned in Corporate Tech Monopolies are Going to Ruin Therapy, platforms like BetterHelp and Talkspace disrupted the traditional private practice model, offering “therapy” via text and video on demand.
This represents the “Uberization” of mental health. The patient is a subscriber paying a monthly fee for “access.” The therapist is a gig worker, often paid by the word or the minute, responding to messages in fragmented bursts. The “User” is matched with a therapist not through a consultation process to determine relational fit, but by an algorithm based on checkbox preferences. This flattens the complex human encounter into a data-matching exercise.
The BetterHelp Scandal: When HIPAA Becomes Meaningless
The nightmare scenario that many predicted came to pass. In 2023, the Federal Trade Commission (FTC) took action against BetterHelp for sharing consumers’ sensitive health data—including information about mental health challenges—with advertising platforms like Facebook and Snapchat. The company had promised users that their data would remain private. Instead, it was monetized.
Here’s what happened: When users completed intake questionnaires asking about their mental health struggles, that data was packaged and sent to advertising platforms for targeted marketing. Users who confided that they were struggling with depression, anxiety, or trauma found themselves targeted with ads based on that vulnerability. Their most intimate psychological confessions became data points for profit.
This reveals a fundamental problem: HIPAA was never designed for the digital age. HIPAA regulations were written for traditional healthcare providers. Multinational tech corporations operating therapy platforms exist in a gray zone where enforcement is inconsistent, slow, and often toothless. By the time the FTC acted, millions of users had already had their data harvested and sold.
The BetterHelp case is not an anomaly—it’s a preview of an algorithmic dystopia. When therapy becomes a “product” delivered by a “platform,” the patient’s data becomes the real product being sold. The therapeutic frame—the sacred container of confidentiality and trust—is shattered beyond recognition.
The Deprofessionalization of the Therapist: From Healer to Technician
What happens to the therapist in this brave new world? The answer is grim: systematic deprofessionalization. The convergence of algorithmic platforms, insurance dictates, and the “evidence-based” fetish has reduced the therapist from a trained professional capable of deep relational work to something closer to a “mental health technician”—or worse, a “digital best friend.”
The Technician Model
In managed care and platform-based settings, the therapist is increasingly expected to function as a technician administering a standardized protocol. Clinical judgment—the hard-won ability to read between the lines, to sense what the patient cannot yet articulate, to navigate the deep waters of the unconscious—is dismissed as “unscientific.” The therapist’s years of training and accumulated wisdom are reduced to checkbox competencies.
This is a disaster for patients. Complex trauma, dissociative conditions, and personality structures cannot be healed by a protocol delivered by a technician. They require what the founders understood: a relationship capable of holding complexity over time.
The “Digital Best Friend” Model
Perhaps even more insidious is the push toward therapists as “digital best friends.” On text-based platforms, the therapist is expected to be available at all hours, responding to messages like a supportive friend. The professional boundary—the frame that makes therapy therapy rather than just a chat—dissolves.
This isn’t just bad for therapists (though it is—burnout rates among platform therapists are astronomical). It’s bad for patients. The containment of the therapeutic frame—the predictable time, the consistent space, the boundaried relationship—is itself healing. When you dissolve it into a 24/7 text exchange, you lose the very structure that makes deep work possible.
The Algorithmic Future: A Warning
We are careening toward a future where:
- AI “therapists” handle initial intake and even ongoing “sessions,” with human therapists supervising multiple AI-patient conversations simultaneously
- Patient data flows freely to advertising platforms, employers, and insurance companies, with “consent” buried in Terms of Service agreements nobody reads
- Therapists are ranked by algorithms based on “patient satisfaction” scores—incentivizing them to avoid the difficult confrontations that real therapeutic work sometimes requires
- HIPAA becomes entirely unenforceable against multinational corporations that operate across jurisdictions, settle FTC fines as a cost of doing business, and continue harvesting data
This is not speculation. Every element of this future already exists in embryonic form. The question is whether the profession will resist—or capitulate.
The Return of the Repressed
The Pendulum Swings Back: “Underlying Forces” Reclaimed
Just as the biomedical and commodified models seemed to achieve total dominance, a powerful counter-movement has emerged. Clinicians and patients alike have begun to reject the “symptom reduction” model in favor of models that acknowledge complexity, trauma, and the fragmentation of the self.
Internal Family Systems (IFS): The Neo-Plural Mind
Internal Family Systems (IFS), developed by Richard Schwartz, has exploded in popularity, challenging the DSM paradigm. IFS conceptualizes the patient not as having a pathology, but as containing a “family” of internal “Parts” (Exiles, Managers, Firefighters) led by a core “Self.”
The radical stance of IFS is that “there are no bad parts.” A symptom like addiction or cutting is not a disease; it is the behavior of a “Protector” part trying to save the system from pain. This replaces the “pathology” model with a “systemic” model. It returns to the depth of psychoanalysis (inner conflict) but frames it in non-shaming, accessible language.
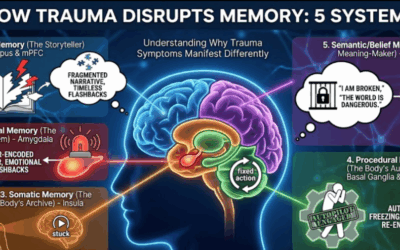
Trauma and the Body: “The Body Keeps the Score”
The immense cultural phenomenon of Bessel van der Kolk’s book The Body Keeps the Score signals a paradigm shift. As explored in my piece on The Path Forward for Trauma Treatment, van der Kolk argues that both the “talking cure” (CBT/Analysis) and the “drug cure” fail to address the physiological imprint of trauma.
The patient is conceptualized as a Body-Mind System. Trauma is not just a memory; it is a physiological state stuck in the nervous system. Models like Peter Levine’s Somatic Experiencing focus on “bottom-up” processing—discharging survival energy trapped in the body—rather than “top-down” cognitive control. This challenges the CBT notion that “changing thoughts changes feelings,” arguing instead that the body must feel safe before the mind can heal.
Gabor Maté and the Myth of Normal
Gabor Maté has become a leading voice critiquing the biomedical model’s isolation of the individual. In The Myth of Normal, Maté argues that “pathology” is often a normal response to an abnormal, toxic culture. He conceptualizes the patient as a “canary in the coal mine” of a sick society—echoing the themes I’ve explored in Healing the Modern Soul.
Psychedelics: Breaking the Maintenance Model
The renaissance of Psychedelic-Assisted Psychotherapy (MDMA, Psilocybin, Ketamine) poses a direct challenge to the “chronic maintenance” model of psychiatry. Unlike SSRIs, which suppress symptoms daily, psychedelics are used in conjunction with deep therapy to induce a breakthrough—a radical reorganization of the self. This model views the patient as capable of profound, rapid transformation through “mystical experience” and neuroplasticity, bridging the materialist and spiritual divides.
Brain-Based Approaches That Honor Depth
At our practice, we’ve found that approaches like Brainspotting, EMDR, and neuromodulation offer a middle path. These are genuinely brain-based therapies that take neuroscience seriously—but they don’t reduce the patient to a checklist. They work with the subcortical brain, the body, and the relational field. They understand that healing is not symptom elimination but integration.
Reclaiming the Soul of Therapy
The evolution of the patient from the Neurotic to the User reflects the broader trajectory of Western culture: a move from depth, tragedy, and complexity toward efficiency, quantification, and commodification. We have dismantled the “conflict” model of the soul in favor of the “deficit” model of the brain, and finally the “consumer” model of the marketplace.
However, the “material forces” that drove this—the insurance mandates for short-term care, the pharmaceutical drive for maintenance drugs, the academic pressure for “measurable” results—have created a system that manages symptoms but often fails to heal people. The “needle has not moved” on mental health outcomes, as Thomas Insel admitted.
The current resurgence of IFS, somatic therapies, and psychedelic medicine represents a grassroots rebellion. Patients are rejecting the “Checklist Identity” of the DSM. They are voting with their feet for therapies that honor their complexity, their bodies, and their “underlying forces.”
But we must be vigilant. The forces of commodification are relentless. The BetterHelp scandal was not an aberration—it was a preview. If we allow therapy to become just another gig-economy product, with therapists reduced to technicians and patients reduced to data points, we will have lost something precious and irreplaceable.
The founders understood something that our spreadsheet-driven age has forgotten: that the person sitting across from us is not a “user” or a “covered life” or a “diagnostic category.” They are a soul—complex, contradictory, yearning for meaning. And they deserve a therapist who has not been reduced to a technician, working in a system that has not been reduced to an algorithm.
As I wrote in Healing the Modern Soul: the path forward is not backward—we cannot return to the 1920s. But we can insist on integrating the wisdom of the past with the genuine advances of neuroscience. We can refuse the false choice between “scientific” and “humane.” We can demand a therapy that is both brain-based and soul-honoring.
The challenge for our profession is whether we can reintegrate these fragmented parts into a coherent whole—or whether we will allow the market to complete its dismemberment of the therapeutic relationship. The patients are watching. The future is not yet written.
The Evolution of Patient Conceptualization:
| Decade | Concept | Key Terms | Mechanism | Material Driver | Brain-Mind |
|---|---|---|---|---|---|
| 1900-1930s | The Neurotic | Unconscious, Repression, Drive | Insight, Catharsis | Private Practice, Urban Elite | Mind (Psychic conflict) |
| 1940s-1950s | The Client | Self-Actualization, Growth | Relationship, Empathy | GI Bill, University Expansion | Self (Humanistic) |
| 1960s-1970s | The Organism | Conditioning, Reinforcement | Re-learning, Desensitization | Demand for Efficiency | Behavior (Black box) |
| 1980s | The Disorder | Criteria, Comorbidity | Diagnosis & Medication | DSM-III, Insurance | Category (Atheoretical) |
| 1990s | The Consumer | Chemical Imbalance, Medical Necessity | Biological Correction (SSRI) | Managed Care, Pharma | Brain (Chemical) |
| 2000s | The Evidence-Based | Manualized, Protocol | Cognitive Restructuring | Academic Tenure/Grants | Cognition (Computer) |
| 2010s | The User | Access, On-Demand, Text | Algorithmic Matching | Gig Economy, Venture Capital | Data (Quantified self) |
| 2020s | The System | Parts, Self, Trauma, Somatic | Integration, Embodiment | Dissatisfaction with Outcomes | Body-Mind System |




















0 Comments